Diseases of the Oral Cavity and Salivary Glands — MCQs

On this page
Which of the following statements is false regarding plunging ranula?
According to Eversole theory, which of the following is NOT a tumor arising from reserve cells of the intercalated ducts of salivary glands?
Noma is:
Ludwig's angina is defined as:
A palatal abscess most commonly results from an infection of which of the following teeth?
Leukoplakia with the worst prognosis is typically found on which of the following locations?
What percentage of sublingual salivary gland tumors is malignant?
Mixed parotid tumor arises from which tissue types?
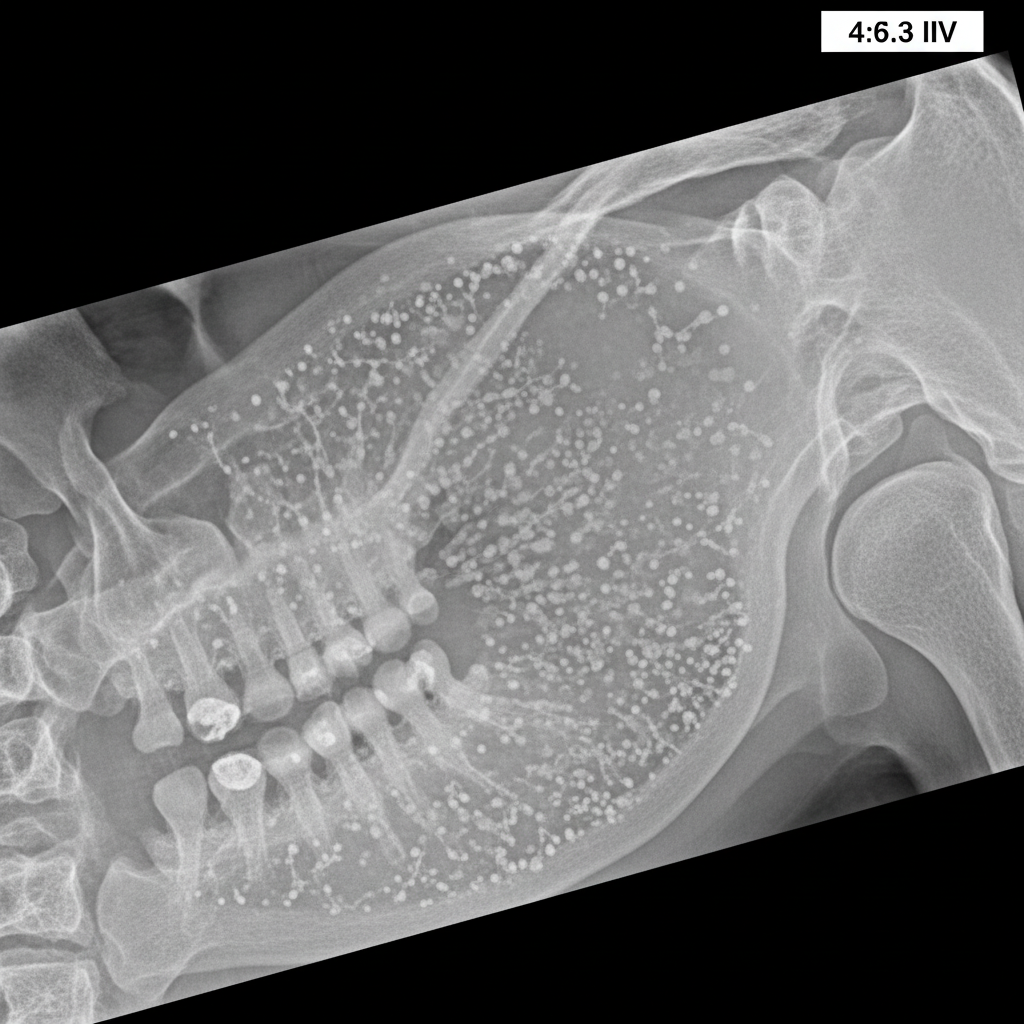
A sialography report of a 46-year-old female is provided. Based on the findings, what is the most likely diagnosis?
What is the characteristic ENT manifestation of Peutz-Jeghers syndrome with benign intestinal polyps?
Practice by Chapter
Stomatitis
Practice Questions
Oral Ulcers
Practice Questions
Oral Leukoplakia
Practice Questions
Oral Cancers
Practice Questions
Sialadenitis
Practice Questions
Sialolithiasis
Practice Questions
Salivary Gland Tumors
Practice Questions
Ranula
Practice Questions
Xerostomia
Practice Questions
Sjögren's Syndrome
Practice Questions
Oral Manifestations of Systemic Diseases
Practice Questions
Temporomandibular Joint Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
