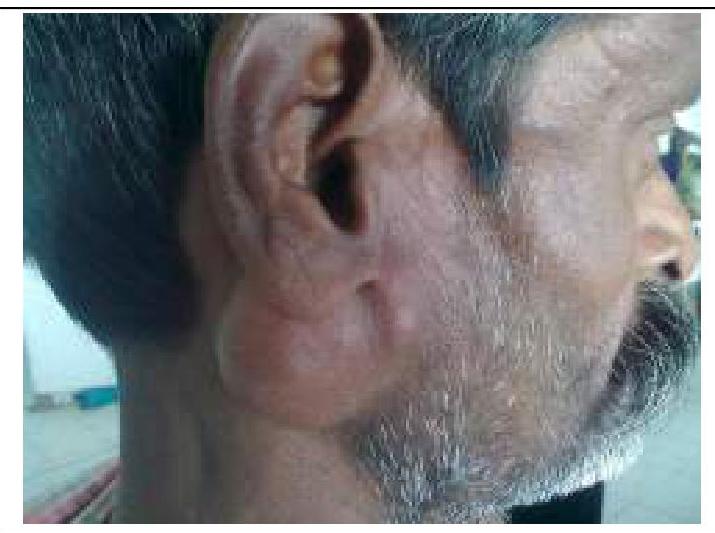
What is the most likely diagnosis for the parotid mass with mixed consistency shown in the image?
In a patient with esophageal cancer and dysphagia affecting liquid intake, what is the most appropriate intervention to ensure nutritional support?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Which of the following is a known risk factor for cholangiocarcinoma?
A patient presents with fever and jaundice after repairing sewers. What is the most appropriate test to diagnose the infection in this patient?
A 29-year-old primigravida presents at 36 weeks of gestation with a transverse lie. What is the recommended management?
Which of the following ocular findings is not associated with diabetes?
Which vitamin deficiency is most commonly associated with rickets in children?
A 2-year-old child with a history of eczema presents with a red, scaly rash around the mouth and extremities. A dietary history reveals excessive consumption of cow's milk. What nutritional deficiency is most likely?
Which of the following is NOT a side effect of amiodarone?
A patient presents with symptoms of muscle weakness and fatigue. Serum potassium levels are significantly elevated. How does hyperkalemia affect the resting membrane potential and action potential generation in neurons?
What is the most likely diagnosis for the parotid mass with mixed consistency shown in the image?

In a patient with esophageal cancer and dysphagia affecting liquid intake, what is the most appropriate intervention to ensure nutritional support?