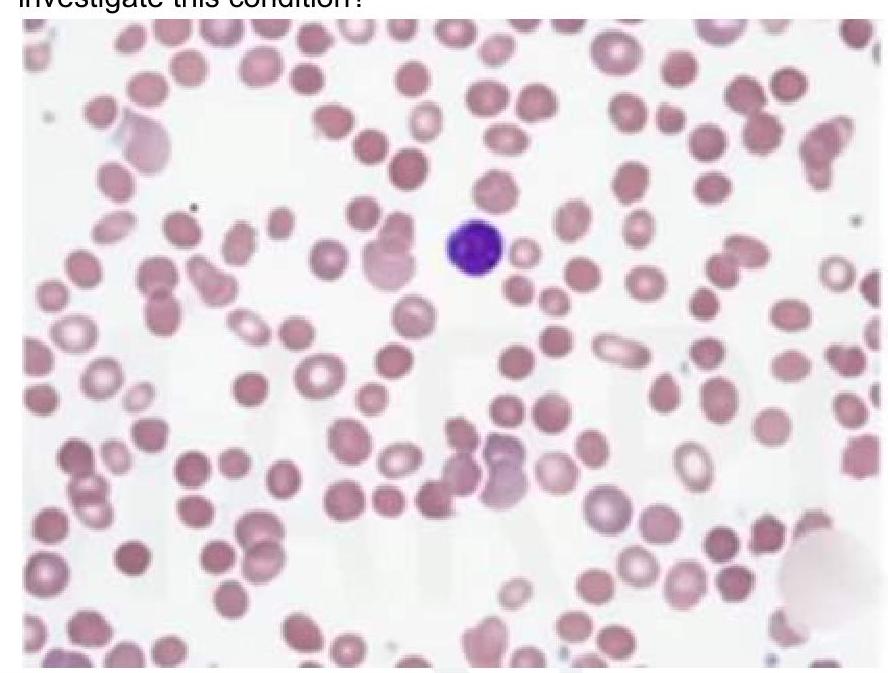
A child presents with intermittent jaundice and splenomegaly. There is a history of similar complaints in the elder brother. Peripheral smear shows the following finding. What is the most appropriate investigation for this condition?
A man presents with a history of dysuria and urethral discharge after having unprotected sexual intercourse. What is the treatment of choice for this infection?