Regional Anesthesia — MCQs

On this page
Which of the following local anesthetics causes the least vasodilation?
What is the standard dose of lignocaine for spinal anesthesia?
Which of the following approaches for a brachial plexus block is most suitable for catheter placement?
A 32-year-old male presents with an 8 cm laceration on the medial plantar aspect of his left foot after stepping on broken glass. Which peripheral nerve block is appropriate for this injury?
Which of the following statements regarding spinal cord and neuraxial blockade is true?
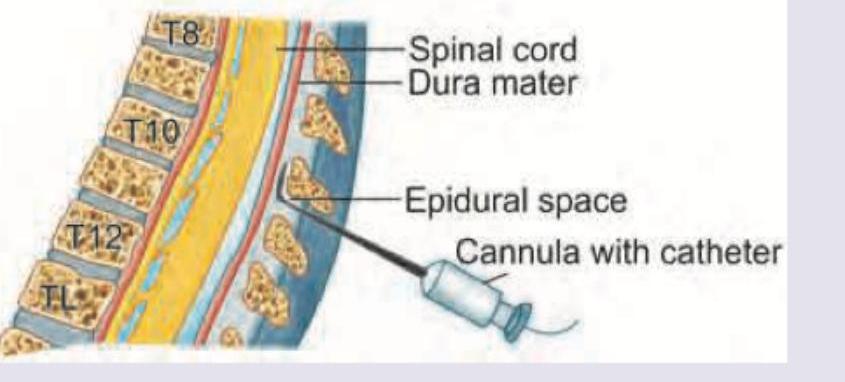
During epidural analgesia, which of the following signs suggests that the needle is in the extradural space?
Which of the following types of nerves are affected after a spinal anesthetic block?
In epidural anesthesia, which of the following layers is least likely to be punctured during the procedure?
Which of the following is most suitable for intravenous regional anesthesia?
During administration of following anesthesia with 10 mL of 2% xylocaine, the patient develops hypotension with respiratory depression. Which of the following is the probable cause? (AIIMS Nov 2016)
Practice by Chapter
Neuraxial Anatomy
Practice Questions
Spinal Anesthesia
Practice Questions
Epidural Anesthesia
Practice Questions
Combined Spinal-Epidural Anesthesia
Practice Questions
Peripheral Nerve Blocks: Upper Extremity
Practice Questions
Peripheral Nerve Blocks: Lower Extremity
Practice Questions
Truncal Blocks
Practice Questions
Ultrasound-Guided Regional Anesthesia
Practice Questions
Complications of Regional Anesthesia
Practice Questions
Regional Anesthesia in Pediatric Patients
Practice Questions
Regional Anesthesia in Obstetrics
Practice Questions
Continuous Peripheral Nerve Catheters
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
