Diseases of the Nose and Paranasal Sinuses — MCQs

On this page
Identify the device shown in the image below:
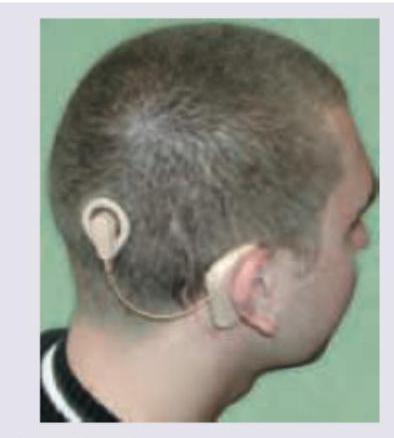
The image shows presence of the following:
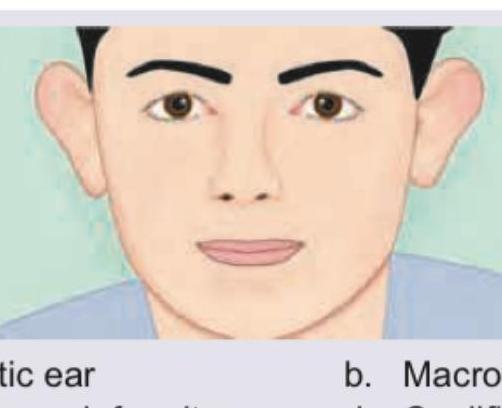
Which one of the following regarding Nasal polyps is NOT true?
Antro-choanal polyp always arises from:
Which sinus drainage is impaired in the following image?
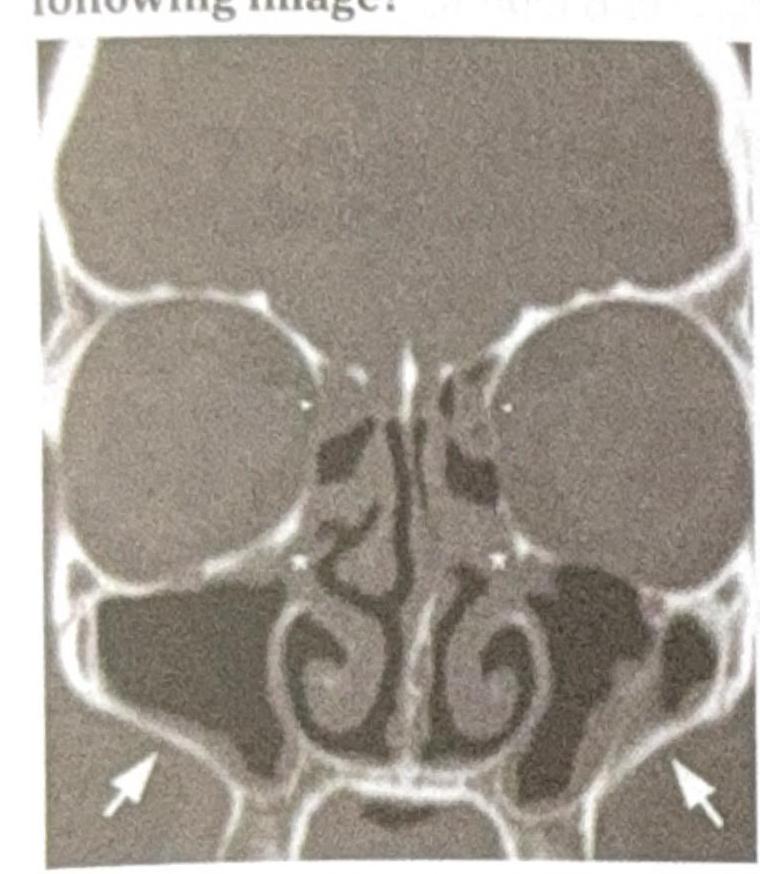
