Clinical Anatomy — MCQs

On this page
Frey's syndrome is associated with-
The landmark shown here is
During resuscitation, fractured ribs most commonly involve:
Frey's syndrome is due to the involvement of
A resident at the emergency department is preparing for a lumbar puncture in a 26 years old female with suspected subarachnoid bleeding. Although she presented with altered sensorium, CT brain was found to be normal. During LP, which structure is pierced after the spinal needle crosses interspinous ligament?
Frey's syndrome occurs due to aberrant misdirection of fibers from salivary glands to sweat glands. These fibers come from which of the following?
Pronator teres syndrome is related to which nerve?
Clinical testing of the function of the long thoracic nerve is done by:
Loss of flexion in the interphalangeal joint of thumb in supracondylar fracture is due to involvement of which nerve?
In carpal tunnel syndrome, which nerve is compressed?
Clinical Anatomy Indian Medical PG Practice Questions and MCQs
Question 81: Frey's syndrome is associated with-
- A. Motor fibres of facial nerve
- B. Parasympathetic fibres of auriculo temporal nerve (Correct Answer)
- C. Sympathetic fibres of auriculo temporal nerve
- D. Parasympathetic fibres of trigeminal nerve
Explanation: ***Parasympathetic fibres of auriculo temporal nerve*** - **Frey's syndrome**, or **gustatory sweating**, occurs due to aberrant regeneration of damaged **auriculotemporal nerve fibers** after **parotid gland surgery** or trauma. - **Parasympathetic secretomotor fibers** that originally innervated the **parotid gland** mistakenly reinnervate overlying **sweat glands** and **blood vessels** of the skin. *Motor fibres of facial nerve* - **Motor fibers of the facial nerve** control **facial expression muscles** and are not directly involved in the pathogenesis of Frey's syndrome. - Damage to these fibers would result in **facial paralysis**, not gustatory sweating. *Sympathetic fibres of auriculo temporal nerve* - The **auriculotemporal nerve** contains **sensory fibers** to the temporal region and **parasympathetic secretomotor fibers** to the parotid gland, but its sympathetic fibers are primarily **vasomotor**. - **Sympathetic fibers** control vasoconstriction and eccrine sweating generally, but their aberrant regeneration is not the cause of Frey's syndrome. *Parasympathetic fibres of trigeminal nerve* - The **trigeminal nerve** is primarily **sensory** to the face and **motor** to the muscles of mastication; it does not directly innervate the parotid gland. - **Parasympathetic innervation** to the parotid gland is carried by the glossopharyngeal nerve via the otic ganglion, not the trigeminal nerve.
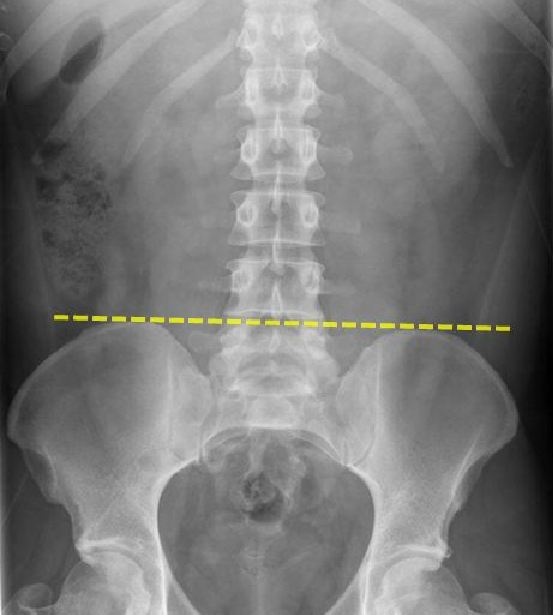
Question 82: The landmark shown here is
- A. Nelaton's line
- B. Transpyloric plane
- C. Shenton's line
- D. Tuffier’s line (Correct Answer)
Explanation: ***Tuffier's line*** - **Tuffier's line**, also known as the intercristal line, connects the highest points of the **iliac crests**. - This line typically corresponds to the level of the **L4 vertebral body** or the L4-L5 intervertebral space, which is an important landmark for lumbar punctures. *Nelaton's line* - **Nelaton's line** is drawn from the **anterior superior iliac spine** to the **ischial tuberosity** of the same side. - It is used to assess for superior displacement of the greater trochanter in conditions like **hip dislocation** or **femoral neck fracture**. *Transpyloric plane* - The **transpyloric plane** is a horizontal plane located halfway between the **suprasternal notch** and the **pubic symphysis**. - It typically passes through the **pylorus of the stomach**, the neck of the pancreas, and the hila of the kidneys, corresponding to the level of the **L1 vertebral body**. *Shenton's line* - **Shenton's line** is an arc formed by the medial margin of the **femoral neck** and the inferior margin of the superior pubic ramus and obturator foramen. - It is used to assess for integrity of the **femoral neck-shaft angle** and is commonly broken in cases of hip dislocation or femoral neck fractures.
