Diseases of the Nose and Paranasal Sinuses — MCQs

On this page
What is the presenting symptom of nasal myiasis?
Which of the following is NOT a cause of epistaxis?
Pain sensations from the ethmoidal sinus are carried by which nerve?
A 22-year-old male with recurrent bleeding, presents with bowing of posterior maxillary wall on CECT. All are false except?
A patient presented to the OPD with complaints of greenish black matter in the nose with foul-smelling discharge. What is the diagnosis?
A 45-year-old male was admitted with respiratory distress. CT showed a nasal polyp with fluid collection in the sinus. Drainage of which of the following is obstructed?
A patient presents with a thick nasal discharge and headache. Examination reveals hypertrophy of the inferior turbinate with a mulberry appearance. Which of the following is the most likely diagnosis?
A 40-year-old patient presents with recurrent and severe nosebleeds from the anterior nasal septum. The bleeding has been refractory to nasal packing and chemical cautery. A decision is made to proceed with surgical ligation to control the bleeding. Which of the following arteries is the primary target for ligation in the management of this patient's anterior epistaxis?
A 12-year-old male with a history of recurrent epistaxis presents with nasal obstruction for the past 1 year. On examination the presence of nasal mass and investigation shows bowing of the posterior wall of maxillary sinus. What is the probable diagnosis?
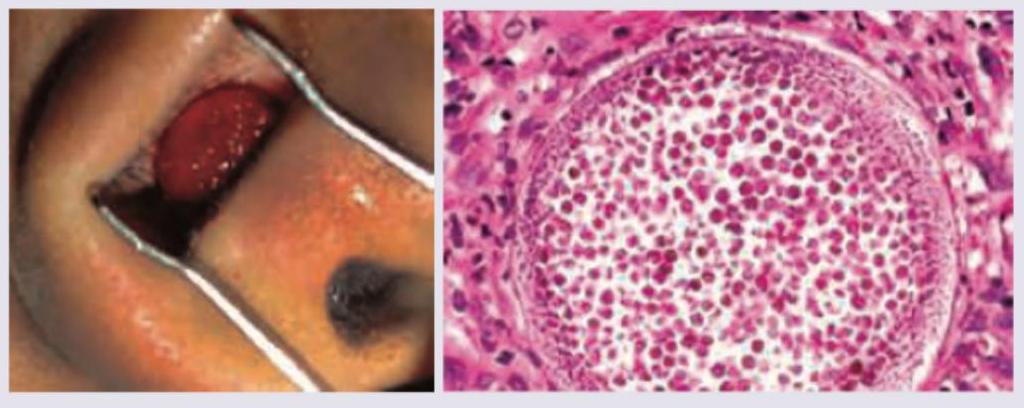
A 15-year-old female presents with nasal obstruction and occasional profuse epistaxis for last 8 weeks. Nasal speculum view and histopathology of resected lesion is given. All are correct about the diagnosis except:
Practice by Chapter
Rhinitis
Practice Questions
Acute Rhinosinusitis
Practice Questions
Chronic Rhinosinusitis
Practice Questions
Nasal Polyposis
Practice Questions
Allergic Fungal Sinusitis
Practice Questions
Deviated Nasal Septum
Practice Questions
Epistaxis
Practice Questions
Nasal Trauma
Practice Questions
Choanal Atresia
Practice Questions
CSF Rhinorrhea
Practice Questions
Tumors of the Nose and Paranasal Sinuses
Practice Questions
Complications of Sinusitis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
