Cardiology — MCQs

On this page
A 57-year-old man presents with sudden onset of severe and central chest pain radiating to the back. ECG shows ST segment elevation in leads V1-V6, I, aVL. The chest X-ray shows a widened mediastinum. What is the most likely diagnosis?
A 65-year-old hypertensive male presented to the ER with sudden onset of severe, tearing pain in the back of the chest, more so in the interscapular region. He also experienced dyspnea, hemiplegia, hemianesthesia, and frequent episodes of syncope in the past 2 days. On examination, the patient was hypotensive with feeble pulses in bilateral radial arteries, a wide pulse pressure, and a diastolic murmur radiating towards the right sternal border. All of the following are true about the condition except:
All of the following are true for mitral valve prolapse, except?
A systolic thrill in the left 2nd and 3rd intercostal space may be seen in all of the following conditions, except?
All of the following are true about Right Ventricular Infarcts, except?
Hypotension with muffled heart sounds and congested neck veins is characteristic of which condition?
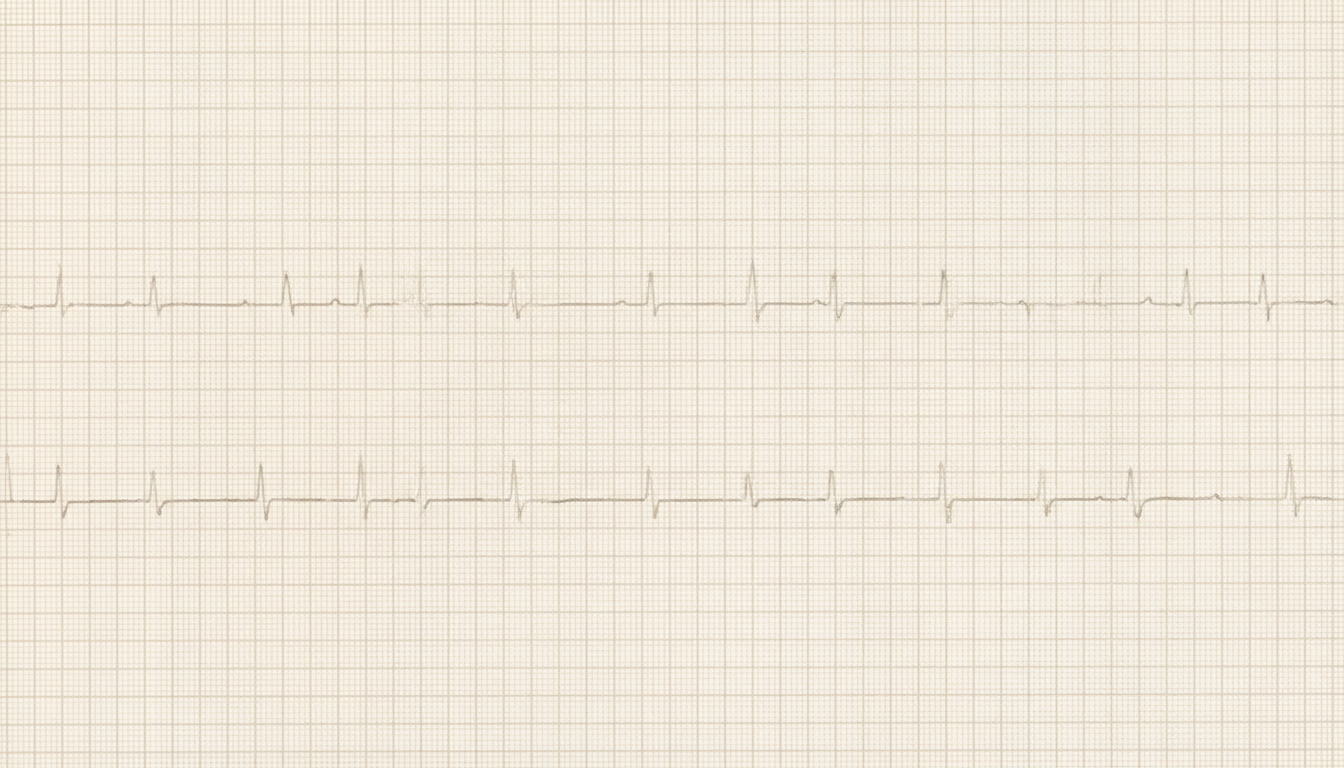
A 68-year-old woman presents to the emergency department complaining of chest pain for the past 30 minutes. The pain is retrosternal in location and it radiates to her neck. She has no history of cardiac conditions or similar episodes of chest discomfort, and her past medical history includes hypertension and dyslipidemia. On physical examination, she is diaphoretic and in moderate distress. The blood pressure is 150/90 mm Hg, the heart sounds are normal, and the lungs are clear on auscultation. The ECG is shown in Figure below. Which of the following mechanisms is the most likely cause of her condition?
The square root sign on abnormal ventricular filling is characteristic of which condition?
Eight days after undergoing a hysterectomy, a 64-year-old woman complains of chest pain. After 12 hours, which test will most likely support the diagnosis of myocardial infarction?
Which of the following valvular lesions is usually NOT seen in rheumatic heart disease?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