Question 83: During resuscitation, fractured ribs most commonly involve:
- A. 3rd -5th ribs
- B. 2nd -4th ribs
- C. 5th -7th ribs
- D. 4th -6th ribs (Correct Answer)
Explanation: ***4th -6th ribs*** - During **cardiopulmonary resuscitation (CPR)**, compressions are typically applied to the **sternum**, leading to direct pressure on the adjacent ribs. - The **middle ribs**, particularly the 4th, 5th, and 6th, are most susceptible to fracture due to their anatomical position and lever arm during compressions. *3rd -5th ribs* - While these ribs can be fractured during CPR, the **3rd rib** is less commonly affected than the 4th-6th due to its more superior position and attachment. - The range does not fully encompass the ribs most consistently subjected to maximum stress during typical chest compressions. *2nd -4th ribs* - Fractures of the **2nd rib** are relatively uncommon during CPR, as it is more protected by the clavicle and shoulder girdle. - This range largely excludes the **5th and 6th ribs**, which are frequently implicated in CPR-related fractures. *5th -7th ribs* - The **7th rib** is less commonly fractured than the 4th-6th ribs because compressions are generally focused higher on the sternum. - This range includes the 7th rib, which is often below the primary point of maximum force during CPR.
Question 84: Frey's syndrome is due to the involvement of
- A. Glossopharyngeal nerve
- B. Auriculotemporal nerve (Correct Answer)
- C. Vagus nerve
- D. All of the options
Explanation: ***Auriculotemporal nerve*** - Frey's syndrome, also known as **auriculotemporal syndrome**, occurs due to damage and aberrant regeneration of the **auriculotemporal nerve** after parotid gland surgery or other trauma. - This leads to sweating and flushing in the preauricular and temporal regions while eating, as parasympathetic fibers that normally innervate the parotid gland mistakenly reinnervate sweat glands and blood vessels in the skin. *Glossopharyngeal nerve* - The **glossopharyngeal nerve** (CN IX) primarily supplies the parotid gland with secretomotor innervation but is typically not directly involved in the pathogenesis of Frey's syndrome itself. - Damage to this nerve would primarily affect taste sensation on the posterior one-third of the tongue, swallowing, and salivation, but not typically the characteristic sweating patterns of Frey's syndrome. *Vagus nerve* - The **vagus nerve** (CN X) is mainly involved in innervating organs of the thorax and abdomen, as well as providing motor and sensory innervation to the pharynx and larynx. - It has no direct anatomical or functional role in the development or symptoms of Frey's syndrome. *All of the options* - Only the **auriculotemporal nerve** is directly responsible for the symptoms of Frey's syndrome. - The glossopharyngeal and vagus nerves are not implicated in this specific condition.
Question 85: A resident at the emergency department is preparing for a lumbar puncture in a 26 years old female with suspected subarachnoid bleeding. Although she presented with altered sensorium, CT brain was found to be normal. During LP, which structure is pierced after the spinal needle crosses interspinous ligament?
- A. Supra/inter spinous ligament
- B. Skin
- C. Sub cutaneous fascia
- D. Dura mater
- E. Arachnoid mater
- F. Ligamentum flava (Correct Answer)
Explanation: The enriched explanation is the original text provided because none of the references were sufficiently relevant to the anatomy of a lumbar puncture. Ligamentum flava - After passing the interspinous ligament, the next significant structure pierced by the spinal needle during a lumbar puncture is the ligamentum flava. - This ligament is crucial for stabilizing the vertebral column and is located anterior to the interspinous ligament, connecting the laminae of adjacent vertebrae. *Supra/inter spinous ligament* - The question explicitly states that the needle has already crossed the interspinous ligament, making this an incorrect choice for the next structure. - The supraspinous ligament lies superficial to the interspinous ligament, both of which are encountered before the ligamentum flava. *Skin* - The skin is the very first layer pierced when performing a lumbar puncture. - The question is asking what is pierced after the interspinous ligament, not what is pierced first. *Sub cutaneous fascia* - The subcutaneous fascia is located directly beneath the skin and is encountered very early in the lumbar puncture procedure. - It lies superficial to all ligaments of the vertebral column, including the interspinous ligament. *Dura mater* - The dura mater is pierced after the ligamentum flava. - It is the outermost meningeal layer, which, once penetrated, indicates entry into the epidural space, followed by the subarachnoid space. *Arachnoid mater* - The arachnoid mater is a thin, delicate membrane that lies immediately deep to the dura mater. - It is pierced almost simultaneously with the dura mater, and its penetration allows entry into the subarachnoid space where CSF is collected. *Return of CSF* - The return of CSF is the result of successfully traversing all necessary layers and entering the subarachnoid space. - It is not an anatomical structure that is pierced itself, but rather the clinical endpoint of the procedure.
