Cardiology — MCQs

On this page
Resistant hypertension is when the goal blood pressure is not achieved with:
Which of the following is a supraventricular tachycardia?
In severe aortic stenosis, which of the following is a true finding?
Which drug is used in unstable angina to prevent myocardial infarction?
J waves (Osborn waves) on ECG are seen in all of the following conditions EXCEPT:
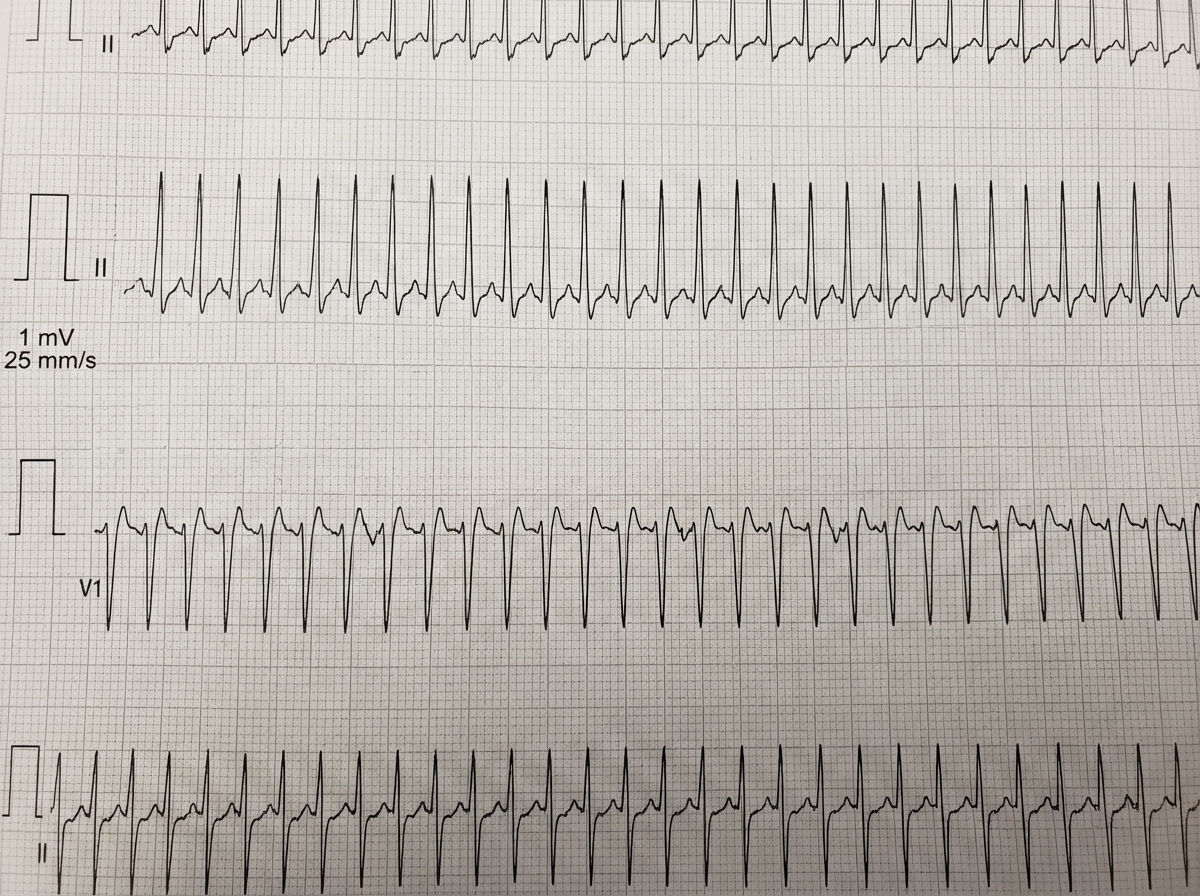
A 36-year-old female presents with a sensation of fast heart rate, slight dizziness, and vague chest fullness. Blood pressure is 110/70. The following rhythm strip is obtained, which shows?
