Clinical Anatomy — MCQs

On this page
Which of the following is NOT a composite muscle?
Pain of ovarian carcinoma is referred to which region?
The regionally named layer of tissue which encloses and binds muscle groups together is the:
After graft repair of a thoraco-abdominal aneurysm, a patient is unable to move both lower limbs. What is the most probable cause?
Atrophy of intrinsic muscles of the hand, sensory deficit on the medial side of the forearm and hand, and diminished radial pulse on turning the head to the affected side could be due to which of the following conditions?
Which maneuver is used to test for integrity of the long thoracic nerve?
Beevor's sign is typically associated with which group of muscles?
A 24-year-old male presents for a routine checkup. Radiographs reveal supernumerary teeth. General examination shows hypermobility of the shoulders, and the Gorlin sign is absent. What is the most probable diagnosis?
Which of the following is NOT a spiral muscle?
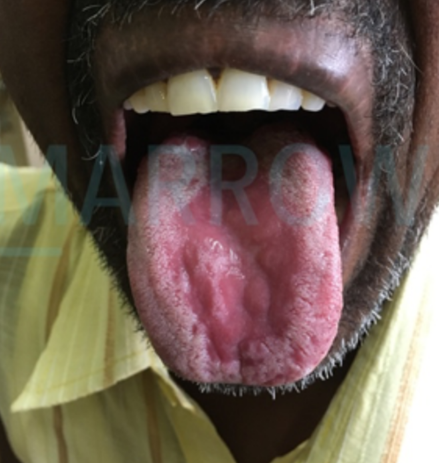
The condition shown in the color plate can be seen in which of the following syndromes?
Practice by Chapter
Anatomical Basis of Common Clinical Conditions
Practice Questions
Surgical Anatomy
Practice Questions
Anatomical Basis of Trauma
Practice Questions
Anatomical Aspects of Infections
Practice Questions
Anatomical Considerations in Regional Anesthesia
Practice Questions
Anatomical Basis of Physical Examination
Practice Questions
Clinical Correlations in Neuroanatomy
Practice Questions
Anatomical Approaches in Minimally Invasive Procedures
Practice Questions
Imaging Correlations in Clinical Anatomy
Practice Questions
Anatomical Variations of Clinical Importance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