Question 86: Frey's syndrome occurs due to aberrant misdirection of fibers from salivary glands to sweat glands. These fibers come from which of the following?
- A. Facial
- B. Glossopharyngeal (Correct Answer)
- C. Trigeminal
- D. Vagus
Explanation: ***Glossopharyngeal*** - Frey's syndrome (auriculotemporal syndrome) is caused by injury to the **auriculotemporal nerve**, a branch of the **mandibular division of the trigeminal nerve**, which carries postganglionic parasympathetic fibers from the **otic ganglion** that originated in the glossopharyngeal nerve. - These parasympathetic fibers, normally destined for the **parotid gland** to stimulate salivation, aberrantly regenerate and innervate sweat glands and blood vessels in the skin over the parotid region, leading to sweating and flushing upon mastication. *Facial* - The facial nerve primarily controls **muscles of facial expression**, taste sensation from the anterior two-thirds of the tongue, and parasympathetic innervation of the **submandibular** and **sublingual glands**, and lacrimal gland. - While it has some parasympathetic function, its fibers are not involved in innervating the parotid gland or the aberrant sweating seen in Frey's syndrome. *Trigeminal* - The trigeminal nerve is responsible for general sensation in the face and mastication, but its fibers are **not the source of the parasympathetic neurons** causing Frey's syndrome. - The auriculotemporal nerve, a branch of the trigeminal's mandibular division, *carries* these aberrant fibers, but they originate from the glossopharyngeal nerve. *Vagus* - The vagus nerve supplies efferent parasympathetic innervation to many organs in the thorax and abdomen, and sensory innervation for the pharynx, larynx, and taste from the epiglottis. - It plays no role in the innervation of the salivary glands relevant to Frey's syndrome or in the aberrant sweating mechanism.
Question 87: Pronator teres syndrome is related to which nerve?
- A. Axillary Nerve
- B. Ulnar Nerve
- C. Radial Nerve
- D. Median Nerve (Correct Answer)
Explanation: ***Median Nerve*** - **Pronator teres syndrome** is a **compression neuropathy** of the **median nerve** as it passes between the two heads of the pronator teres muscle [1]. - Symptoms include pain in the proximal forearm, paresthesia in the median nerve distribution, and weakness in forearm pronation and thumb/finger flexion [1]. *Axillary Nerve* - The **axillary nerve** innervates the **deltoid** and **teres minor** muscles and supplies sensation to the lateral shoulder. - Its compression or injury would lead to shoulder weakness and sensory deficits, not forearm symptoms. *Ulnar Nerve* - The **ulnar nerve** passes through **Guyon's canal** at the wrist and the cubital tunnel at the elbow [1]. - Compression leads to symptoms in the **medial 1.5 digits** and weakness of intrinsic hand muscles, not related to the pronator teres. *Radial Nerve* - The **radial nerve** innervates the **extensor muscles** of the arm and forearm. - Compression or injury would result in wrist drop or sensory deficits on the dorsal hand, symptoms not associated with pronator teres syndrome.
Question 88: Clinical testing of the function of the long thoracic nerve is done by:
- A. Perform resisted flexion of the arm at the shoulder joint
- B. Perform resisted external rotation of the arm at the shoulder joint
- C. Raise the arm above the head on the affected side
- D. Push the wall with outstretched arms and observe for scapular winging (Correct Answer)
Explanation: ***Push the wall with outstretched arms and observe for scapular winging*** - The **long thoracic nerve** innervates the **serratus anterior muscle**, which is responsible for holding the scapula against the thoracic wall and for upward rotation of the scapula during arm elevation. - When the long thoracic nerve is damaged, the serratus anterior weakens, leading to classic **scapular winging** where the medial border and inferior angle of the scapula protrude posteriorly, especially when the patient pushes against a wall with outstretched arms. *Perform resisted flexion of the arm at the shoulder joint* - This action primarily tests the **deltoid muscle** and **biceps brachii**, innervated by the **axillary** and **musculocutaneous nerves**, respectively. - It does not specifically isolate the function of the serratus anterior or the long thoracic nerve. *Perform resisted external rotation of the arm at the shoulder joint* - **External rotation** of the arm at the shoulder is mainly performed by the **infraspinatus** and **teres minor muscles**, which are innervated by the **suprascapular nerve** and **axillary nerve**, respectively. - This maneuver does not evaluate the integrity of the long thoracic nerve or serratus anterior. *Raise the arm above the head on the affected side* - While the serratus anterior assists in **upward rotation of the scapula** during arm elevation, observing only global arm elevation may not be specific enough to detect subtle long thoracic nerve dysfunction. - Other muscles like the deltoid and trapezius contribute significantly to this movement, potentially masking a weak serratus anterior until more specific testing like the wall push-up test is performed.
