Microscopic Anatomy — MCQs

On this page
Basement membrane around Schwann cells contains which of the following collagens?
What is the type of cell lining the small intestine?
Which of the following is present in Paneth cells?
What is the cell junction marked by the circle?
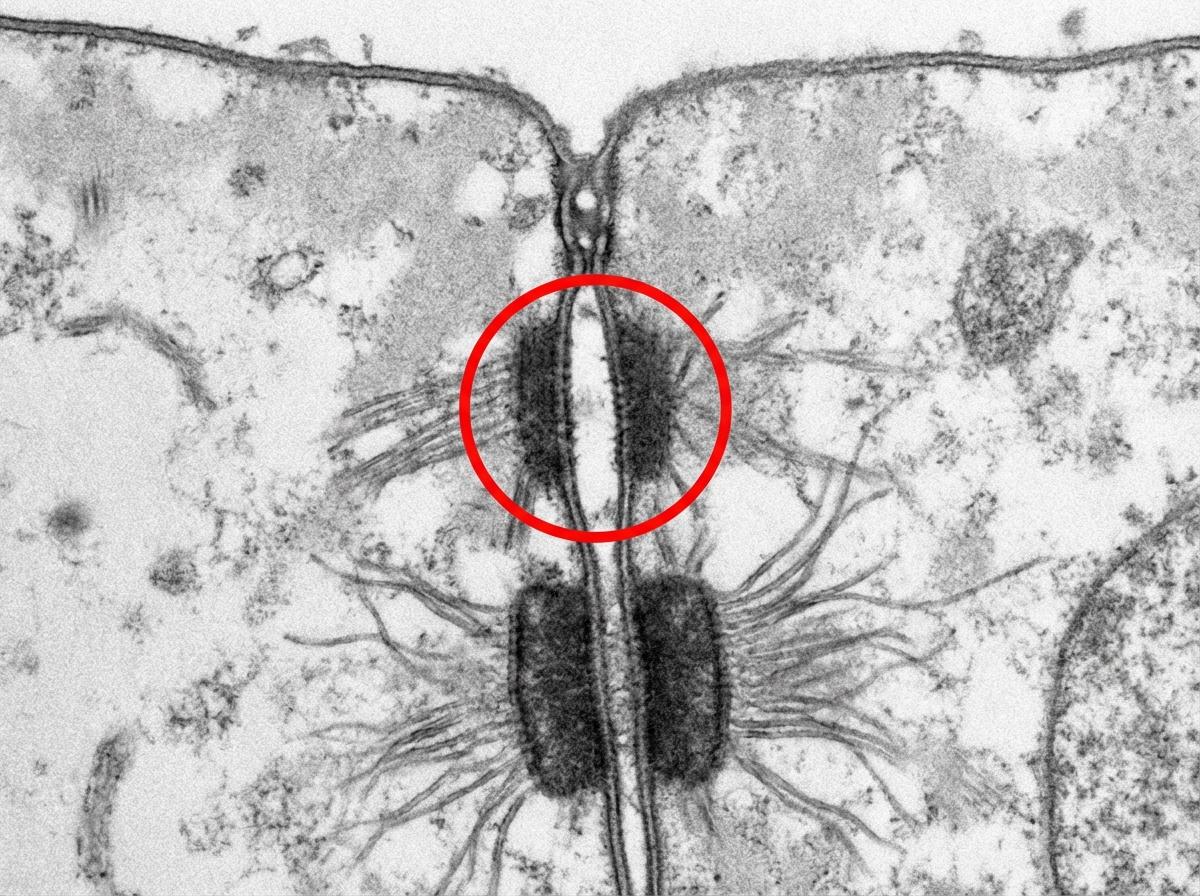
Which one of the following is NOT a component of the filtration slit diaphragm at the glomerulus?
Practice by Chapter
Cellular Ultrastructure
Practice Questions
Microscopic Anatomy of Epithelial Tissues
Practice Questions
Microscopic Anatomy of Connective Tissues
Practice Questions
Microscopic Anatomy of Muscle Tissues
Practice Questions
Microscopic Anatomy of Nervous Tissues
Practice Questions
Microscopic Anatomy of Blood and Immune System
Practice Questions
Microscopic Anatomy of Endocrine Glands
Practice Questions
Microscopic Anatomy of Digestive System
Practice Questions
Microscopic Anatomy of Respiratory System
Practice Questions
Microscopic Anatomy of Urinary System
Practice Questions
Microscopic Anatomy of Reproductive System
Practice Questions
Techniques in Microscopic Anatomy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
