Neuroanesthesia — MCQs

On this page
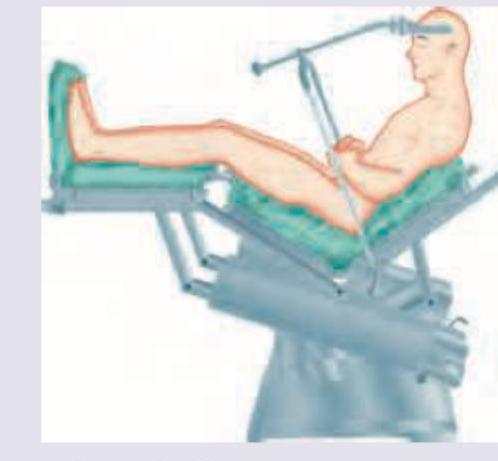
A patient is scheduled for neurosurgery for posterior fossa tumor. During the surgery the BP crashes and Et CO2 suddenly decreases to zero. What is the most likely diagnosis?
A comatose patient after sustaining severe head injury has been admitted to the neurosurgical ICU. Which of the following parameters should ideally be maintained in this patient? 1. pCO2 = 4.5 - 5.0 kPa (33-38 mm Hg) 2. MAP = 80 - 90 mm of Hg 3. pO2 > 11 kPa (> 80 mm Hg) 4. Na+ < 130 meq/L
Anesthetic agent contraindicated in raised ICT is?
Which of the following is the best cerebroprotective drug?
Thiopentone has cerebroprotective effect because of –
All of the following decrease cerebral blood flow and intracranial pressure except:
Increased intracranial pressure occurs with:
Which of the following anaesthetic agents causes a rise in the Intracranial pressure:
Which of the following anesthetic agents may have cerebroprotective effect:
Which of the following drugs is contraindicated in a patient with raised intracranial pressure ?
Practice by Chapter
Cerebral Physiology and Pathophysiology
Practice Questions
Anesthetics and Cerebral Blood Flow
Practice Questions
Intracranial Pressure Management
Practice Questions
Anesthesia for Supratentorial Craniotomy
Practice Questions
Anesthesia for Infratentorial Craniotomy
Practice Questions
Anesthesia for Traumatic Brain Injury
Practice Questions
Neuromonitoring Techniques
Practice Questions
Anesthesia for Spine Surgery
Practice Questions
Anesthesia for Neurovascular Procedures
Practice Questions
Awake Craniotomy
Practice Questions
Neuromuscular Disorders
Practice Questions
Postoperative Care in Neurosurgical Patients
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