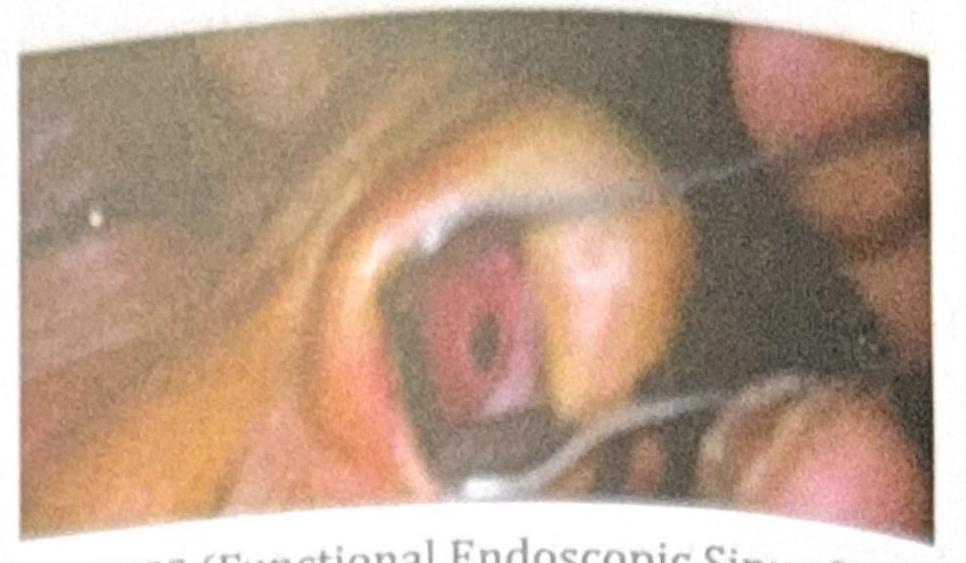
A 14-year-old child with a history of recurrent nasal bleeding has the endoscopic view provided. What is the investigation of choice?
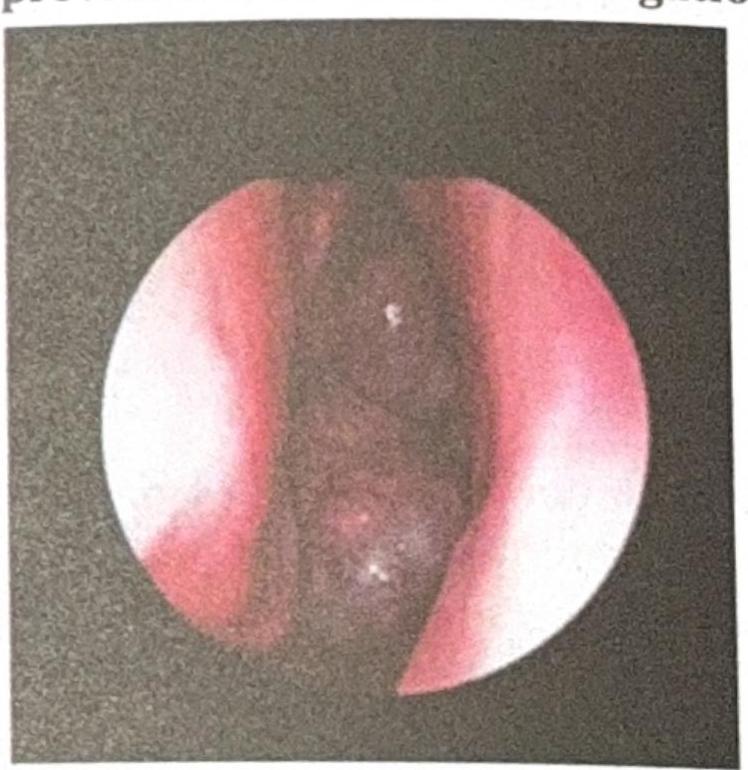
A patient with chronic nasal obstruction underwent a procedure 3 months ago and now presents with recurrent epistaxis, crusting, and the clinical image showing a septal perforation. What procedure was most likely carried out?
