Cardiology — MCQs

On this page
Increased AV nodal blockade leads to termination of tachycardia in all except?
Which of the following is the most common complication of heart failure?
What is the most common cause of shock in myocardial infarction?
What is the cause of essential (Primary) Hypertension?
What is a main disadvantage of stenting?
Which of the following is the most common complication of asymptomatic atrial fibrillation?
Which condition typically requires a rapid reduction of blood pressure?
All of the following are seen in cardiac tamponade except:
Which of the following is true about malaria?
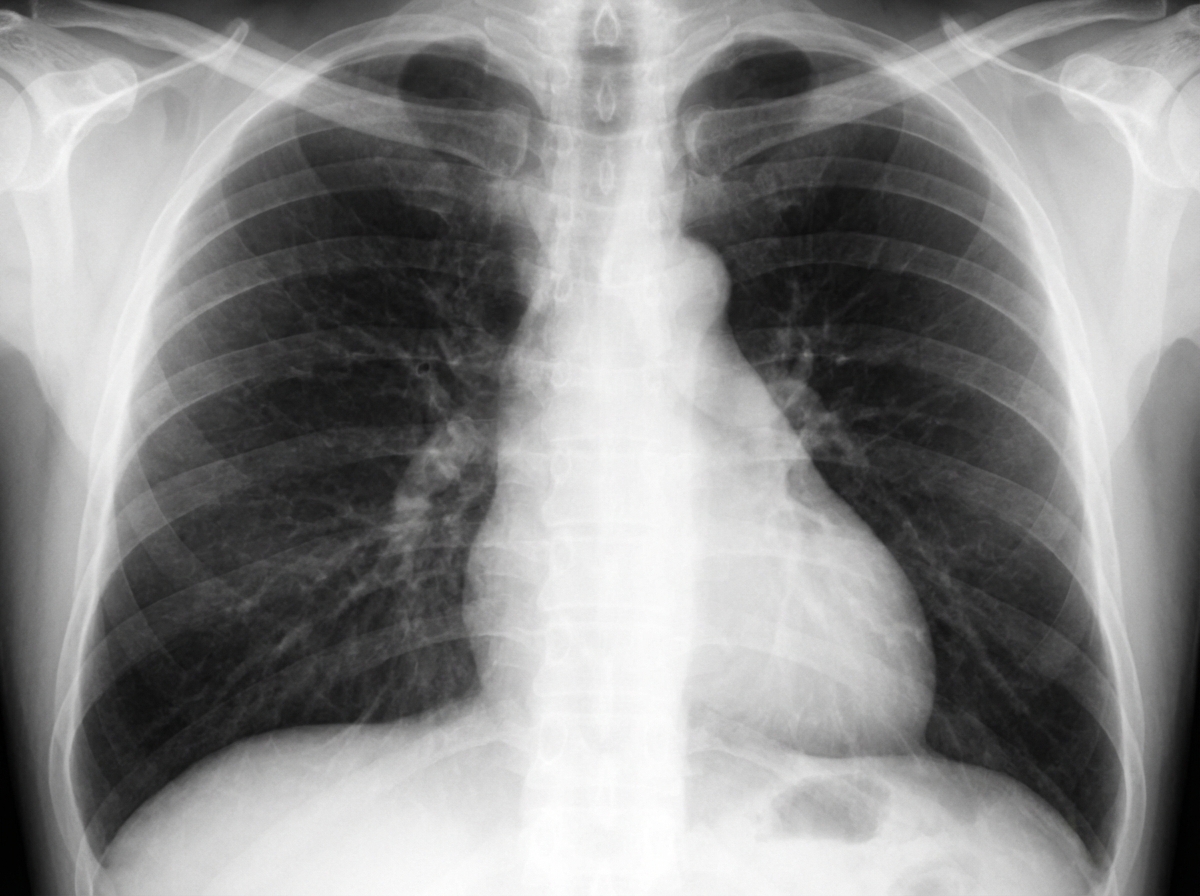
A 41-year-old male schoolteacher, a nonsmoker, presents with lightheadedness, shortness of breath, "lack of stamina," and chest pain. On physical examination, vital signs are normal. The patient is overweight with a BMI of 33. Cardiovascular examination reveals a left parasternal heave, a harsh grade 3/6 systolic flow murmur, and a loud P2 sound. Chest radiographs are shown. What is the most likely diagnosis?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
