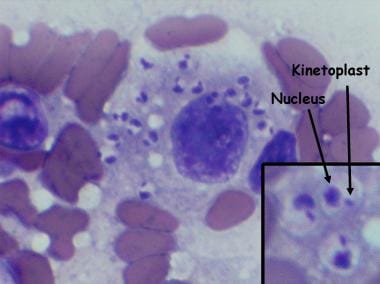
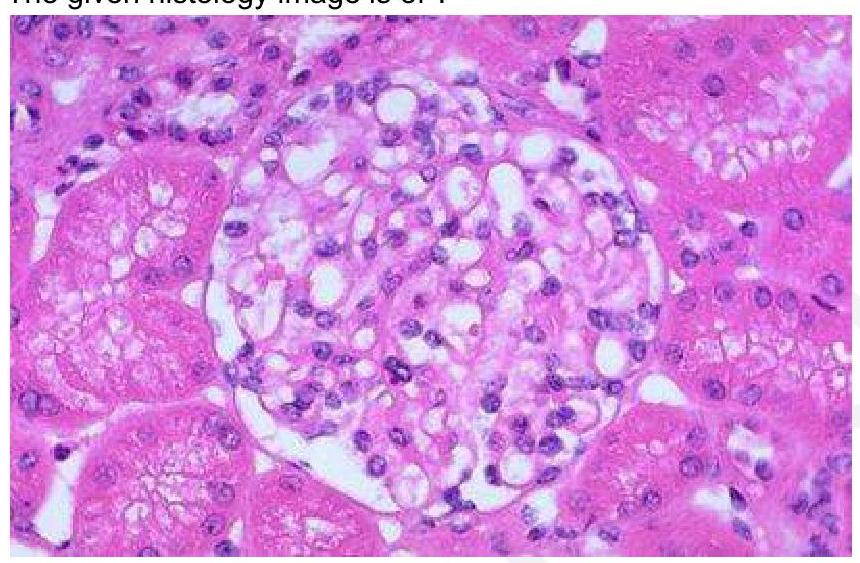
The given histology image is of which structure?
A patient is brought to the OPD by his wife, complaining about difficulty expressing emotions and lack of participation in daily activities. On examination, resting tremors and rigidity are noted. Given the possible diagnosis, which part of the brain is affected in this patient?