Cardiology — MCQs

On this page
Cardiomyopathy may be seen in all of the following conditions except?
What is the drug of choice in Chagas disease?
Which of the following is not included in acute coronary syndrome?
In Valvular Aortic Stenosis, when is the prognosis poorest?
A patient presents with an ECG showing ST elevation and low blood pressure. What is the best immediate management?
Protein losing enteropathy is seen in which of the following conditions?
Which of the following ECG changes is NOT typically seen in hyperkalemia?
Rapid X descent is unlikely in which of the following conditions?
Stokes-Adams syndrome is associated with which of the following conditions?
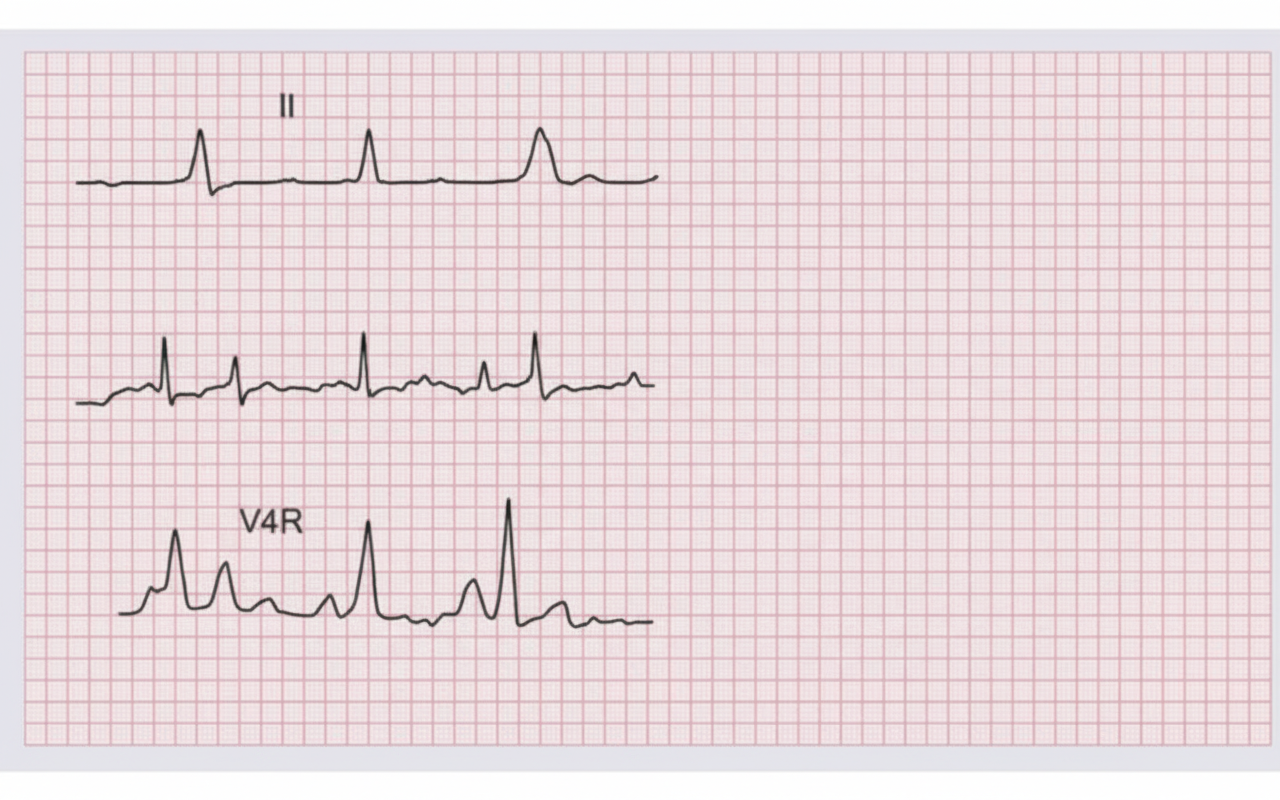
A 65-year old man presents with crushing chest pain for 2 hours. On examination, BP = 80/60 mm Hg and JVP are elevated 4 cm above the sternal angle. All are true about the condition shown except?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
