Microscopic Anatomy — MCQs

On this page
Cells which surround the oocyte in graafian follicle are called ?
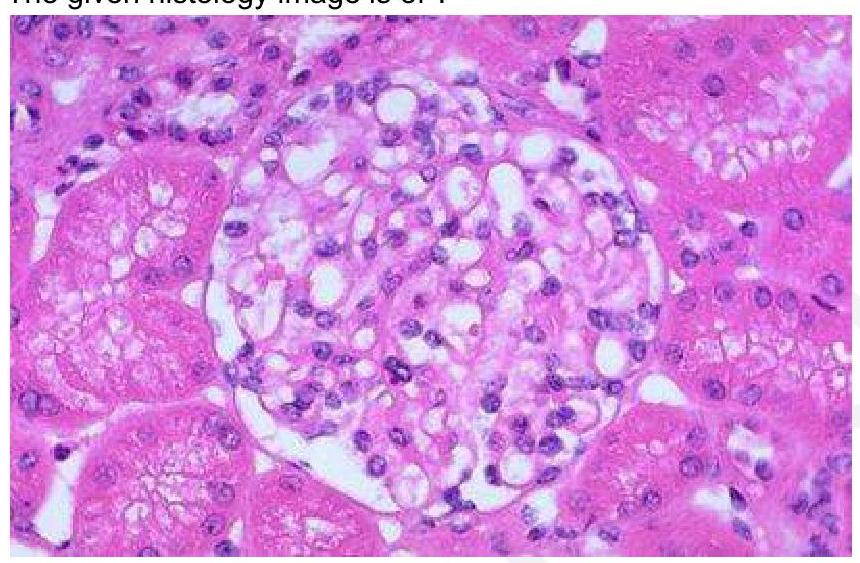
The given histology image is of which structure?
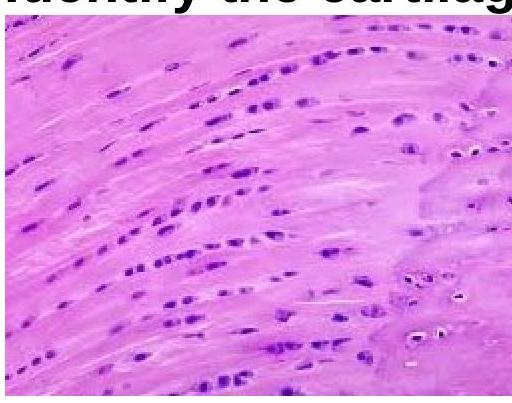
Identify the type of cartilage shown in the image.
Which type of collagen is the most abundant in the human skin?
Which of the following accurately describes the anatomical structure of the hard palate?
What is the type of epithelium of the adenoid?
Ceruminous glands present in the ear are:
Which area in the spleen is considered *primarily* thymus-dependent?
In the context of blood pressure regulation, where are baroreceptors primarily located?
Blood testis barrier in testis is formed by?
Practice by Chapter
Cellular Ultrastructure
Practice Questions
Microscopic Anatomy of Epithelial Tissues
Practice Questions
Microscopic Anatomy of Connective Tissues
Practice Questions
Microscopic Anatomy of Muscle Tissues
Practice Questions
Microscopic Anatomy of Nervous Tissues
Practice Questions
Microscopic Anatomy of Blood and Immune System
Practice Questions
Microscopic Anatomy of Endocrine Glands
Practice Questions
Microscopic Anatomy of Digestive System
Practice Questions
Microscopic Anatomy of Respiratory System
Practice Questions
Microscopic Anatomy of Urinary System
Practice Questions
Microscopic Anatomy of Reproductive System
Practice Questions
Techniques in Microscopic Anatomy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
