Thorax — MCQs

On this page
The right coronary artery supplies all of the following parts of the conducting system in the heart except:
What is the normal fluid level in the pericardial cavity?
What is referred to as a "Potential Anastomosis"?
Which artery supplies the upper one-third of the esophagus?
A 40-year-old male underwent coronary artery bypass grafting. During the procedure, the surgeon applied a clamp to the vessel lying anterior to the transverse pericardial sinus. Identify this vessel.
Which of the following statements regarding the diaphragm is true?
Which structure passes through the esophageal hiatus?
Which of the following statements regarding cardiac conduction functions are TRUE/FALSE?
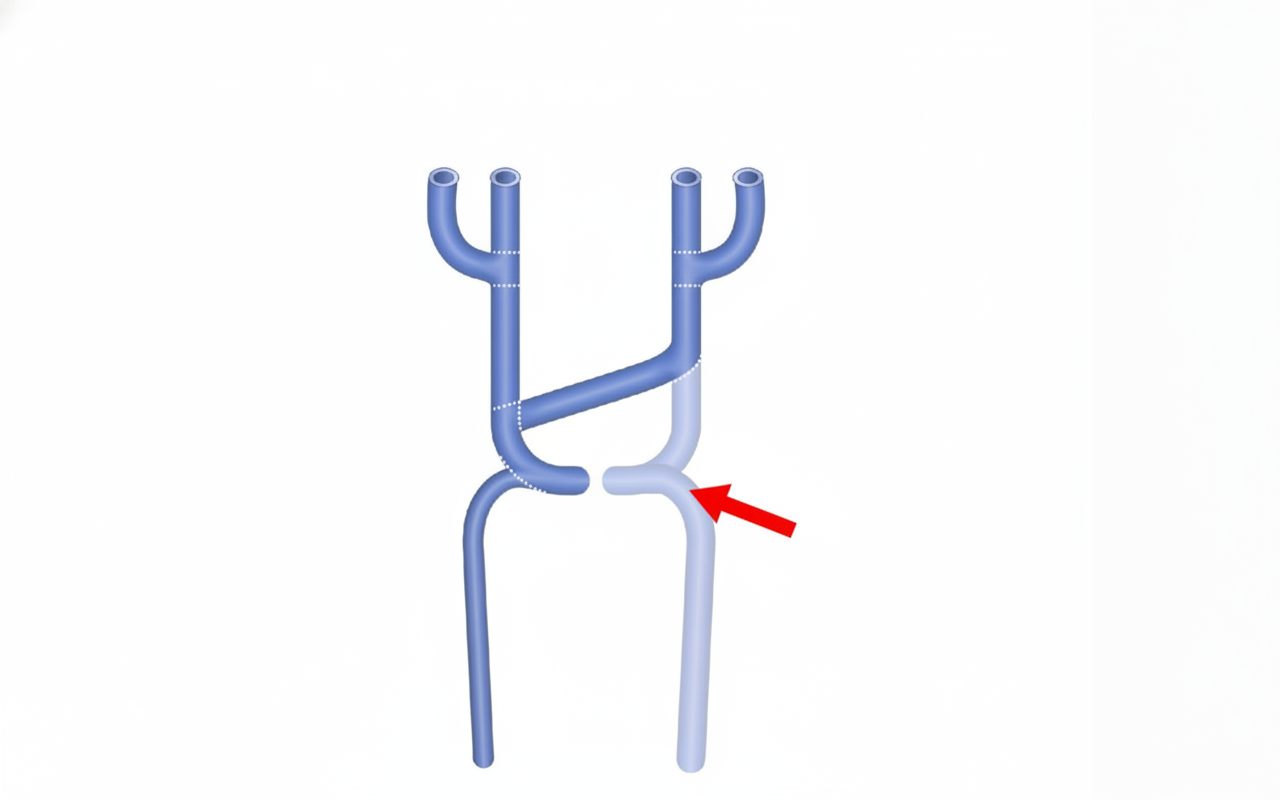
The arrow-marked structure drains into which chamber of the heart?
All are true about extralobar pulmonary sequestration except:
Practice by Chapter
Thoracic Wall and Diaphragm
Practice Questions
Pleura and Lungs
Practice Questions
Mediastinum
Practice Questions
Heart and Pericardium
Practice Questions
Great Vessels and Azygos System
Practice Questions
Thoracic Duct and Lymphatics
Practice Questions
Autonomic Innervation
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Thoracic Imaging and Cross-sectional Anatomy
Practice Questions
Embryological Development of Thoracic Structures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
