Cardiology — MCQs

On this page
What is the most common parasite causing myocarditis?
What is the management of uncomplicated essential hypertension?
Which of the following is a common risk factor for coronary heart disease, except?
Which valvular lesion is being repaired in a 20-year-old man presenting with a malar flush?
Pulsus paradoxus is seen in all except?
A young patient presents with a systolic murmur at the apex. The murmur increases with both handgrip and Valsalva maneuver. Which of the following conditions is most likely?
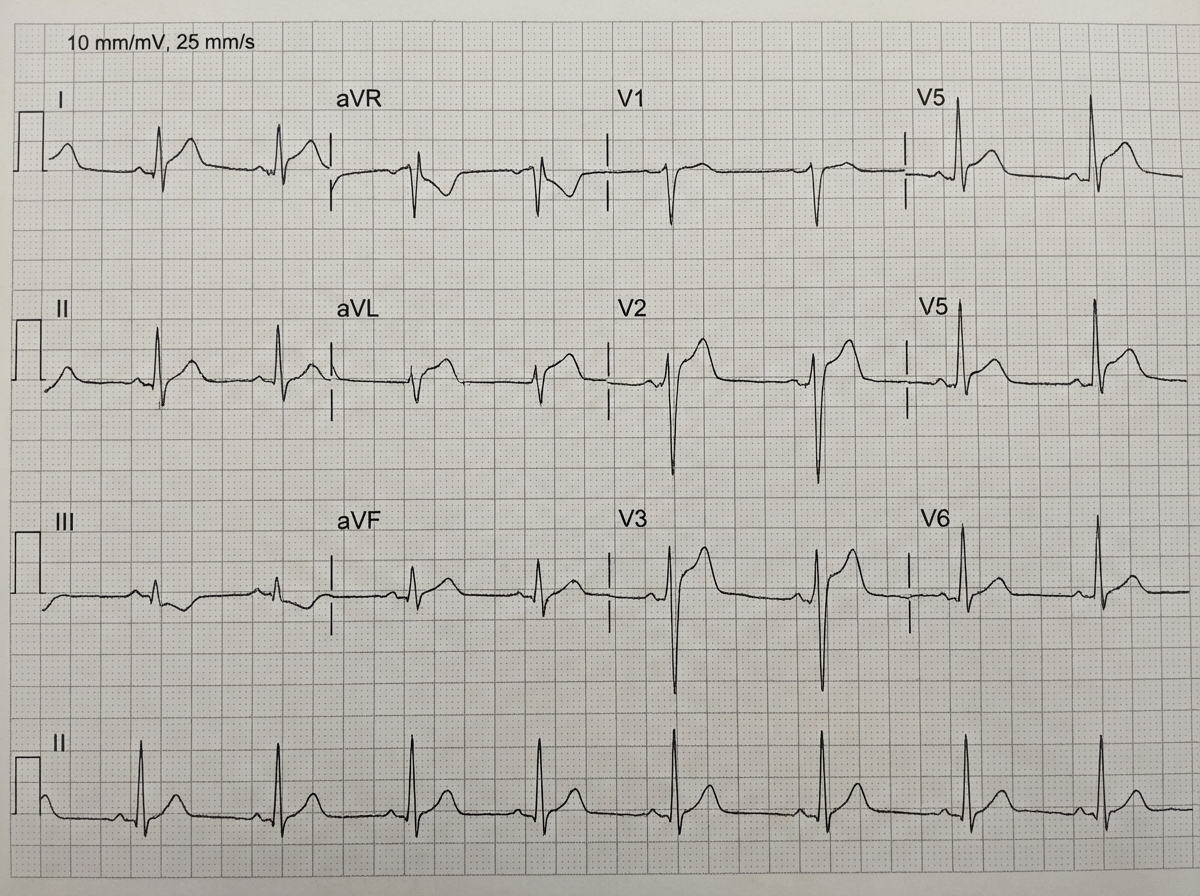
A 38-year-old man develops severe retrosternal chest pain radiating to the back, aggravated by breathing and movement. He has no significant past medical history but had a mild upper respiratory tract infection 1 week ago. His electrocardiogram is shown in Figure. Which of the following is the most likely cause for his condition?
Pulsus paradoxus is characteristically seen in cardiac tamponade. Absence of pulsus paradoxus is seen when cardiac tamponade is associated with all except one of the following?
Which of the following dietary interventions reduces the further risk in patients who have had a myocardial infarction (MI)?
Beck's triad of cardiac tamponade includes all except?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
