Carbohydrate Metabolism — MCQs

On this page
Name the antigen marked as X determining blood group A.
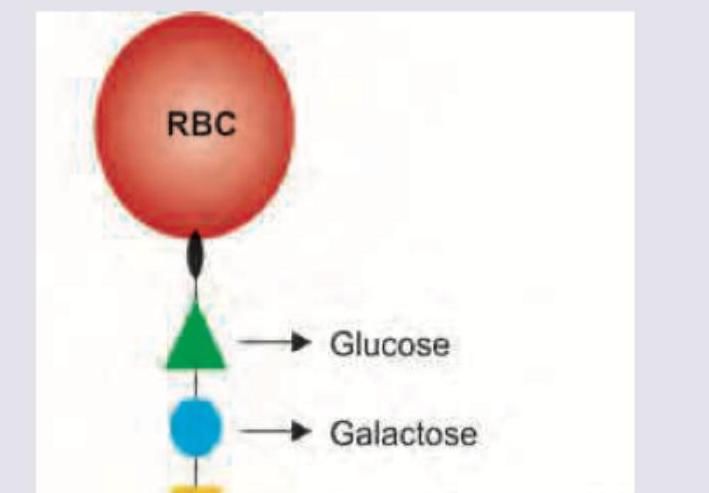
The enzyme catalyzing this pathway is absent in?
A 50-year-old male with family history for type 2 diabetes underwent a urine test for reducing substances. The test tube containing 0.5 ml of urine and 5 ml Benedict's reagent was put in a water bath for 2 minutes and change in colour of tube was noticed. Which is the correct statement about the concentration of sugar in the test tube?

Which transporter helps in the improvement of insulin resistance in type 2 diabetes mellitus (DM2) with regular exercise and physical activities?
Corneal Transparency is maintained by which of the following GAGs?
Which of the following is not a substrate for glucose formation?
What is the primary mechanism for glucose uptake in neurons?
A 20-year-old male with no significant medical history comes to you with a urine positive for fructose. He does not have diabetes mellitus. Which enzyme is most likely to be deficient in this patient?
Which of the following is present in skeletal muscle?
Synovial fluid contains-
Practice by Chapter
Carbohydrate Chemistry and Classification
Practice Questions
Glycolysis: Reactions and Regulation
Practice Questions
Gluconeogenesis: Reactions and Regulation
Practice Questions
Glycogen Metabolism: Synthesis and Breakdown
Practice Questions
Glycogen Storage Diseases
Practice Questions
Pentose Phosphate Pathway
Practice Questions
Metabolism of Fructose and Galactose
Practice Questions
Disorders of Fructose and Galactose Metabolism
Practice Questions
Blood Glucose Regulation
Practice Questions
Diabetes Mellitus: Biochemical Aspects
Practice Questions
Glycosylation and Glycoproteins
Practice Questions
Lactose Intolerance and Galactosemia
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
