NEET-PG 2023 — Surgery
9 Previous Year Questions with Answers & Explanations
Patients with chronic pancreatitis often exhibit a "chain of lakes" appearance in ERCP examinations. Management is?
A 45-year-old male presenting with penile cancer extending up to the glans penis is treated with which of the following surgical options?
A patient presented with right hypochondriac pain. He had an episode of diarrhea 1 week prior. CT scan of the abdomen reveals a liver abscess of around 25 cc. What is the next step in management?
A diabetic patient presents with sudden-onset perineal pain. On examination, foul-smelling discharge and necrotic tissue are noted. Which of the following is the most characteristic feature of this condition?
A patient was brought to the ER following a road traffic accident. On examination, the patient opens his eyes to a painful stimulus, speaks inappropriately, and withdraws his limbs to a painful stimulus. What is his GCS score?
A 23-year-old male patient presents with midline swelling in the neck. The swelling moves with deglutition and protrusion of the tongue. What is the likely diagnosis?
What is the most likely diagnosis for the parotid mass with mixed consistency shown in the image?
In a patient with esophageal cancer and dysphagia affecting liquid intake, what is the most appropriate intervention to ensure nutritional support?
A patient presents with a gradually progressive, painless mass persisting for 10 years. The mass is firm to nodular and shows variable consistency within different areas of the swelling. What is the most probable diagnosis?
NEET-PG 2023 - Surgery NEET-PG Practice Questions and MCQs
Question 1: Patients with chronic pancreatitis often exhibit a "chain of lakes" appearance in ERCP examinations. Management is?
- A. Total pancreatectomy
- B. Resecting the tail of pancreas and performing a pancreaticojejunostomy
- C. Sphincteroplasty
- D. Side to side pancreaticojejunostomy (Correct Answer)
Explanation: ***Side to side pancreaticojejunostomy*** - This procedure, specifically a **Puestow procedure**, is the gold standard for managing painful chronic pancreatitis with a dilated main pancreatic duct (≥6-7 mm) and multiple strictures, presenting as a "chain of lakes" on ERCP. - It involves dividing the small bowel, closing one end, and connecting the other to a longitudinal incision made along the dilated pancreatic duct, thereby allowing drainage of pancreatic secretions into the jejunum and alleviating pain. *Total pancreatectomy* - This is a highly morbid procedure reserved for very severe cases of chronic pancreatitis that are refractory to other treatments, often associated with unmanageable pain and severe exocrine and endocrine insufficiency. - It would necessitate lifelong **enzyme replacement therapy** and **insulin for diabetes**, indicating its use as a last resort. *Sphincteroplasty* - This procedure involves widening the sphincter of Oddi and is primarily used for **biliary obstruction** or **pancreatitis secondary to sphincter dysfunction**, not for the widespread strictures and dilated ducts typical of chronic pancreatitis with a "chain of lakes" appearance. - While it can improve drainage, it does not address the extensive ductal pathology seen in many cases of chronic pancreatitis with multiple strictures. *Resecting the tail of pancreas and performing a pancreaticojejunostomy* - This describes a **distal pancreatectomy with pancreaticojejunostomy**, which is suitable for lesions or pathologies primarily confined to the **body or tail of the pancreas**, such as certain tumors or cysts. - It would not effectively address the diffuse ductal changes and multiple strictures throughout the entire pancreas that cause the "chain of lakes" appearance in chronic pancreatitis, which usually requires decompression of the entire duct system.
Question 2: A 45-year-old male presenting with penile cancer extending up to the glans penis is treated with which of the following surgical options?
- A. Partial penectomy with a 2 cm margin (Correct Answer)
- B. Simple circumcision
- C. Partial penectomy with a 4 cm margin
- D. Partial penectomy with inguinal lymph node dissection
Explanation: ***Partial penectomy with a 2 cm margin*** - For **penile cancer** confined to the glans, **partial penectomy** is the standard surgical approach to achieve local control while preserving penile length. - Historically, a **2 cm tumor-free margin** was recommended as the standard of care (reflected in older guidelines and exam questions). - **Modern evidence** suggests that narrower margins of **5-8 mm** are oncologically safe with comparable local control rates, but the **2 cm margin** was the traditional teaching and remains the expected answer for this question context. *Simple circumcision* - **Simple circumcision** is indicated for benign conditions like **phimosis** or **premalignant lesions** (carcinoma in situ), not for invasive cancer. - It does not provide adequate oncological clearance for **invasive penile cancer** and carries a high risk of **local recurrence**. *Partial penectomy with a 4 cm margin* - A **4 cm margin** is excessively radical and would result in unnecessary loss of penile length and function. - Even by historical standards, this exceeds the recommended **2 cm margin** and would cause significant functional and psychological morbidity. *Partial penectomy with inguinal lymph node dissection* - **Inguinal lymph node dissection** is indicated when there is **clinical or radiological evidence of lymph node metastasis** or high-risk pathological features. - Without evidence of nodal involvement, routine prophylactic lymphadenectomy is not performed due to significant morbidity (lymphedema, wound complications). - The question does not specify nodal involvement, making this option unnecessarily aggressive.
