Cardiology — MCQs

On this page
Inoue balloon is used in the treatment of which condition?
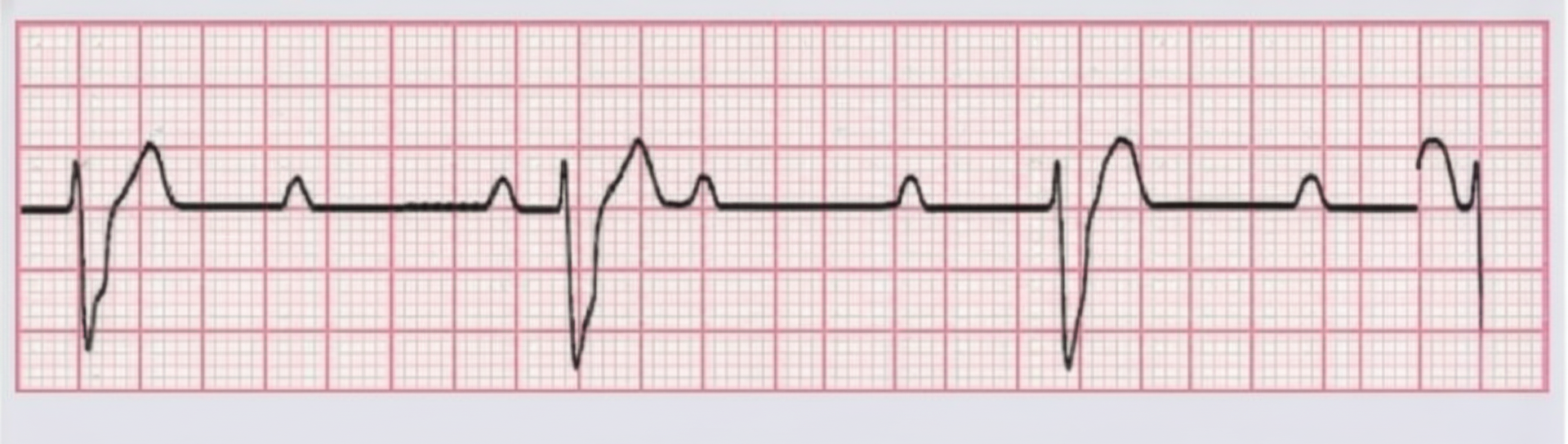
Ventricular ectopic beats are represented by which of the following findings?
What is the most common complication of infective endocarditis?
In a hospital cardiac care unit, there are three patients with different cardiac conditions: a 52-year-old man with dilated cardiomyopathy, an 18-year-old girl with mitral valve prolapse, and a 30-year-old man with infective endocarditis of the mitral valve. Which of the following features do all these patients most likely share?
Which of the following physical signs is seen in a patient with severe aortic stenosis?
Which of the following lesions is not a common cause for vegetation formation in the heart?
A midsystolic click is a characteristic feature of which condition?
A 55-year-old female presented to the ER with sudden onset of shortness of breath along with syncope. Chest X-ray was unremarkable. ECG was done. On examination, some skin lesions were observed. What is the most likely diagnosis in this case?
A 68-year-old man who has had a recent syncopal episode is hospitalized with congestive heart failure. His blood pressure is 160/80 mmHg. His pulse rate is 80 beats per minute, and there is a grade III/IV harsh systolic murmur. An echocardiogram shows a disproportionately thickened ventricular septum and systolic anterior motion of the mitral valve. Which of the following findings would most likely be present in this man?
Which ECG feature is characteristic of acute cor pulmonale, such as that caused by pulmonary embolism?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
