Epidemiology — MCQs

On this page
Which of the following diseases shows seasonal trends?
Secondary level of prevention includes all of the following except?
Which of the following is NOT a primary level of prevention?
The incubation period of Rabies depends on which of the following factors?
Annual blood smear examination rate is an indicator of which of the following?
Screening for a condition is recommended when?
Number of new cases occurring in a defined population during a specified period of time is known as:
Which of the following statements is NOT true regarding infective endocarditis?
Taking a history of smoking in a pregnant woman and following its effect on the fetus is an example of which type of epidemiological study?
Which epidemiological study design is represented by the following illustration?
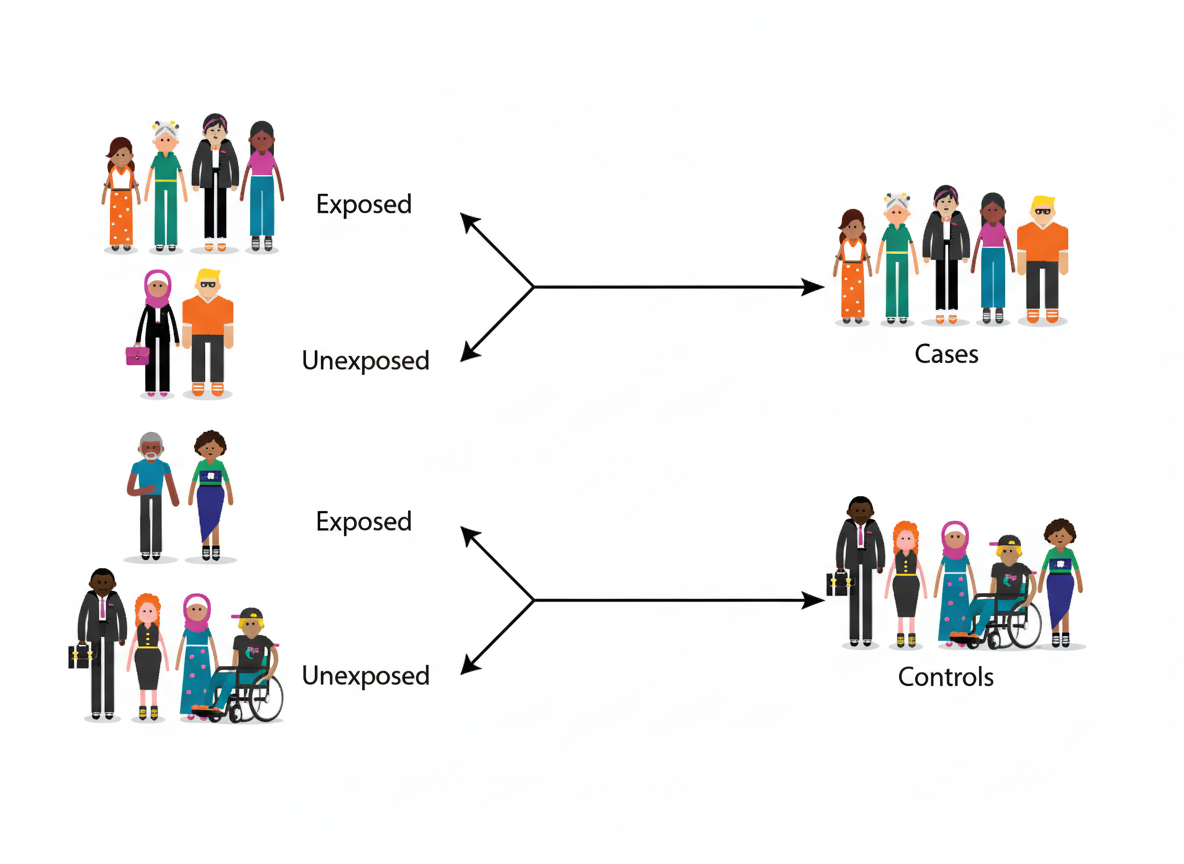
Practice by Chapter
Principles of Epidemiology
Practice Questions
Measures of Disease Frequency
Practice Questions
Epidemiological Study Designs
Practice Questions
Descriptive Epidemiology
Practice Questions
Analytical Epidemiology
Practice Questions
Experimental Epidemiology
Practice Questions
Screening for Disease
Practice Questions
Surveillance Systems
Practice Questions
Investigation of an Epidemic
Practice Questions
Association and Causation
Practice Questions
Modern Epidemiological Methods
Practice Questions
Critical Appraisal of Epidemiological Studies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
