Diseases of the Nose and Paranasal Sinuses — MCQs

On this page
A 70-year-old patient presents with epistaxis and hypertension (BP 200/100 mm Hg). On examination, no active bleeding is noted. What is the next step in management?
Sphenoid sinusitis pain is referred most commonly to:
The opening of the posterior ethmoid sinus is located in which anatomical structure?
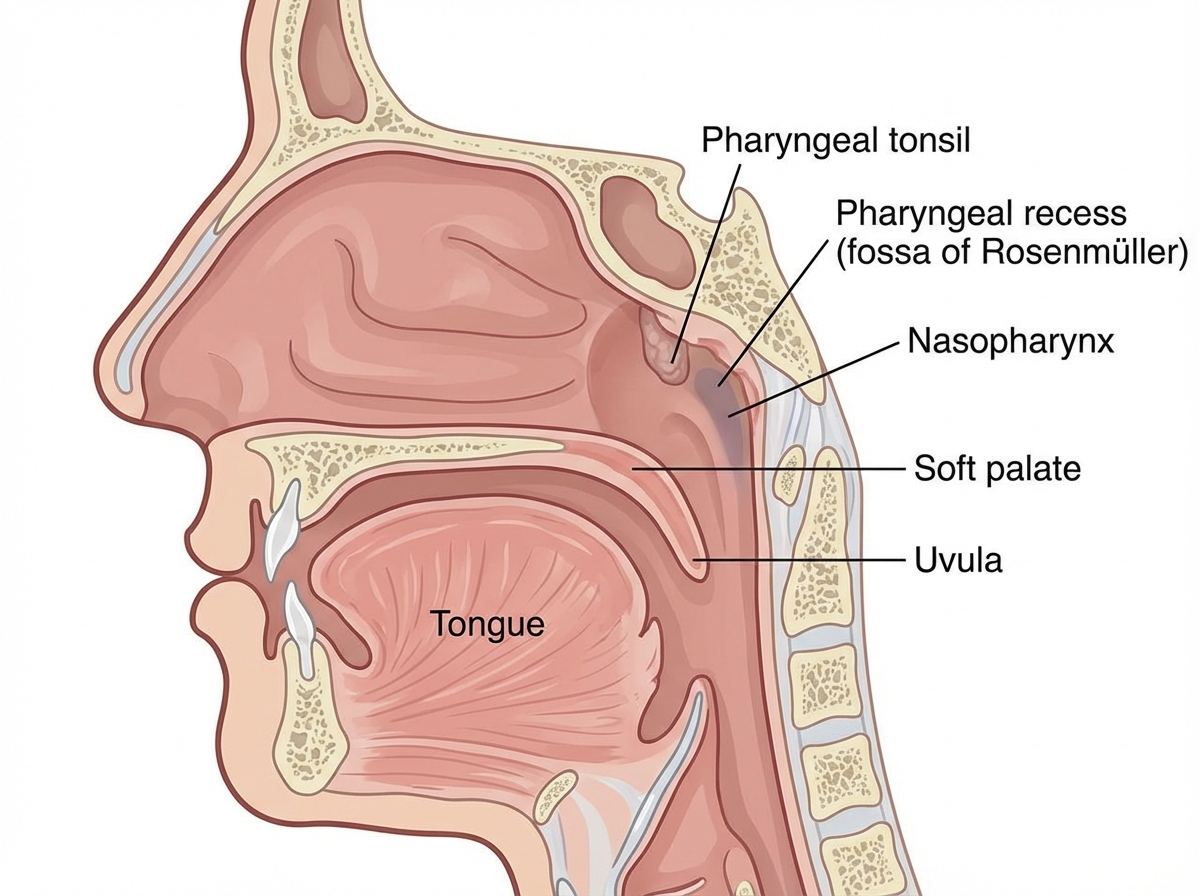
A marked area in the nasopharynx gives rise to which of the following diseases?
What is the treatment of choice in recurrent epistaxis in a patient with hereditary hemorrhagic telangiectasia?
A patient with a sinus infection develops bilateral proptosis, chemosis, and fever. What is the most likely diagnosis?
Which test is used to measure nasal mucociliary clearance?
Dennie-Morgan lines are seen in which of the following conditions?
What is the name of the incision used for the maxillary sinus?
A unilateral mass causing nasal obstruction is seen in the nose of a patient. What is the most probable diagnosis?
Practice by Chapter
Rhinitis
Practice Questions
Acute Rhinosinusitis
Practice Questions
Chronic Rhinosinusitis
Practice Questions
Nasal Polyposis
Practice Questions
Allergic Fungal Sinusitis
Practice Questions
Deviated Nasal Septum
Practice Questions
Epistaxis
Practice Questions
Nasal Trauma
Practice Questions
Choanal Atresia
Practice Questions
CSF Rhinorrhea
Practice Questions
Tumors of the Nose and Paranasal Sinuses
Practice Questions
Complications of Sinusitis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
