Cardiology — MCQs

On this page
Turner syndrome is maximally associated with ?
Erb's Point in cardiology refers to:
Which of the following is the MOST common complication of untreated hypertension?
A hypertensive patient who is non-compliant with medication presents to you with sudden onset breathlessness. A chest x-ray was done, which is shown below. How will you manage this patient?
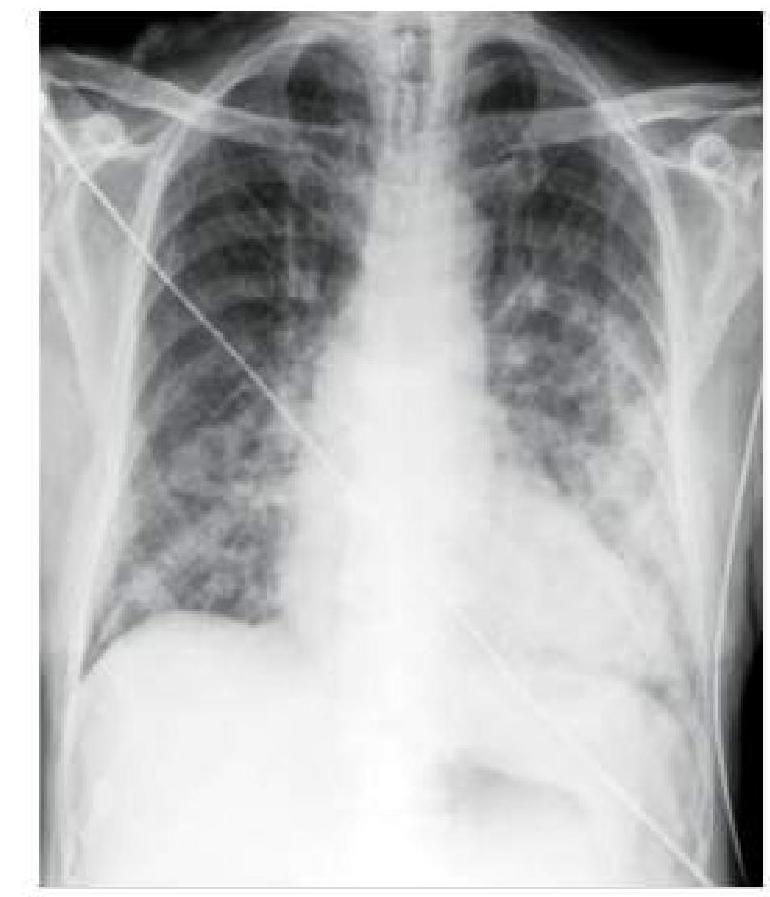
What is the normal range for the QRS axis in degrees?
Vegetation in mitral valve seen in which condition
Which of the following statements is true about the Bundle of Kent?
Osborn J waves are seen in which of the following conditions?
A patient presents to you with an irregularly irregular pulse of 120/minutes and a pulse deficit of 20. Which of the following would be the jugular venous pressure (JVP) finding?
What is the most appropriate immediate management for a hemodynamically unstable patient with supraventricular tachycardia (SVT)?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