Question 3: A patient presented with right hypochondriac pain. He had an episode of diarrhea 1 week prior. CT scan of the abdomen reveals a liver abscess of around 25 cc. What is the next step in management?
- A. PAIR
- B. Surgery
- C. Medical therapy (Correct Answer)
- D. Percutaneous drainage
Explanation: ***Medical therapy*** - This is the appropriate next step for a **small liver abscess** of 25 cc (approximately 2.9 cm diameter). - Current evidence-based guidelines recommend **medical therapy alone** for abscesses **<5 cm in diameter**. - The preceding diarrheal episode suggests **amebic liver abscess**, which responds excellently to **metronidazole** with drainage reserved for non-responders. - Success rate with medical therapy alone for small abscesses is **>85%**. - Percutaneous drainage is reserved for: abscesses >5 cm, failed medical therapy (no improvement in 4-7 days), left lobe location, or imminent rupture. *Percutaneous drainage* - This would be indicated for **larger abscesses (>5 cm)**, left lobe abscesses, or if medical therapy fails after 4-7 days. - For a **small 25 cc abscess**, immediate drainage is unnecessary and carries procedural risks without added benefit. - Drainage should be considered if fever persists beyond 72 hours of appropriate antibiotics or clinical deterioration occurs. *PAIR* - **PAIR (Puncture, Aspiration, Injection, Re-aspiration)** is specifically for **hydatid cysts**, not pyogenic or amebic liver abscesses. - Injecting scolicidal agents would be inappropriate and potentially harmful in non-hydatid pathology. *Surgery* - Surgical drainage is reserved for **complicated cases**: ruptured abscess, multiple/loculated collections failing percutaneous drainage, or thick-walled abscesses. - A small, uncomplicated 25 cc abscess does not warrant surgical intervention as first-line management.
Question 4: A diabetic patient presents with sudden-onset perineal pain. On examination, foul-smelling discharge and necrotic tissue are noted. Which of the following is the most characteristic feature of this condition?
- A. Mixed aerobic and anaerobic infection (Correct Answer)
- B. Urinary diversion may be considered in severe cases
- C. Bilateral orchidectomy is not routinely required
- D. Anti-gas gangrene serum is indicated only in specific cases
Explanation: **Mixed aerobic and anaerobic infection** - Fournier's gangrene is a polymicrobial infection typically involving a **synergistic mixture of aerobic and anaerobic bacteria**. - This mixed infection contributes to the rapid progression and tissue destruction seen in this condition, leading to the **foul-smelling discharge** due to anaerobic metabolism. *Anti-gas gangrene serum is indicated only in specific cases.* - Anti-gas gangrene serum is specifically for **Clostridium perfringens** infections, which can cause gas gangrene but is usually a distinct clinical entity from Fournier's. - While Clostridium species can be present in Fournier's gangrene, it is not the sole causative agent, and **broader antimicrobial therapy** is the mainstay of treatment, not antitoxin serum. *Urinary diversion may be considered in severe cases.* - Urinary diversion, such as a **suprapubic catheter**, may be necessary when the urethra or perineum is extensively involved or to prevent ongoing contamination of the surgical site. - However, it's not a primary treatment for the infection itself but rather an **adjunctive measure** to manage complicated cases of Fournier's gangrene. *Bilateral orchidectomy is not routinely required.* - **Testicular involvement** in Fournier's gangrene is rare due to the separate blood supply of the testes. - **Orchidectomy** is only performed if the testes themselves are affected by necrosis, which is uncommon and occurs in critically severe cases; routine removal is not indicated.
Question 5: A patient was brought to the ER following a road traffic accident. On examination, the patient opens his eyes to a painful stimulus, speaks inappropriately, and withdraws his limbs to a painful stimulus. What is his GCS score?
