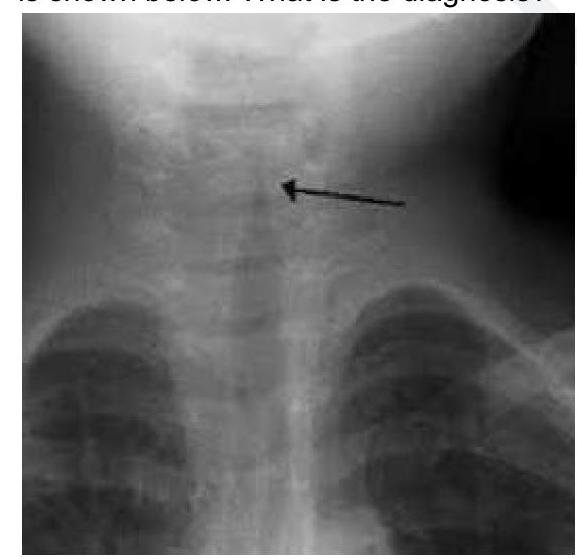
A 2 year child presented with low grade fever and stridor. What is the likely diagnosis?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
During acute tonsillitis, referred pain from the tonsil to the middle ear occurs via which nerve?
Which of the following is true about nerve injuries?
A 29-year-old patient presents with focal seizures. MRI shows frontal and temporal enhancement. What is the most probable diagnosis?
When resuscitating a patient in shock which of the following is not an adequate parameter to predict end point of resuscitation?
All the following nerves are involved in entrapment neuropathy except -
All of the following cause Fournier's gangrene except:
A swelling behind the ear suggests fracture of:
A child 10 yrs of age presents with a mass on his left thigh. The mass seems to be arising from the diaphysis of the femur and involving the soft tissue of the thigh. The child is having fever also. Give your most probable diagnosis -
A 2 year child presented with low grade fever and stridor. What is the likely diagnosis?

A patient presents with a gradually progressive, painless mass persisting for 10 years. The mass is firm to nodular and shows variable consistency within different areas of the swelling. What is the most probable diagnosis?