Thorax — MCQs

On this page
What does the spinal epidural space contain?
The spinal epidural space is largest at which vertebral level?
Which part of the subclavian artery is affected by stenosis?
At which vertebral level does the thoracic duct enter the thorax from the abdomen?
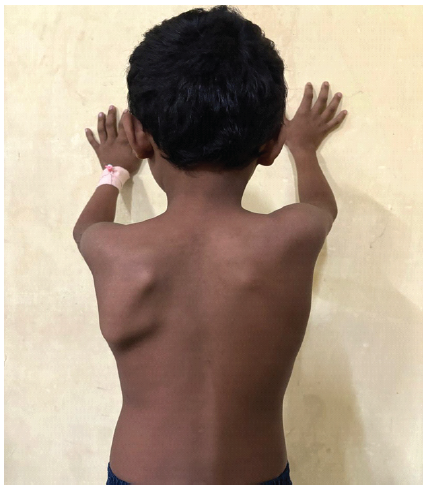
Which nerve is involved in this presentation?
What is the approximate distance of diaphragmatic constriction from the nostril and incisor, respectively?
A 40-year-old male smoker was diagnosed with carcinoma of the right lung. A bronchogram showed a tumor causing partial occlusion of the eparterial bronchus. Which of the following bronchopulmonary segments receive decreased airflow?
Which of the following is not a boundary of the triangle of safety?
The thoracic duct does NOT drain which part of the body?
Which of the following statements is NOT true about the superior vena cava?
Practice by Chapter
Thoracic Wall and Diaphragm
Practice Questions
Pleura and Lungs
Practice Questions
Mediastinum
Practice Questions
Heart and Pericardium
Practice Questions
Great Vessels and Azygos System
Practice Questions
Thoracic Duct and Lymphatics
Practice Questions
Autonomic Innervation
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Thoracic Imaging and Cross-sectional Anatomy
Practice Questions
Embryological Development of Thoracic Structures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