A patient presents 12 hours following a Myocardial infarction. What is the test of choice?
A 37-year-old woman presents with shortness of breath on exertion. She has a past history of rheumatic fever as a child. On cardiac auscultation, there is a loud S1 and a mid-to-late low-pitched diastolic murmur. Which of the following findings is most likely to be seen on the chest X-ray in someone with mitral stenosis?
A 62-year-old man with carcinoma of the lung presented to the emergency department with respiratory distress. His ECG showed electrical alternans. What is the most likely diagnosis?
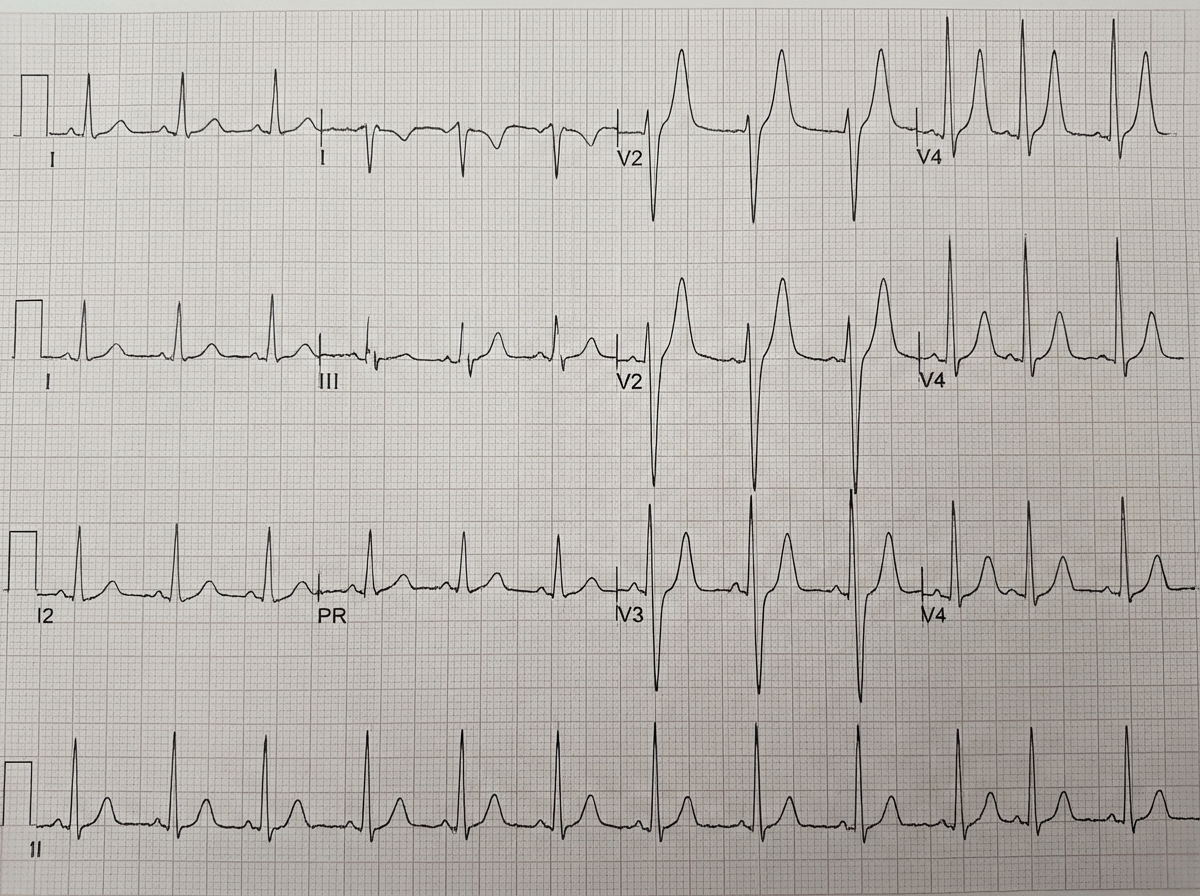
Which electrolyte imbalance is shown in the following ECG?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
