Epidemiology — MCQs

On this page
Which of the following scales is used for quantitative data?
Which of the following is a live oral vaccine?
The Sullivan index indicates:
Which one of the following will be affected by inter-observer variation in epidemiological studies?
According to Revised National Tuberculosis Control Programme (RNTCP) guidelines, what is the case definition for sputum examination?
The "floating tip of the iceberg" phenomenon in epidemiology represents which of the following?
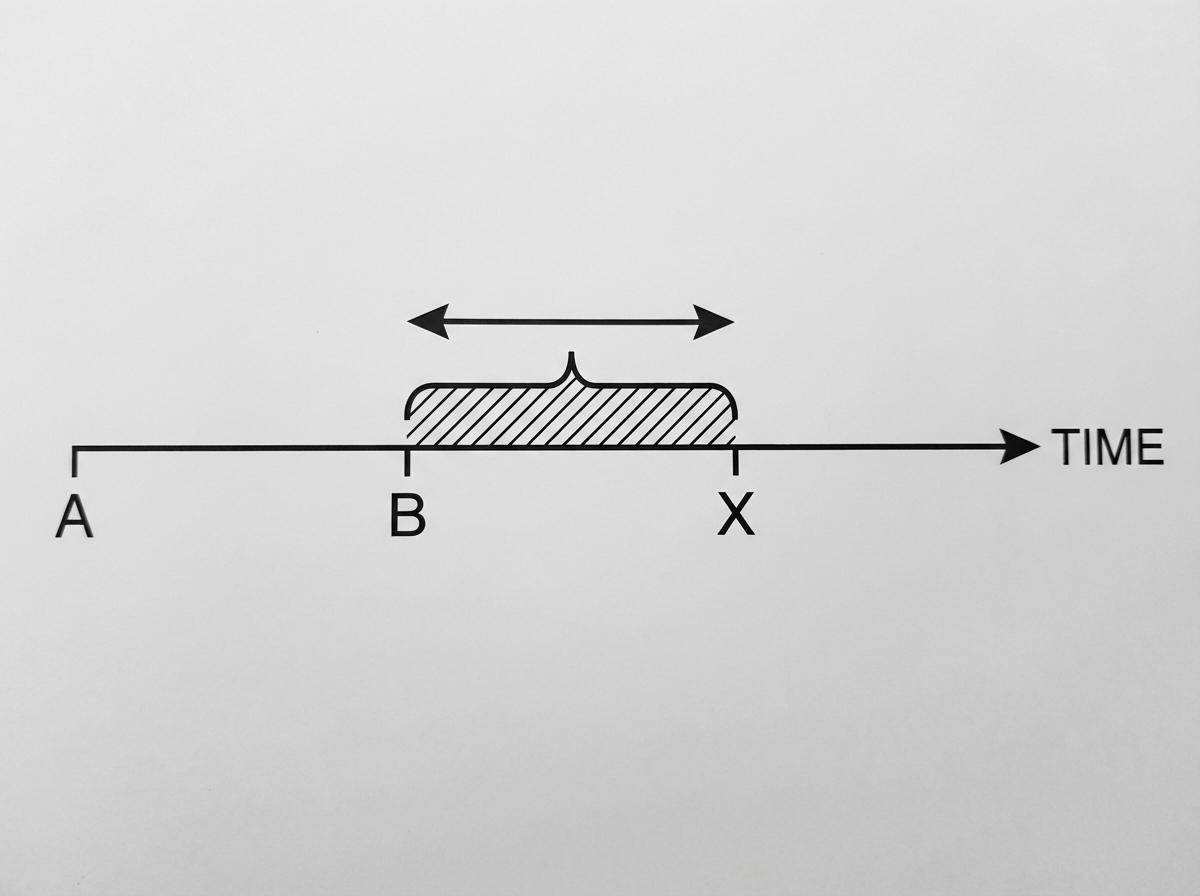
In the natural history of a disease, what does B-X duration represent?
The epidemiological triad includes all of the following EXCEPT:
For the purpose of intervention trials, the preferred randomization unit is an individual for all of the following except?
Under the National Malaria Eradication Programme (NMEP), what is the minimum annual blood examination rate that should be achieved?
Practice by Chapter
Principles of Epidemiology
Practice Questions
Measures of Disease Frequency
Practice Questions
Epidemiological Study Designs
Practice Questions
Descriptive Epidemiology
Practice Questions
Analytical Epidemiology
Practice Questions
Experimental Epidemiology
Practice Questions
Screening for Disease
Practice Questions
Surveillance Systems
Practice Questions
Investigation of an Epidemic
Practice Questions
Association and Causation
Practice Questions
Modern Epidemiological Methods
Practice Questions
Critical Appraisal of Epidemiological Studies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
