Cardiology — MCQs

On this page
Congenital long QT syndrome has a tendency to develop which of the following conditions?
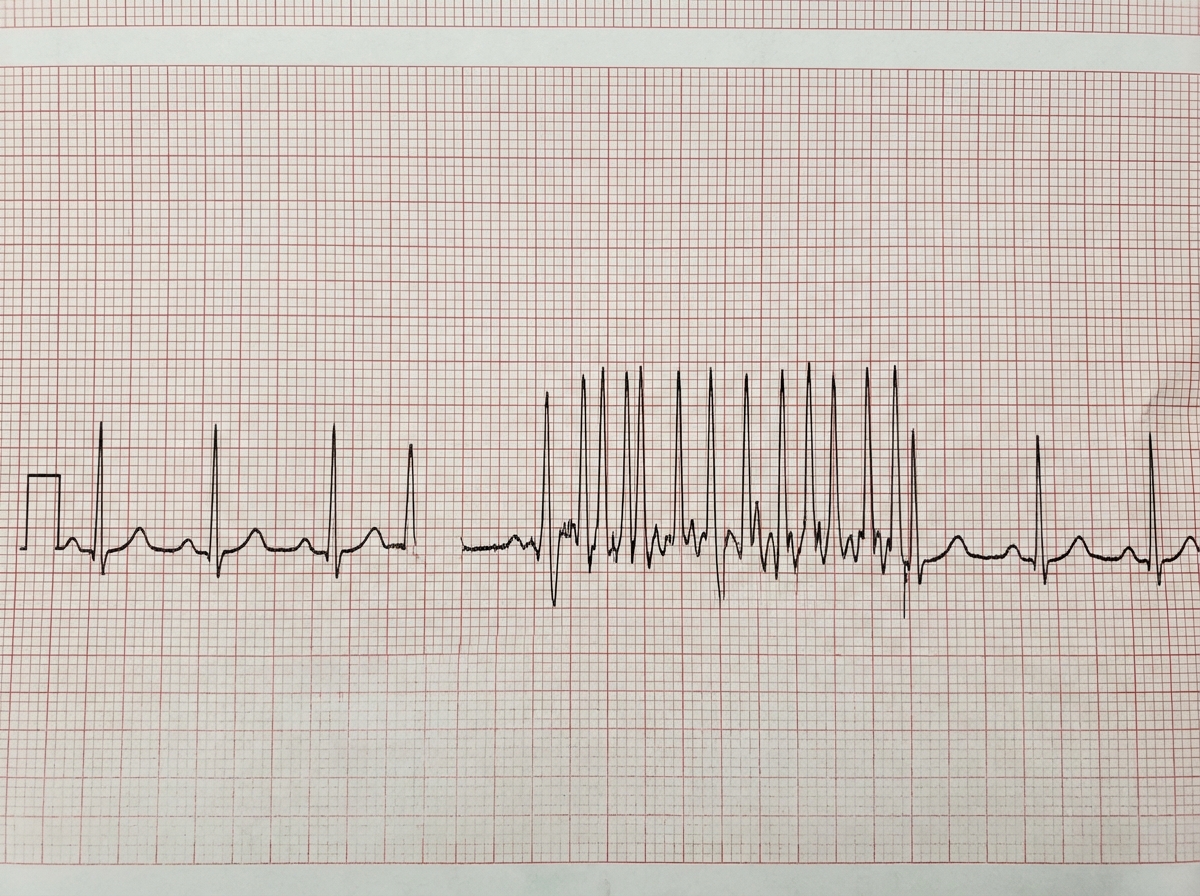
A 50-year-old patient complains of dizziness and palpitations. What does the ECG show?
What are the causes of constrictive pericarditis?
Which of the following is true regarding neurocardiogenic syncope?
All of the following features suggest broad complex ventricular tachycardia except:
What is the earliest feature of pulmonary venous hypertension?
Beck's triad of cardiac tamponade includes:
A patient develops sudden palpitation with a heart rate of 150 beats per minute, which is regular. What is the most likely cause?
A 35-year-old athlete with a height of 184 cm, arm span of 194 cm, pulse rate of 64/min, and BP of 148/64 mm Hg presents with a long diastolic murmur heard over the right second intercostal space on routine chest auscultation. What is the probable diagnosis?
Which of the following conditions is associated with a QRS duration greater than 0.16 seconds?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
