Thorax — MCQs

On this page
Which of the following statements is true about the right atrium?
A patient underwent sentinel node biopsy for treatment of breast carcinoma. Which of the following nerves is likely to be injured during this procedure?
What artery supplies the SA node?
The thoracic duct terminates by emptying into which structure?
The nipple is supplied by which of the following intercostal nerves?
In which intercostal space is the typical arrangement of vein, artery, and nerve (VAN) absent?
Anastomosis around the shoulder is between branches of which parts of the subclavian and axillary arteries?
Which of the following structures form the bulge marked X?
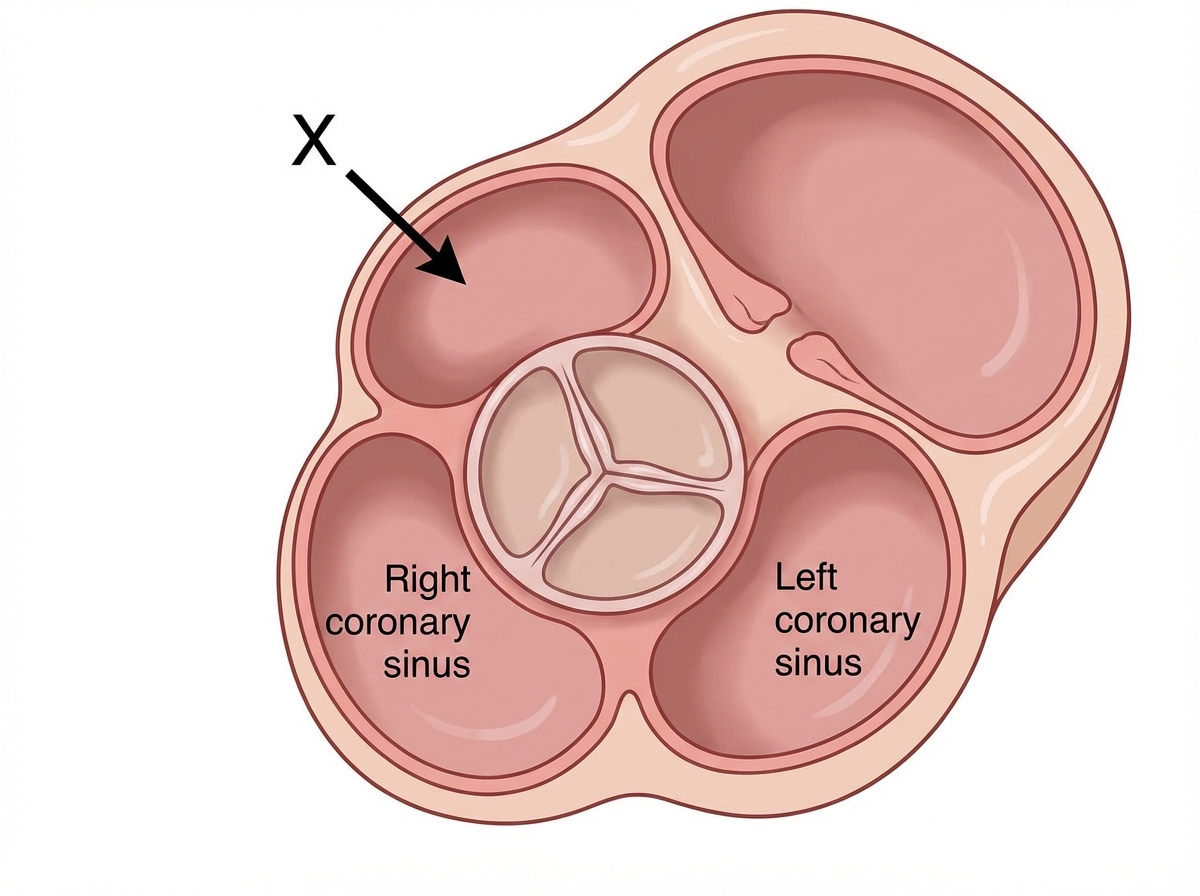
Which of the following statements is NOT true?
Which chamber forms the base of the heart?
Practice by Chapter
Thoracic Wall and Diaphragm
Practice Questions
Pleura and Lungs
Practice Questions
Mediastinum
Practice Questions
Heart and Pericardium
Practice Questions
Great Vessels and Azygos System
Practice Questions
Thoracic Duct and Lymphatics
Practice Questions
Autonomic Innervation
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Thoracic Imaging and Cross-sectional Anatomy
Practice Questions
Embryological Development of Thoracic Structures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
