Cardiology — MCQs

On this page
What is the first-line drug of choice for acute pulmonary edema?
Which of the following is an absolute contraindication for exercise testing?
What is true about the third heart sound (S3)?
What is the treatment for orthostatic hypotension?
Dressler's syndrome is due to:
What is the initial pharmacological treatment for sinus bradycardia in the context of myocardial infarction?
A 73-year-old woman has had episodes of chest pain during the past week. She is afebrile. Her pulse is 80/min, respirations are 16/min, and blood pressure is 110/70 mm Hg. On auscultation of the chest, heart sounds seem distant, but the lung fields are clear. Neck veins are distended to the angle of the jaw, even while sitting. There is a darkly pigmented, irregular, 1.2-cm skin lesion on the right shoulder. A chest radiograph shows prominent borders on the left and right sides of the heart. Pericardiocentesis yields bloody fluid. Laboratory findings include a serum troponin I level of 0.3 ng/mL. Which of the following lesions is the most likely cause of these findings?
Which of the following statements is TRUE in diastolic dysfunction of the left ventricle?
A 45-year-old man presents with central chest pain for 4 hours. Troponin I is 0.8 ng/dL. What is the diagnosis?
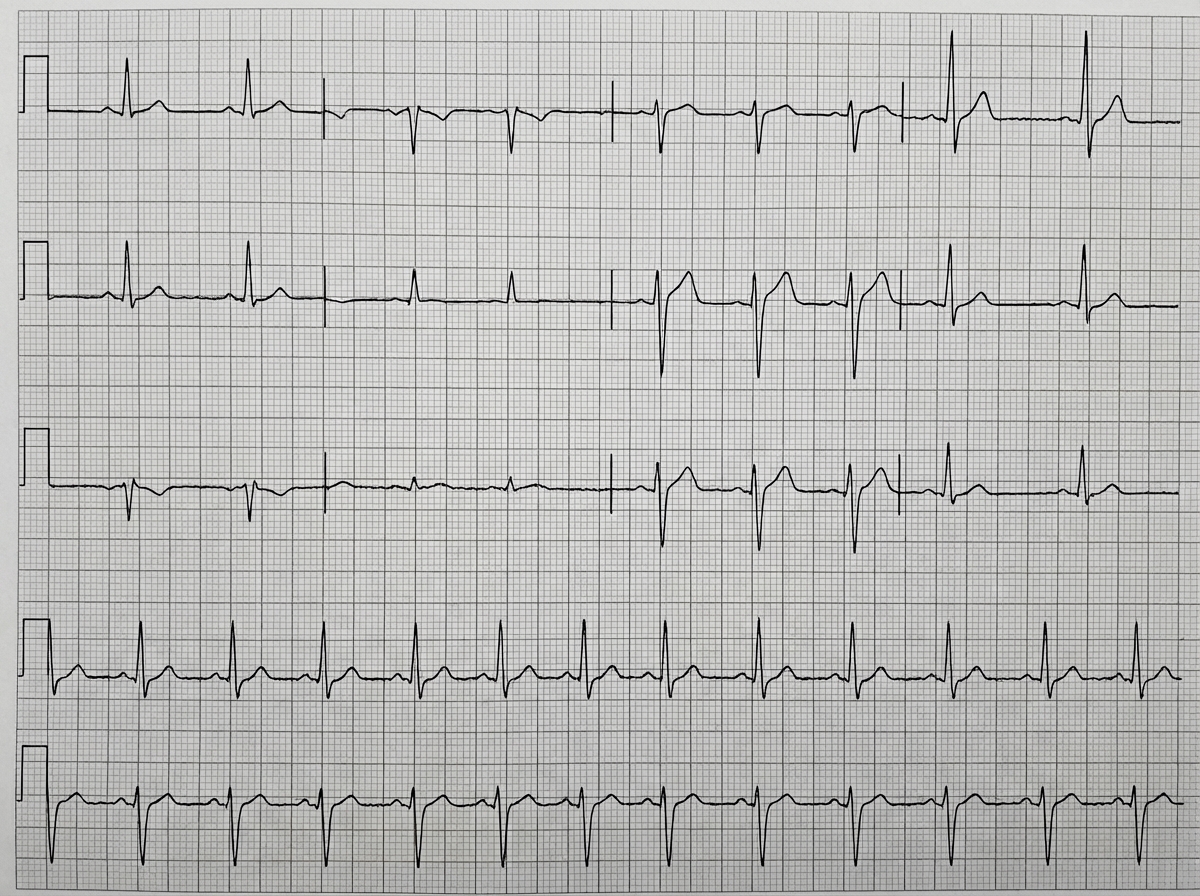
All of the following are true about Atrial Fibrillation, except?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
