Cardiology — MCQs

On this page
A 42-year-old man presents with dizziness on standing. His systolic blood pressure falls by 50 mm Hg and his heart rate is 52/min. What is the likely cause?
Giant a waves in JVP are seen in which of the following conditions?
Comment on the ECG finding shown below?
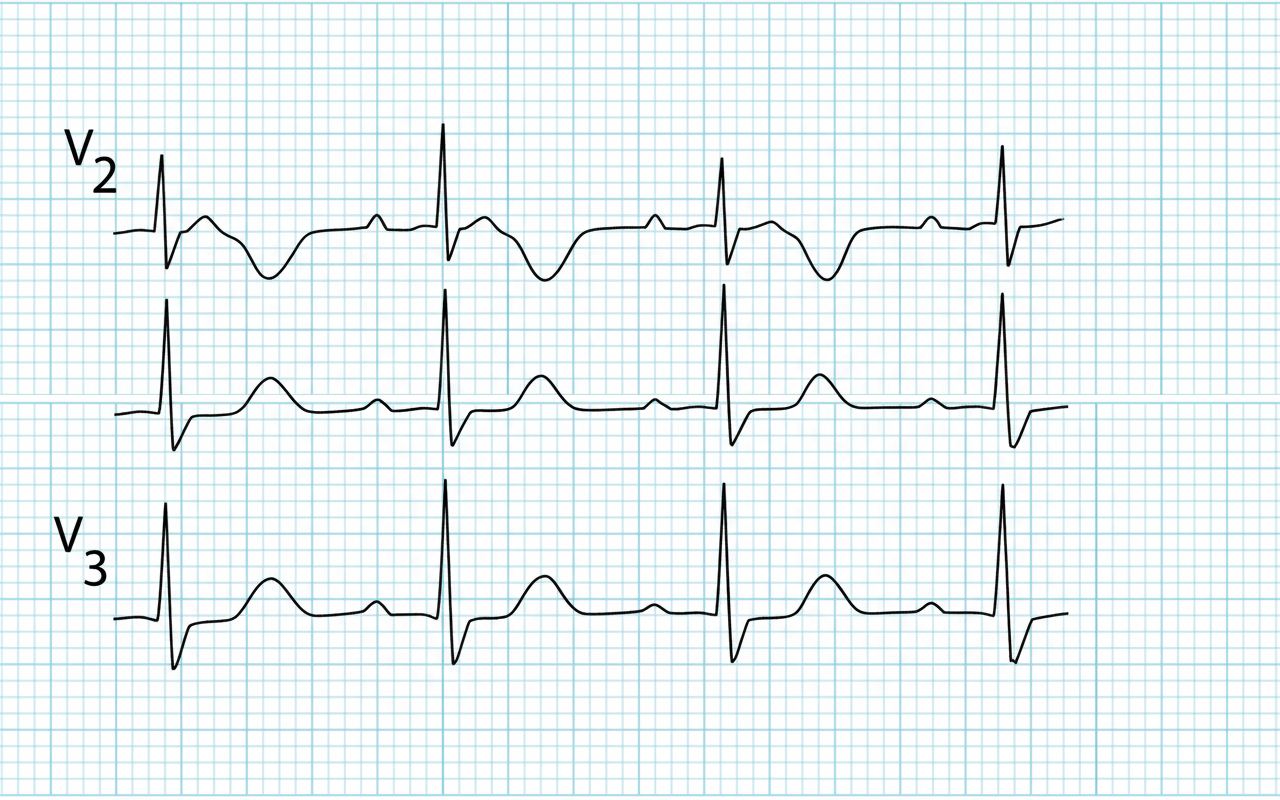
A 55-year-old female presents with Levine sign, hiccups, and vomiting episodes. On examination, HR=50/min with BP =100/60 mm Hg with elevated JVP. ECG technician is yet to arrive. Which coronary artery is likely to be involved?
Which of the following is the most common cause of midsystolic murmur in adults?
Which condition is most likely associated with the given ECG tracing?
All of the following predispose to Ischemic Heart Disease except?
What is the most common valvular lesion seen with carcinoid syndrome?
Wolff-Parkinson-White (WPW) syndrome is characterized by which of the following electrocardiographic findings?
Which one of the following is of most serious prognostic significance in a patient of essential hypertension?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
