Cardiology — MCQs

On this page
What is the most common sustained tachycardia in healthy young women?
Which of the following is NOT a management or diagnostic modality for Wolff-Parkinson-White syndrome?
Which of the following conditions causes heart failure with reduced ejection fraction?
Which of the following ECG findings in an asymptomatic athlete's heart should be considered pathological?
A 45-year-old tall, thin male presents with acute onset of chest pain radiating into the back. In the emergency room, his right radial pulse is bounding, but his femoral pulses are absent. What is the most likely diagnosis?
A 30-year-old male presents with severe chest pain, breathlessness, and hypotension. ECG shows ST elevation in V3, V4, V5, and V6 leads. What is the best treatment for this patient?
A 65-year-old man is about to undergo an elective hip replacement. A pre-operative ECG is taken. Based upon the ECG, which of the following jugular venous pressure (JVP) abnormalities is most likely to be present?
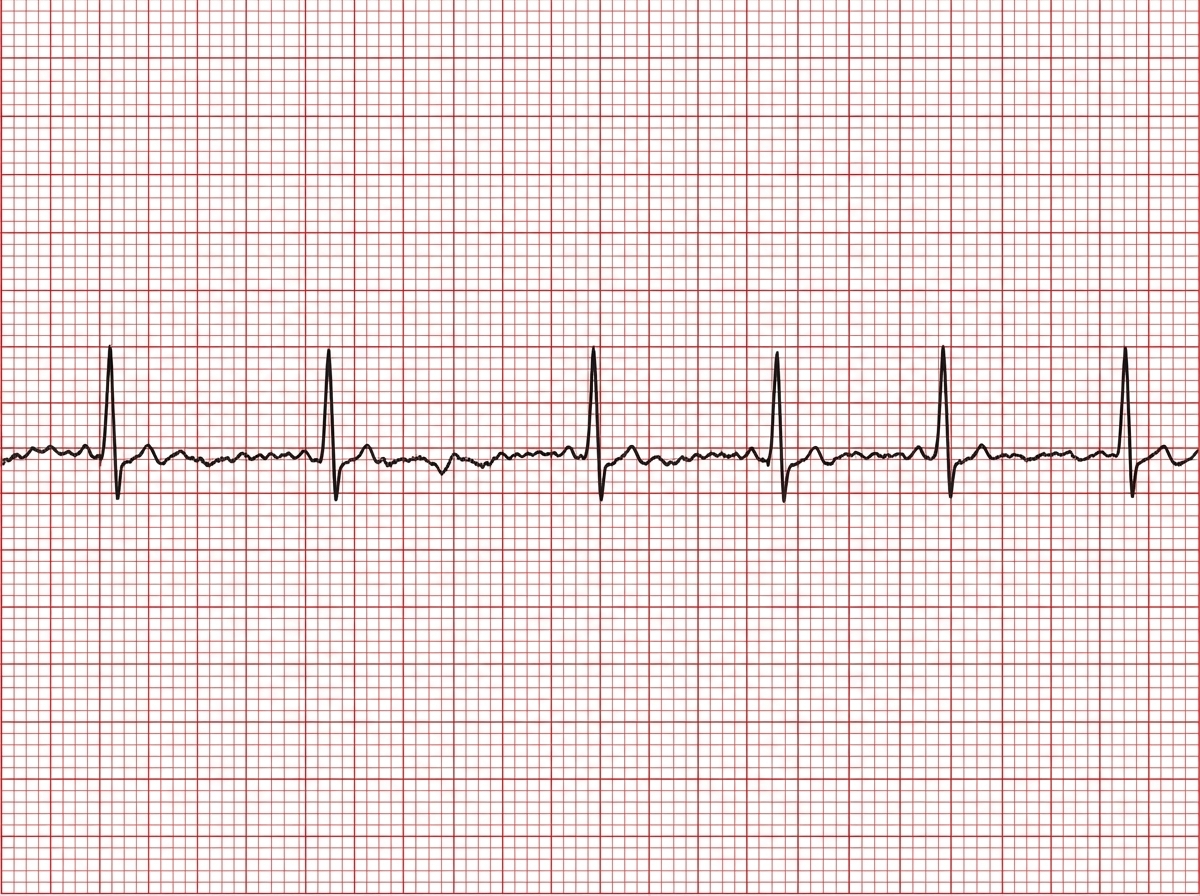
Electrical alternans in ECG is characteristic of which condition?
Malignant hypertension can lead to all of the following except?
A 48-year-old male patient with an anterior myocardial infarction underwent primary angioplasty with a bare metal stent. What duration of antiplatelet therapy will you advise for discharge?
Practice by Chapter
Coronary Artery Disease and Angina
Practice Questions
Acute Coronary Syndromes
Practice Questions
Heart Failure
Practice Questions
Cardiac Arrhythmias
Practice Questions
Valvular Heart Diseases
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Hypertension and Hypertensive Emergencies
Practice Questions
Pulmonary Hypertension
Practice Questions
Non-invasive Cardiac Diagnostics
Practice Questions
Preventive Cardiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
