Diseases of the Nose and Paranasal Sinuses — MCQs

On this page
A 35-year-old male presented with nasal discharge, facial pain, and fever, which subsided with a course of antibiotics and antihistamines but recurred again after 2 months. On examination, there was mucopurulent discharge from the middle meatus and inflamed sinus openings. What is the investigation of choice?
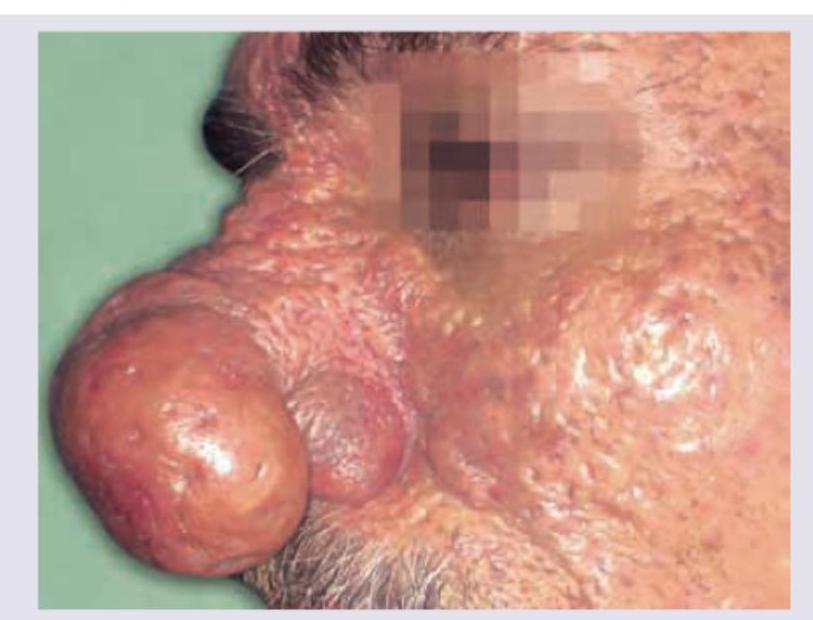
A patient presented with the following symptoms. What is the etiopathogenesis of the disease process?
What is the most common intracranial complication of chronic sinusitis?
Which of the following are complications of acute sinusitis?
Howah operation is done for which condition?
Which of the following conditions does not lead to septal perforation?
Nasal septum perforation occurs in all of the following except?
What is the most common cause of epistaxis in children?
The Killian term is used for which of the following polyps?
Maxillary sinusitis due to viral etiology is:
Practice by Chapter
Rhinitis
Practice Questions
Acute Rhinosinusitis
Practice Questions
Chronic Rhinosinusitis
Practice Questions
Nasal Polyposis
Practice Questions
Allergic Fungal Sinusitis
Practice Questions
Deviated Nasal Septum
Practice Questions
Epistaxis
Practice Questions
Nasal Trauma
Practice Questions
Choanal Atresia
Practice Questions
CSF Rhinorrhea
Practice Questions
Tumors of the Nose and Paranasal Sinuses
Practice Questions
Complications of Sinusitis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
