Bacterial Skin Infections — MCQs

On this page
What is the minimum number of bacilli per gram of tissue required for a positive slit skin smear for Hansen's disease?
Lupus vulgaris is a form of which of the following?
Manifestations of erythema nodosum leprosum (ENL) include all of the following except:
What is a Globi?
Bacillary angiomatosis is caused by which organism?
What is the first consideration in the differential diagnosis of a painless palatal perforation?
A farmer presents with a lesion on the leg. Which of the following is the most likely diagnosis?
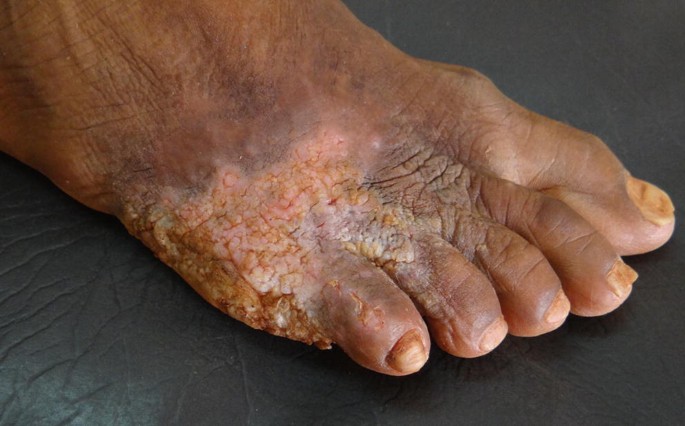
The Ridley-Jopling classification of leprosy is a type of?
Apple jelly nodules on diascopy are characteristic of which condition?
A penile ulcer is painful in which of the following conditions?
Practice by Chapter
Impetigo
Practice Questions
Folliculitis, Furuncles, and Carbuncles
Practice Questions
Ecthyma
Practice Questions
Erysipelas and Cellulitis
Practice Questions
Staphylococcal Scalded Skin Syndrome
Practice Questions
Necrotizing Fasciitis
Practice Questions
Cutaneous Tuberculosis
Practice Questions
Leprosy
Practice Questions
Lyme Disease
Practice Questions
Syphilis
Practice Questions
Antibiotic Resistance in Dermatology
Practice Questions
Prophylaxis and Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