- A. E2V2M3
- B. E3V3M3
- C. E3V2M2
- D. E2V3M4 (Correct Answer)
Explanation: ***E2V3M4*** - Eye opening to **painful stimulus** scores 2 (E2). - Inappropriate speech scores 3 (V3). - Withdrawal from pain scores 4 (M4). *E2V2M3* - This option incorrectly assesses the **verbal response** and **motor response**. - Speaking incomprehensibly scores V2, while here the patient speaks inappropriately (V3). - Flexion to pain scores M3, but the patient exhibits withdrawal from pain (M4). *E3V3M3* - This option incorrectly assesses the **eye opening response**. - Eye opening to verbal command scores E3, but here the patient opens eyes to painful stimulus (E2). - The motor response is also incorrect, as M3 is flexion to pain, not withdrawal from pain (M4). *E3V2M2* - This option incorrectly assesses all three components of the **GCS score**. - A patient who opens eyes to a painful stimulus would score E2, not E3 (eyes opening to verbal command). - Both verbal (V3 for inappropriate speech, not V2 for incomprehensible sounds) and motor responses (M4 for withdrawal from pain, not M2 for extension to pain) are incorrectly scored.
Question 6: A 23-year-old male patient presents with midline swelling in the neck. The swelling moves with deglutition and protrusion of the tongue. What is the likely diagnosis?
- A. Brachial cyst
- B. Thyroglossal cyst (Correct Answer)
- C. Plunging ranula
- D. Dermoid cyst
Explanation: ***Thyroglossal cyst*** - A **thyroglossal cyst** is a congenital anomaly that arises from the persistent **thyroglossal duct**, a remnant of the thyroid's embryologic descent. - Its classic diagnostic feature is its movement with **deglutition** (due to attachment to the hyoid bone, which moves during swallowing) and **protrusion of the tongue** (as the thyroglossal duct is connected to the base of the tongue). *Brachial cyst* - A **brachial cyst** is a congenital neck mass that typically presents as a lateral neck swelling, often located along the anterior border of the **sternocleidomastoid muscle**. - Unlike a thyroglossal cyst, it does not typically move with **deglutition** or **tongue protrusion**. *Plunging ranula* - A **plunging ranula** is a type of mucocele that arises from the **sublingual gland** and extends below the mylohyoid muscle into the neck. - It presents as a cervical mass but is typically located in the floor of the mouth or submandibular region and does not move with **deglutition** or **tongue protrusion**. *Dermoid cyst* - A **dermoid cyst** is a congenital cyst that can occur anywhere on the body, including the head and neck, often presenting as a painless mass. - It arises from sequestered embryonic ectoderm and mesoderm, containing skin appendages, but it does not move with **deglutition** or **tongue protrusion**.
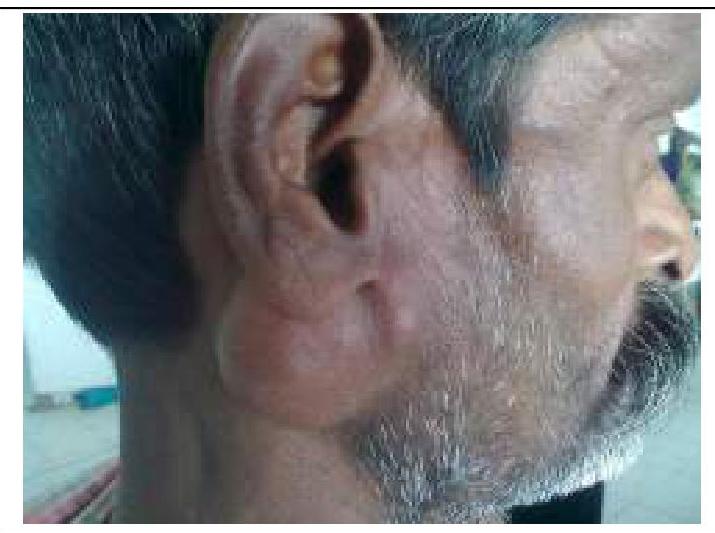
Question 7: What is the most likely diagnosis for the parotid mass with mixed consistency shown in the image?
- A. Pleomorphic adenoma (Correct Answer)
- B. Sebaceous cyst
- C. Dermoid cyst
- D. None of the options
Explanation: ***Pleomorphic adenoma*** - The **mixed consistency** of the parotid mass indicates a **benign tumor**, predominantly of epithelial and mesenchymal origin, typical of pleomorphic adenomas. - This type of tumor is usually **pain-free** and can exhibit a **soft** and **firm** texture on examination [1]. *Sebaceous cyst* - Typically presents as a **smooth, fluctuant nodule** and usually has a **firm consistency** rather than mixed. - Generally not seen as a parotid mass; usually found on the skin in areas with sebaceous glands. *Dermoid cyst* - Generally presents as a **well-defined, soft, and mobile mass**, not commonly associated with mixed consistency. - Often contains **keratin** and has a more homogenous consistency rather than the mixed characteristics of pleomorphic adenoma. *All* - As not all options are suitable for the description of a **mixed consistency parotid mass**, this option is incorrect. - Only **pleomorphic adenoma** aligns with the specific clinical presentation detailed in the question [1]. **References:** [1] Kumar V, Abbas AK, et al.. Robbins and Cotran Pathologic Basis of Disease. 9th ed. Head and Neck, pp. 751-753.
