Phototherapy and Photobiology — MCQs

On this page
What is the mechanism of action of psoralen?
A 45-year-old farmer presents with itchy erythematous papular lesions on the face, neck, 'V' area of the chest, and dorsum of hands and forearms, present for 3 years. The lesions are more severe in summers and improve in winters. What is the most appropriate diagnostic test for this condition?
What is the typical wavelength range of a Wood's lamp?
All are true regarding Polymorphous light eruption (PMLE), EXCEPT?
On a 4 Gy dose of radiation to the scalp, when does alopecia typically develop?
Which of the following skin conditions is treated with PUVA therapy?
Solar urticaria is characterized by which of the following skin reactions after exposure to the sun?
A 32-year-old male presents with abdominal pain and vomiting. He also complains of psychiatric symptoms and visual hallucinations. What is the most likely diagnosis?
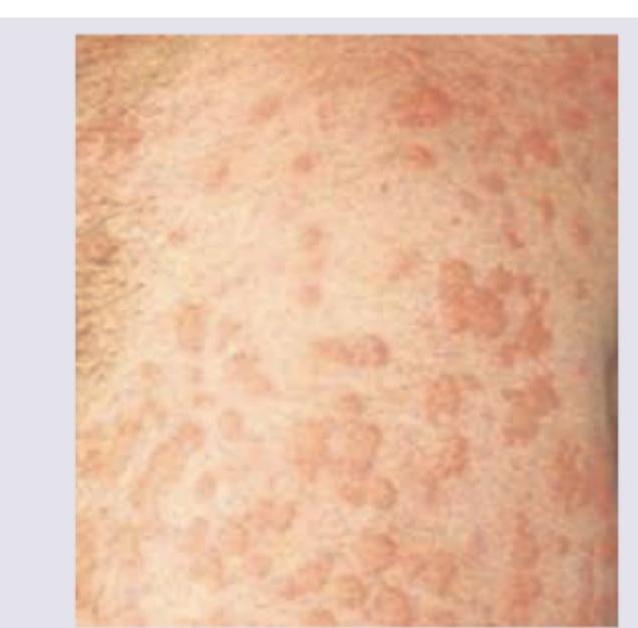
A 26-year-old female with a history of extensive exposure to sun comes to your clinic with presentation shown below. What is the most likely diagnosis?
What is the best time to give oral psoralen with UVA -
Practice by Chapter
Fundamentals of Photobiology
Practice Questions
UVA and UVB Phototherapy
Practice Questions
PUVA Therapy
Practice Questions
Narrow-Band UVB Therapy
Practice Questions
Excimer Laser Therapy
Practice Questions
Photodynamic Therapy
Practice Questions
Phototoxicity and Photoallergy
Practice Questions
Photoprotection
Practice Questions
Sunscreens
Practice Questions
Photoaging
Practice Questions
Phototherapy Protocols
Practice Questions
Management of Phototherapy Side Effects
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
