Cardiology — MCQs

On this page
Which of the following is a risk factor for atherosclerosis?
Which condition is characterized by a 'hockey-stick' appearance on echocardiography?
Which of the following statements about blood pressure measurement is INCORRECT?
ST depression and T wave inversion in V1 to V6 and aVL leads indicate:
A patient in CCU on day 2 of PCI procedure has the following rhythm. BP=90/60mmHg. Which is the next best step for management of this patient?
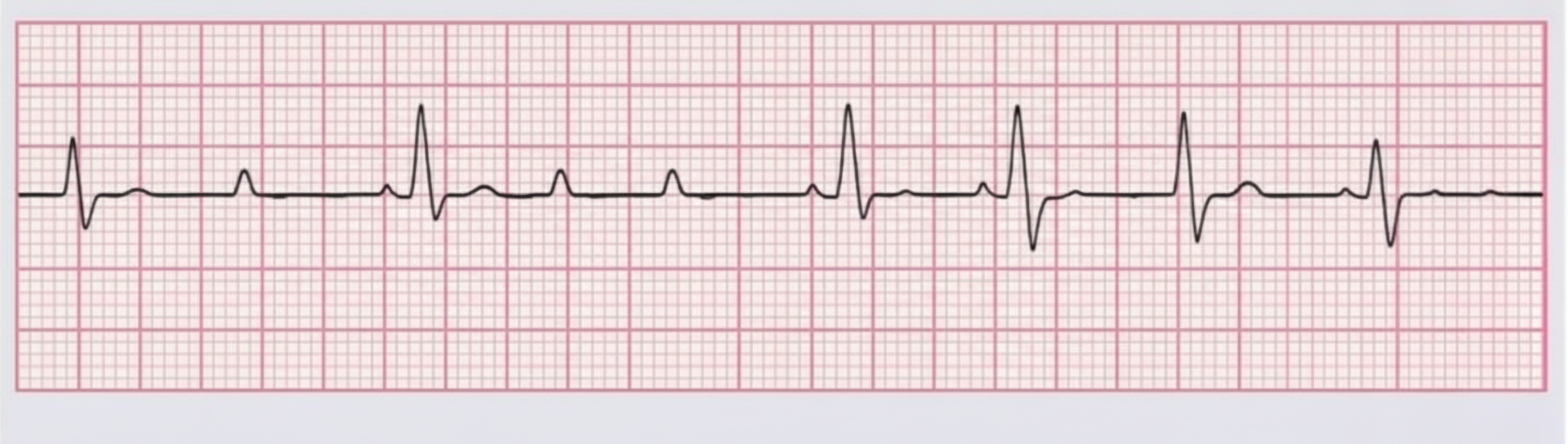
Postural orthostatic tachycardia syndrome is characterized by all EXCEPT?
What condition is associated with the presence of Visser's sign?
Reduced risk of cardiovascular disease is associated with all of the following EXCEPT:
A 56-year-old man presents with severe chest pain and difficulty in breathing. An immediate ECG was taken. What diagnosis does the ECG suggest?
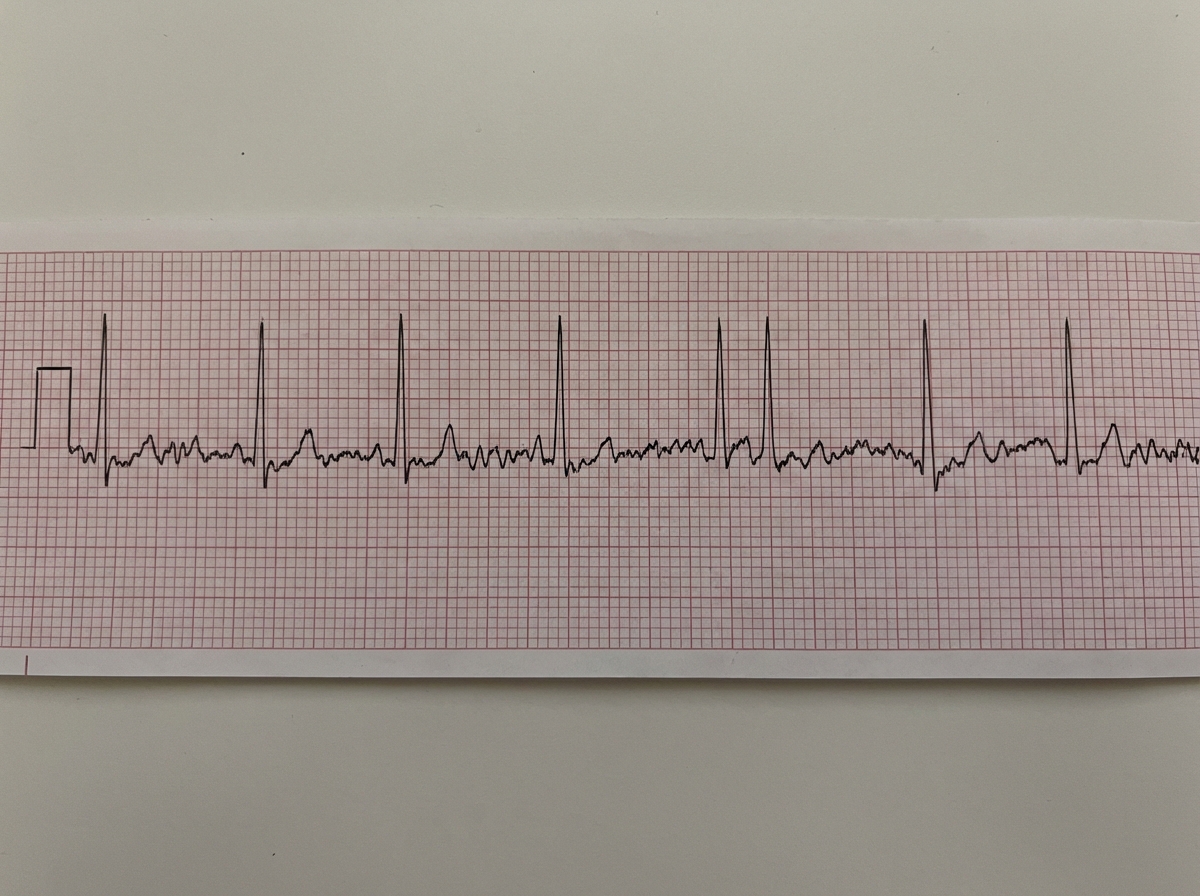
What is the best modality of treatment for a patient with acute inferior wall myocardial infarction?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
