Carbohydrate Metabolism — MCQs

On this page
A pregnant woman with lactase deficiency cannot tolerate milk in her diet and is concerned about producing milk of insufficient caloric value to nourish her baby. What is the best advice to give her?
Disaccharides are digested mostly in which part of the digestive tract?
The polyol pathway is responsible for the formation of which of the following?
Dextrose is:
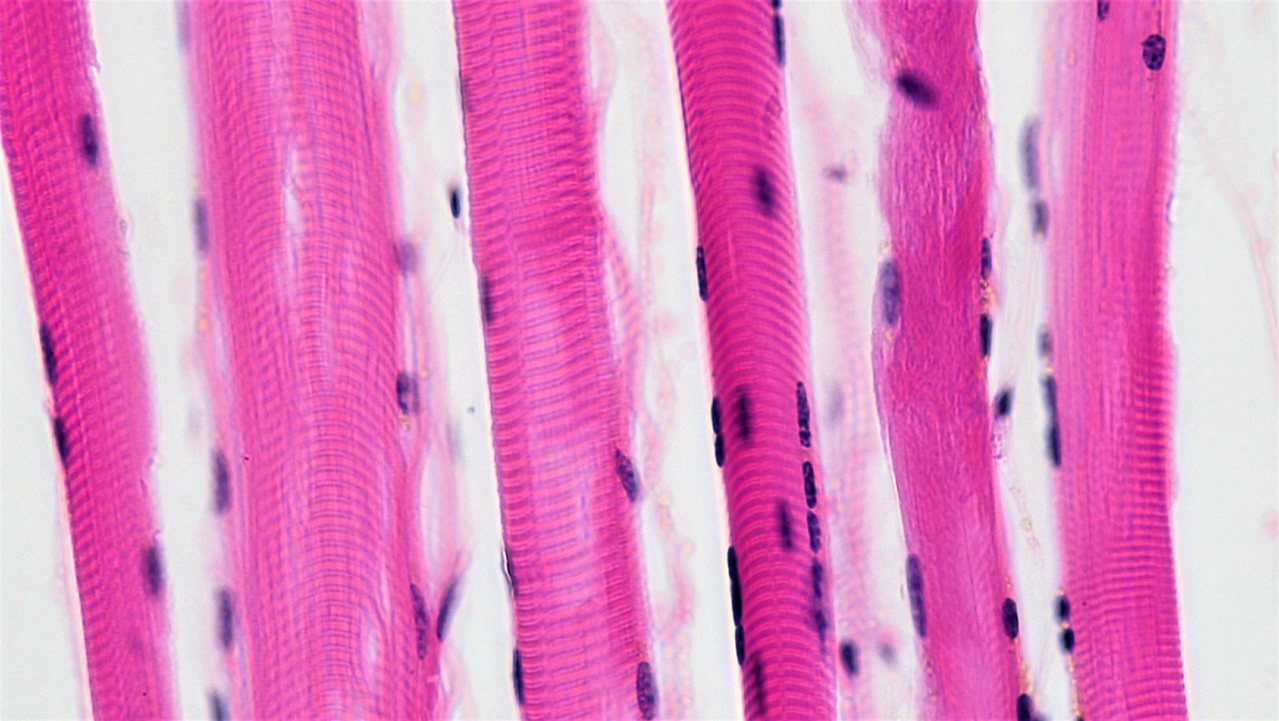
The muscle shown in the illustration predominantly uses which glucose transporter?
Which molecule, known to initiate cataract formation in the eye lens, also has a 1-phosphate derivative responsible for liver failure?
Which of the following is also known as milk sugar?
In which of the following steps is ATP released?
Oxidation of galactose with a strong oxidizing agent produces which of the following?
Insulin is required for glucose transport in all of the following tissues except:
Practice by Chapter
Carbohydrate Chemistry and Classification
Practice Questions
Glycolysis: Reactions and Regulation
Practice Questions
Gluconeogenesis: Reactions and Regulation
Practice Questions
Glycogen Metabolism: Synthesis and Breakdown
Practice Questions
Glycogen Storage Diseases
Practice Questions
Pentose Phosphate Pathway
Practice Questions
Metabolism of Fructose and Galactose
Practice Questions
Disorders of Fructose and Galactose Metabolism
Practice Questions
Blood Glucose Regulation
Practice Questions
Diabetes Mellitus: Biochemical Aspects
Practice Questions
Glycosylation and Glycoproteins
Practice Questions
Lactose Intolerance and Galactosemia
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