Question 8: In a patient with esophageal cancer and dysphagia affecting liquid intake, what is the most appropriate intervention to ensure nutritional support?
- A. Total parenteral nutrition
- B. Nasogastric tube feeding
- C. Esophageal stent placement
- D. Placement of a percutaneous endoscopic gastrostomy tube (Correct Answer)
Explanation: ***Placement of a percutaneous endoscopic gastrostomy tube*** - The question tests the principle that **gastrostomy tube feeding offers long-term nutritional support** for patients with esophageal obstruction and **dysphagia**, ensuring adequate caloric intake directly into the stomach. - Gastrostomy tubes are preferred over nasogastric tubes for **long-term feeding** (>4-6 weeks) due to better patient comfort, reduced risk of aspiration, and ease of care. - **Clinical Note:** In severe esophageal obstruction, a true PEG (percutaneous endoscopic gastrostomy) may not be technically feasible due to inability to pass the endoscope. In such cases, **radiologically inserted gastrostomy (RIG)** or **surgical gastrostomy** would be performed instead, but the principle of enteral feeding via gastrostomy remains the same. - The **functioning gastrointestinal tract** should always be utilized when possible (enteral feeding preferred over parenteral). *Total parenteral nutrition* - **TPN is reserved for patients with non-functional gastrointestinal tracts** or those who cannot tolerate enteral feeding, which is not applicable here as the stomach and intestines remain functional. - It carries **higher risks of infection, hepatic complications, metabolic derangements**, and is significantly more expensive compared to enteral feeding. - Following the principle: **"If the gut works, use it"** - enteral nutrition is always preferred when feasible. *Nasogastric tube feeding* - **Nasogastric tubes cannot be passed through an obstructing esophageal tumor** and are typically only suitable for short-term feeding (less than 4-6 weeks). - They are uncomfortable for patients and pose a **higher risk of aspiration pneumonia**. - Not appropriate for long-term nutritional support in malignancy. *Esophageal stent placement* - Esophageal stents are **palliative interventions primarily used to alleviate dysphagia** and restore oral intake in malignant obstruction. - While stents may allow some oral nutrition, they **do not guarantee adequate or reliable nutritional support**, especially as disease progresses. - Stents can lead to complications such as **tumor overgrowth, stent migration, fistula formation, or chest pain**, which may further compromise nutritional intake. - When the primary goal is **ensuring adequate nutritional support** rather than just relieving dysphagia, a feeding gastrostomy is more reliable.
Question 9: A patient presents with a gradually progressive, painless mass persisting for 10 years. The mass is firm to nodular and shows variable consistency within different areas of the swelling. What is the most probable diagnosis?
- A. Dermoid cyst
- B. Malignancy
- C. Sebaceous cyst
- D. Pleomorphic adenoma (Correct Answer)
Explanation: ***Pleomorphic adenoma*** - A **gradually progressive**, **painless mass** that has been present for 10 years, with a **firm to nodular** consistency and variability at different sites, is highly characteristic of a pleomorphic adenoma. - This benign tumor of salivary glands is known for its **slow growth** and **variable histological composition**, leading to its characteristic consistency. *Dermoid cyst* - Dermoid cysts are typically **present from birth** or early childhood and tend to be **soft and doughy** in consistency, rather than firm or nodular with variable consistency. - While painless, their growth pattern and texture differ from the described mass. *Malignancy* - A mass that has been present for **10 years** and is still described as **gradually progressive** but painless is less likely to be a malignancy, as most malignant tumors tend to grow more rapidly and often present with pain or other symptoms over such a long period. - Malignancies usually demonstrate a more infiltrative and aggressive growth pattern. *Sebaceous cyst* - A sebaceous cyst (epidermoid cyst) typically presents as a **smooth, movable, dome-shaped lump** and contains a cheesy, malodorous material, which is not consistent with a firm to nodular mass with varying consistency. - While they can be long-standing and painless, their characteristic feel and contents are different.