Cardiology — MCQs

On this page
Bacterial endocarditis can cause all of the following except:
Which of the following can cause a soft first heart sound (S1)?
A patient post myocardial infarction develops atrial fibrillation. Subsequently, echocardiography shows a mural thrombus. What is the recommended management?
Constrictive pericarditis is associated with each of the following except?
All are true about hypertrophic obstructive cardiomyopathy except?
A patient with an atrial septal defect (ASD) presents with a murmur similar to mitral regurgitation and left axis deviation of 40 degrees. What is the likely diagnosis?
What is the most common cause of right ventricular failure?
What is Wenckebach phenomenon?
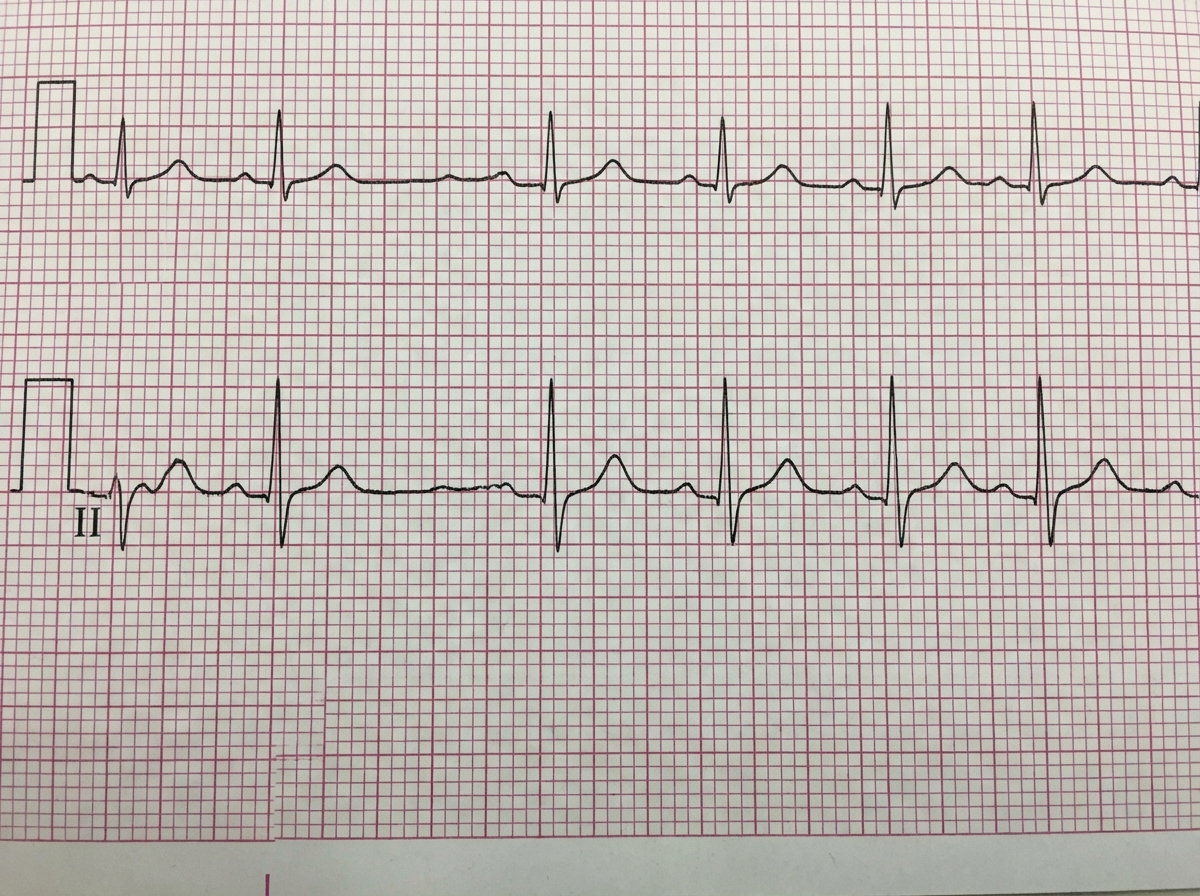
The following ECG represents?
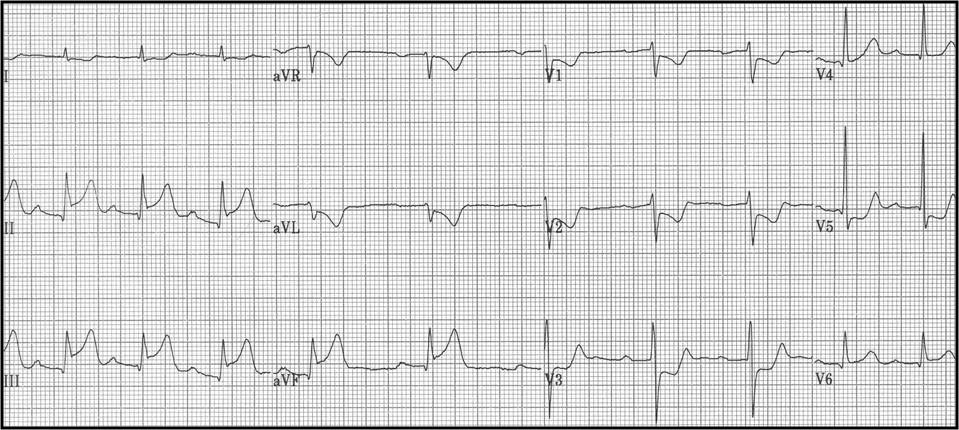
Comment on the diagnosis from the ECG shown below?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
