Regional Anesthesia — MCQs

On this page
All are correct about the regional anesthesia provided to the patient except:
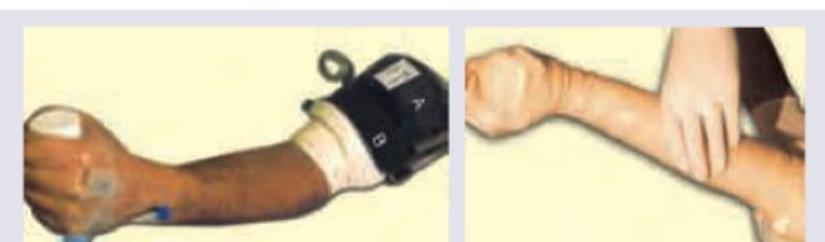
Which finding indicates correct placement of needle in this nerve block? (Recent NEET Pattern 2016-17)
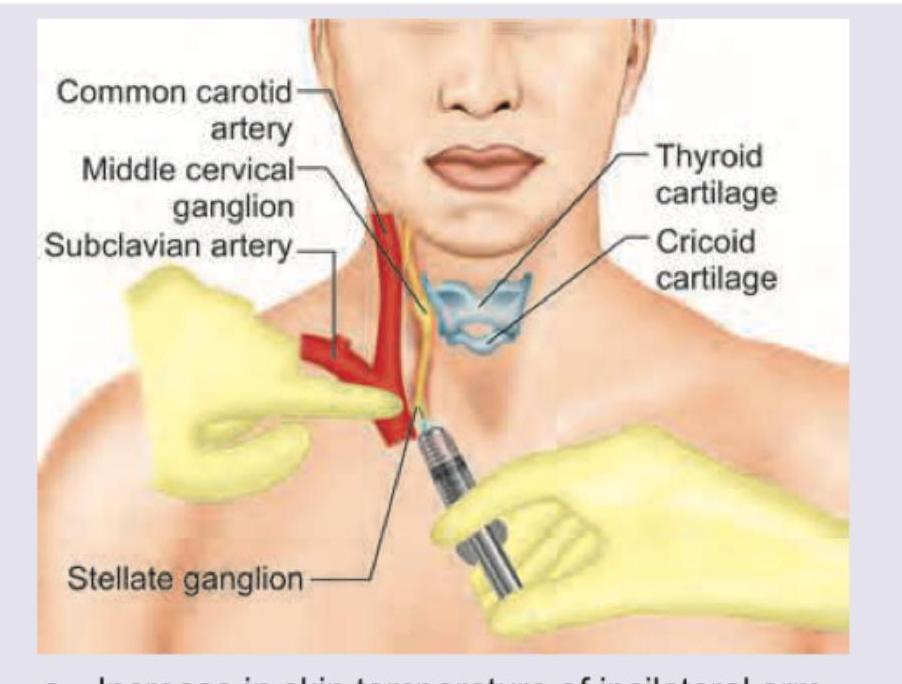
All are contraindications of this anesthesia technique except: (Recent NEET Pattern 2016-17)
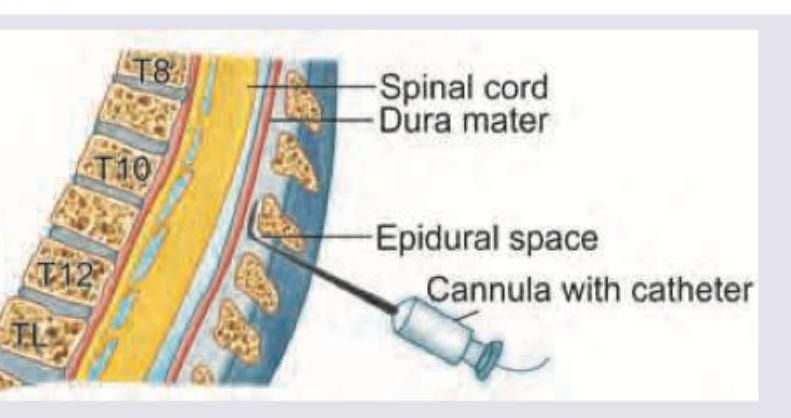
All are complications of this anesthesia technique except: (Recent NEET Pattern 2016-17)
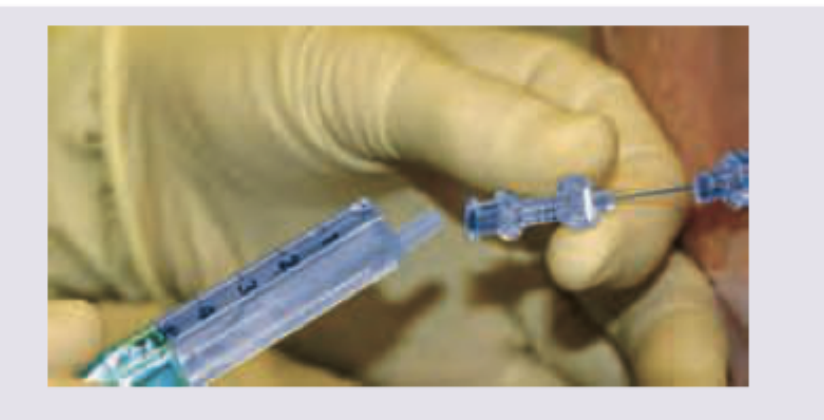
Name the spinal needle shown in the image:
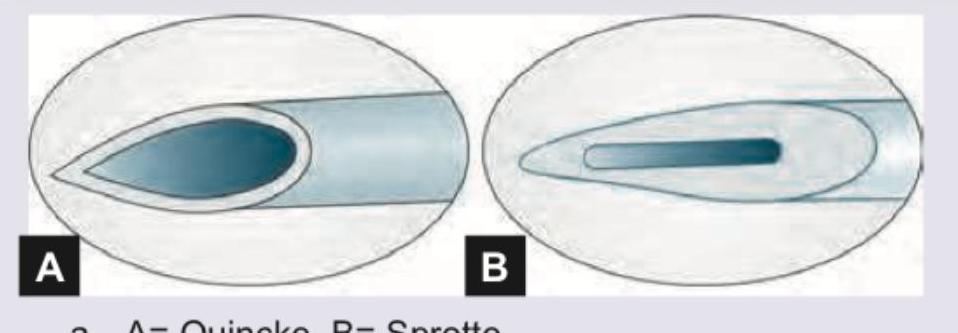
Which is not true regarding the procedure done with the needle shown below?

A patient is placed in the **lateral decubitus position** (lying on their side with knees drawn toward the chest and the spine flexed/arched outward) before the procedure. This position is maintained during which of the following types of anaesthesia?
Contraindications to epidural analgesia include the following except
What is the name of the nerve block technique shown in the image?
The duration of spinal anaesthesia is based directly on:
Practice by Chapter
Neuraxial Anatomy
Practice Questions
Spinal Anesthesia
Practice Questions
Epidural Anesthesia
Practice Questions
Combined Spinal-Epidural Anesthesia
Practice Questions
Peripheral Nerve Blocks: Upper Extremity
Practice Questions
Peripheral Nerve Blocks: Lower Extremity
Practice Questions
Truncal Blocks
Practice Questions
Ultrasound-Guided Regional Anesthesia
Practice Questions
Complications of Regional Anesthesia
Practice Questions
Regional Anesthesia in Pediatric Patients
Practice Questions
Regional Anesthesia in Obstetrics
Practice Questions
Continuous Peripheral Nerve Catheters
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
