Diseases of the Nose and Paranasal Sinuses — MCQs

On this page
A diabetic patient presents with a nasal mass and blackish discharge. What is the most likely diagnosis?
Proof puncture is done through which anatomical location?
In CSF rhinorrhea, from which anatomical structure does CSF originating from the middle cranial fossa typically reach the nasal cavity?
What is a common cause of discharge from the nose?
Strawberry appearance of the nasal mucosa is a characteristic finding in which of the following conditions?
Following Caldwell-Luc operation, a patient develops hypoesthesia. Which nerve is likely damaged?
Which of the following statements about nasal glioma is FALSE?
A 32-year-old female patient underwent extraction of an upper first molar on the right side, resulting in a 0.3 mm perforation into the sinus wall. From which anatomical location does the Caldwell-Luc incision begin?
A female who underwent laparoscopic appendectomy for acute appendicitis developed difficulty in breathing and a swelling in the anterior part of the nasal septum after bumping her nose on a table on post-operative day 2. What is the next line of management?
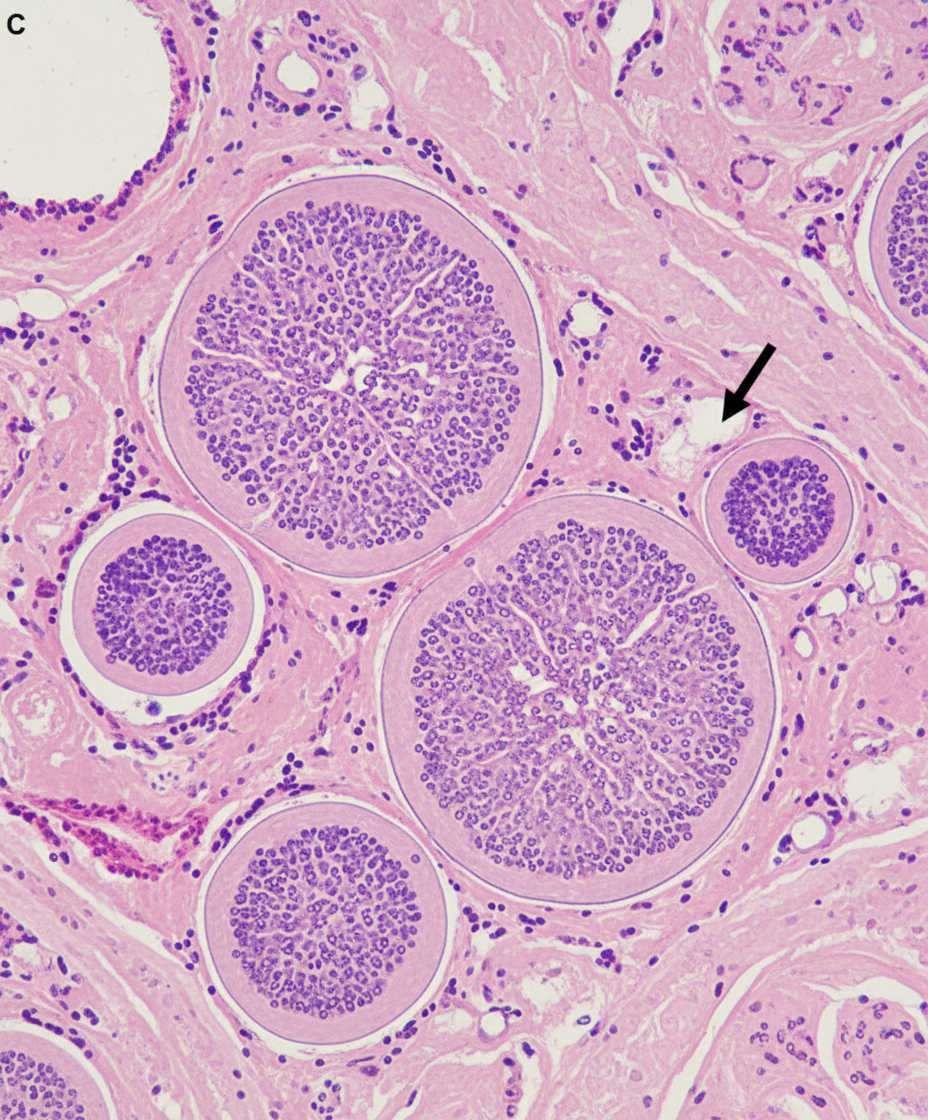
A 60-year-old male complains of right-sided nasal obstruction and nasal discharge, which is sometimes blood-tinged. Biopsy findings are shown below. What is your diagnosis?
Practice by Chapter
Rhinitis
Practice Questions
Acute Rhinosinusitis
Practice Questions
Chronic Rhinosinusitis
Practice Questions
Nasal Polyposis
Practice Questions
Allergic Fungal Sinusitis
Practice Questions
Deviated Nasal Septum
Practice Questions
Epistaxis
Practice Questions
Nasal Trauma
Practice Questions
Choanal Atresia
Practice Questions
CSF Rhinorrhea
Practice Questions
Tumors of the Nose and Paranasal Sinuses
Practice Questions
Complications of Sinusitis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