A woman visits the ENT outpatient department with complaints of nasal obstruction. On examination, greenish-black crusts were found in the nasal cavity covering the turbinates and septum, and she also had complete anosmia (lack of sense of smell). What other sign is most likely to be found on examination in this case?
A 35-year-old female patient presents with complaints of nasal obstruction and post-nasal drip. There is a past history of FESS for failed conservative management 5 years ago. Uncinectomy and maxillary ostium dilation was done during the previous FESS. A DNE done now shows patent ostia and mucosal edema of the maxillary sinus lining. What is the next best step in management? FESS - Functional endoscopic sinus surgery
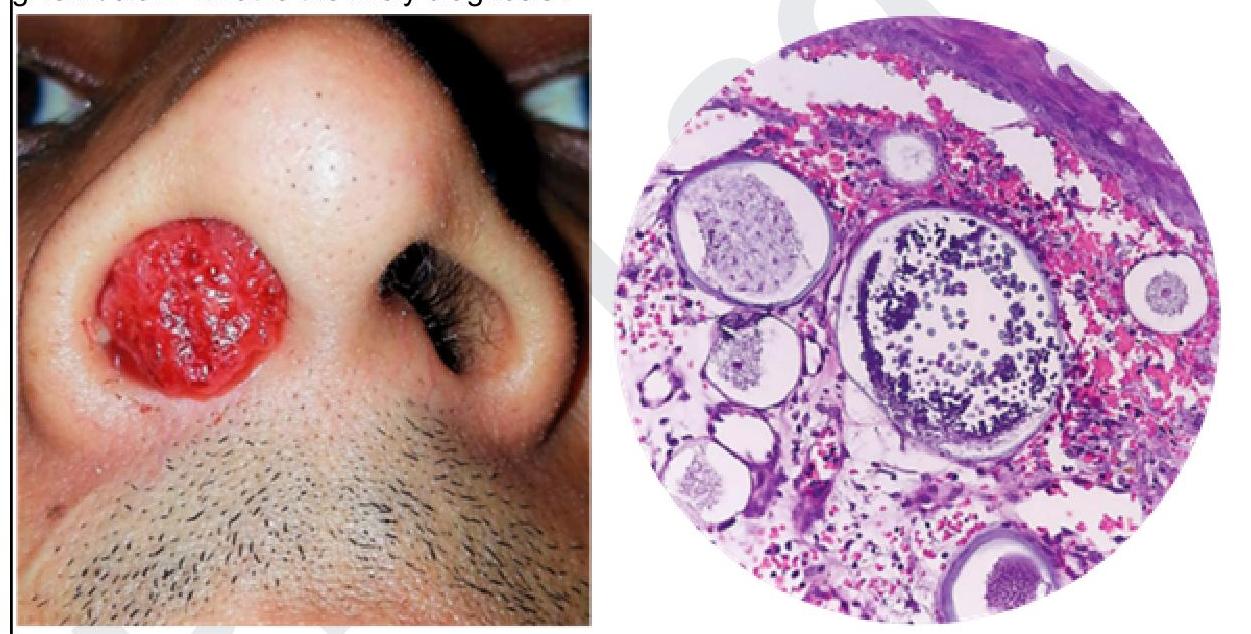
A South Indian male farmer presents to the ENT OPD with complaints of reddish mass coming out from the nose as shown in the image below and the histopathology examination is also given below. What is the likely diagnosis?
Practice by Chapter
Rhinitis
Practice Questions
Acute Rhinosinusitis
Practice Questions
Chronic Rhinosinusitis
Practice Questions
Nasal Polyposis
Practice Questions
Allergic Fungal Sinusitis
Practice Questions
Deviated Nasal Septum
Practice Questions
Epistaxis
Practice Questions
Nasal Trauma
Practice Questions
Choanal Atresia
Practice Questions
CSF Rhinorrhea
Practice Questions
Tumors of the Nose and Paranasal Sinuses
Practice Questions
Complications of Sinusitis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
