Regional Anesthesia — MCQs

On this page
What is the vasopressor of choice in hypotension produced during subarachnoid block?
For which of the following is continuous epidural anaesthesia used?
Regarding lidocaine, which of the following statements is false?
EMLA cream is effective in relieving pain of which procedures?
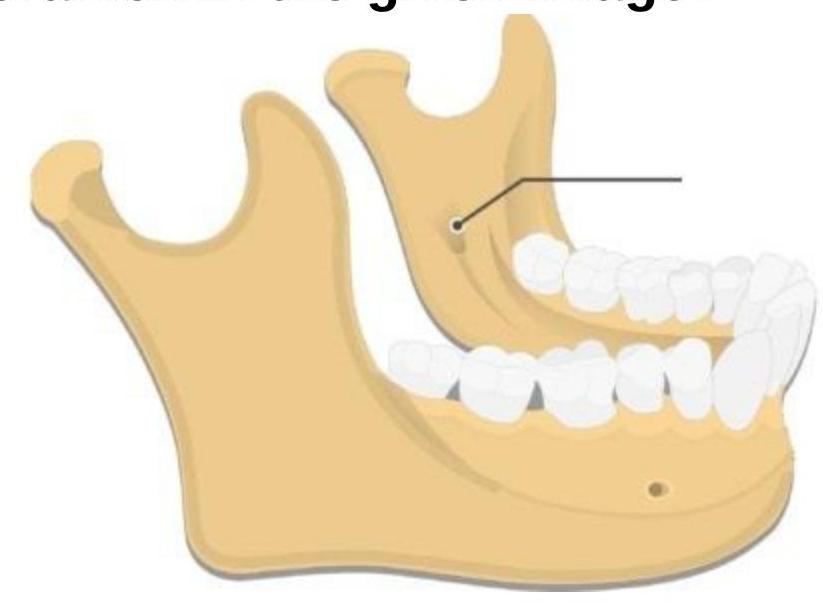
What is true regarding a bilateral mandibular block?
Local anesthetic toxicity is maximally seen with which of the following routes of administration?
What is the order of absorption routes for local anesthetics, from fastest to slowest?
Which of the following is NOT true about post-spinal headache?
The topical use of which of the following local anesthetics is not recommended?
The block shown in the diagram is going to affect all of the following nerves EXCEPT?
Practice by Chapter
Neuraxial Anatomy
Practice Questions
Spinal Anesthesia
Practice Questions
Epidural Anesthesia
Practice Questions
Combined Spinal-Epidural Anesthesia
Practice Questions
Peripheral Nerve Blocks: Upper Extremity
Practice Questions
Peripheral Nerve Blocks: Lower Extremity
Practice Questions
Truncal Blocks
Practice Questions
Ultrasound-Guided Regional Anesthesia
Practice Questions
Complications of Regional Anesthesia
Practice Questions
Regional Anesthesia in Pediatric Patients
Practice Questions
Regional Anesthesia in Obstetrics
Practice Questions
Continuous Peripheral Nerve Catheters
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
