Systemic Anatomy — MCQs

On this page
Which of the following is a multipennate muscle?
In case of Inferior Vena Cava (IVC) obstruction, which of the following collateral pathways does NOT open up?
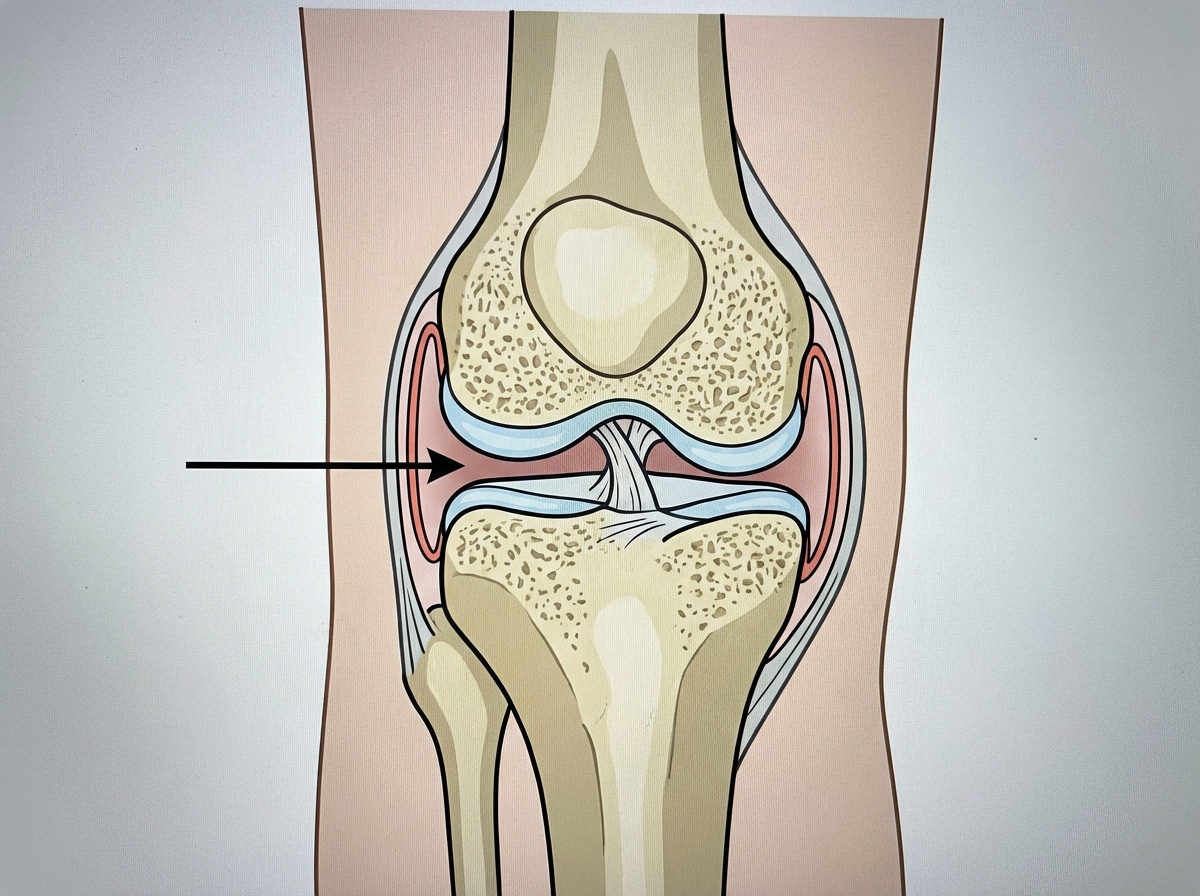
What type of joint is indicated at the site marked by the arrow?
The coracoid process of the scapula is which type of epiphysis?
Spleniculi are seen in which anatomical location?
Which type of cartilage covers a synovial joint?
The fracture of the diaphysis involves which of the following bones?
Which of the following is NOT a pneumatic bone?
The gonadal arteries are derived from which of the following?
All of the following organs are categorized as secondary lymphoid organs, EXCEPT?
Practice by Chapter
Skeletal System
Practice Questions
Articular System
Practice Questions
Muscular System
Practice Questions
Cardiovascular System
Practice Questions
Lymphatic System
Practice Questions
Nervous System
Practice Questions
Respiratory System
Practice Questions
Digestive System
Practice Questions
Urinary System
Practice Questions
Reproductive System
Practice Questions
Endocrine System
Practice Questions
Integumentary System
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