Question 89: Loss of flexion in the interphalangeal joint of thumb in supracondylar fracture is due to involvement of which nerve?
- A. Anterior interosseous (Correct Answer)
- B. Median
- C. Ulnar
- D. Posterior interosseous
Explanation: ***Anterior interosseous*** - The **anterior interosseous nerve (AIN)** is a branch of the median nerve and innervates the **flexor pollicis longus (FPL)**, which is responsible for **flexion of the interphalangeal (IP) joint of the thumb**. [1] - A supracondylar fracture of the humerus can compress or injure the AIN, leading to weakness or paralysis of the FPL. - In clinical practice, when isolated FPL weakness occurs, we specifically identify **AIN injury** rather than general median nerve injury. *Median* - While the **anterior interosseous nerve (AIN)** is a branch of the median nerve, the question asks for the **specific nerve involved** in isolated thumb IP joint flexion loss. [1] - A proximal median nerve injury at the supracondylar level would also affect other median nerve-innervated muscles like the **flexor digitorum superficialis**, **pronator teres**, and the thenar muscles (via recurrent motor branch). [1] - The **isolated loss of IP joint flexion of the thumb** indicates a specific injury to the **AIN** rather than the entire median nerve trunk, making "Anterior interosseous" the more precise and correct answer. *Ulnar* - The **ulnar nerve** primarily innervates the **flexor carpi ulnaris** and the ulnar half of the **flexor digitorum profundus**, as well as most intrinsic hand muscles. [1] - Injury to the ulnar nerve would primarily affect **flexion of the distal interphalangeal joints of the 4th and 5th digits** and intrinsic hand muscle function, not thumb IP joint flexion. [1] *Posterior interosseous* - The **posterior interosseous nerve (PIN)** is a deep motor branch of the radial nerve and innervates the **extensor muscles** of the forearm and hand. [1] - Injury to the PIN would result in the inability to **extend the wrist and digits**, which is not consistent with the presented symptom of loss of thumb IP joint flexion.
Question 90: In carpal tunnel syndrome, which nerve is compressed?
- A. Anterior interosseous nerve
- B. Ulnar nerve
- C. Median nerve (Correct Answer)
- D. Radial nerve
Explanation: ***Median nerve*** - Carpal tunnel syndrome is caused by the **compression of the median nerve** as it passes through the **carpal tunnel** in the wrist [2]. - This compression leads to characteristic symptoms such as pain, numbness, and tingling in the thumb, index finger, middle finger, and radial half of the ring finger [2]. *Anterior interosseous nerve* - The **anterior interosseous nerve** is a branch of the median nerve that arises proximal to the carpal tunnel in the forearm [1]. - Compression of this nerve leads to **anterior interosseous syndrome**, characterized by weakness of the flexor pollicis longus and flexor digitorum profundus (to index finger), with **no sensory deficits** unlike carpal tunnel syndrome [1]. *Ulnar nerve* - The **ulnar nerve** passes through Guyon's canal at the wrist and its compression leads to conditions like ulnar neuropathy or Guyon's canal syndrome. - Ulnar nerve compression affects sensation in the little finger and ulnar half of the ring finger, and weakness of intrinsic hand muscles, distinct from carpal tunnel syndrome symptoms [2]. *Radial nerve* - The **radial nerve** controls muscles in the forearm and hand responsible for wrist and finger extension, and sensation over the back of the hand. - Compression of the radial nerve typically occurs higher up in the arm (e.g., Saturday night palsy) and results in **wrist drop** or sensory deficits on the back of the hand, not within the carpal tunnel.
Practice by Chapter
Anatomical Basis of Common Clinical Conditions
Practice Questions
Surgical Anatomy
Practice Questions
Anatomical Basis of Trauma
Practice Questions
Anatomical Aspects of Infections
Practice Questions
Anatomical Considerations in Regional Anesthesia
Practice Questions
Anatomical Basis of Physical Examination
Practice Questions
Clinical Correlations in Neuroanatomy
Practice Questions
Anatomical Approaches in Minimally Invasive Procedures
Practice Questions
Imaging Correlations in Clinical Anatomy
Practice Questions
Anatomical Variations of Clinical Importance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Start For Free