NEET-PG 2023 — Microbiology
3 Previous Year Questions with Answers & Explanations
A boy presented with a fever and chills. Rapid test was positive for specific antigen HRP-2. Which of the following species of Plasmodium is the most likely causative agent?
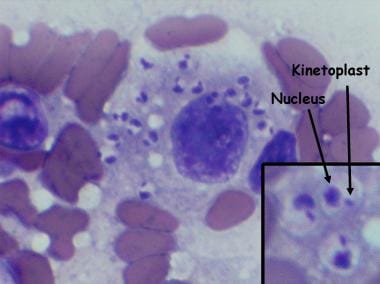
A lady from West Rajasthan presented with an ulcer surrounded by erythema on the right leg. Microscopy of the biopsy from the edge of the ulcer showed organisms with dark staining nuclei and kinetoplast. What is the most likely causative agent? (Refer to the provided image)
All of the following cause Fournier's gangrene except:
NEET-PG 2023 - Microbiology NEET-PG Practice Questions and MCQs
Question 1: A boy presented with a fever and chills. Rapid test was positive for specific antigen HRP-2. Which of the following species of Plasmodium is the most likely causative agent?
- A. Plasmodium falciparum (Correct Answer)
- B. Plasmodium malariae
- C. Plasmodium vivax
- D. Plasmodium ovale
Explanation: ***Plasmodium falciparum*** - The **histidine-rich protein 2 (HRP-2)** antigen is specifically produced by **P. falciparum** and is targeted by most rapid diagnostic tests for malaria. - A positive HRP-2 test in a patient with fever and chills indicates a high likelihood of **P. falciparum** infection, which is often the most severe form of malaria. *Plasmodium malariae* - **P. malariae** does not produce **HRP-2 antigen**, therefore, a rapid diagnostic test targeting HRP-2 would be negative for this species. - This species can cause a **quartan fever pattern** (fever every 72 hours) and usually presents with less severe symptoms compared to P. falciparum. *Plasmodium vivax* - **P. vivax** produces **_Plasmodium_ lactate dehydrogenase (pLDH)** and **aldolase antigens**, but not HRP-2. Some rapid tests combine detection of HRP-2 with pLDH to identify both *P. falciparum* and *P. vivax*. - While *P. vivax* causes fever and chills, its presence would not be indicated by a positive HRP-2 specific test alone. *Plasmodium ovale* - **P. ovale** also produces **pLDH and aldolase antigens**, similar to *P. vivax*, and does not produce **HRP-2**. - Infections with *P. ovale* are relatively rare and generally cause milder disease than *P. falciparum*, often with a **tertian fever pattern**.
Question 2: A lady from West Rajasthan presented with an ulcer surrounded by erythema on the right leg. Microscopy of the biopsy from the edge of the ulcer showed organisms with dark staining nuclei and kinetoplast. What is the most likely causative agent? (Refer to the provided image)
- A. Leishmania tropica (Correct Answer)
- B. Babesia microti
- C. Trypanosoma brucei
- D. Histoplasma capsulatum
Explanation: ***Leishmania tropica*** - The presence of an ulcer with surrounding erythema in **West Rajasthan**, along with microscopy showing organisms with a **nucleus and kinetoplast**, is highly characteristic of **cutaneous leishmaniasis** caused by *Leishmania tropica*. - The organisms seen are **amastigotes** within macrophages in skin lesions, which are identified by their distinct **nucleus and kinetoplast** on microscopy. - West Rajasthan is an **endemic area** for cutaneous leishmaniasis. *Babesia microti* - *Babesia microti* causes **babesiosis**, a tick-borne illness affecting red blood cells, leading to **hemolytic anemia** and malaria-like symptoms. - It does not typically cause **skin ulcers** and its characteristic form in smears is a **ring form or tetrad ("Maltese cross")** within red blood cells, not organisms with kinetoplasts in macrophages. *Trypanosoma brucei* - *Trypanosoma brucei* causes **African trypanosomiasis (sleeping sickness)**, presenting with fever, headaches, joint pain, and neurological symptoms, possibly a **chancre** at the inoculation site. - While it has a **kinetoplast**, it exists as a flagellated **trypomastigote** in the blood and CSF, not as an **amastigote** in macrophages within a skin ulcer. - Additionally, this is **geographically incorrect** for West Rajasthan. *Histoplasma capsulatum* - *Histoplasma capsulatum* is a **fungus** that causes **histoplasmosis**, primarily affecting the respiratory system, especially in immunocompromised individuals. - It does **not possess a kinetoplast** and while it can cause disseminated disease with skin lesions, the microscopic appearance would be **yeast forms** within macrophages, not organisms with kinetoplasts.
Question 3: All of the following cause Fournier's gangrene except:
- A. Bacteroides
- B. Clostridium (Correct Answer)
- C. Streptococcus
- D. Staphylococcus
Explanation: ***Clostridium*** - While *Clostridium* species (especially *C. perfringens*) **CAN be isolated** from Fournier's gangrene cases and contribute to gas formation and tissue necrosis, they are **less commonly identified as primary pathogens** compared to other organisms. - In the context of this question, *Clostridium* is considered the "except" option because it is **relatively less frequently implicated** in Fournier's gangrene compared to the other listed organisms, though it is NOT entirely excluded from the microbiology of this condition. - *Clostridium* species are more classically associated with **gas gangrene (clostridial myonecrosis)** in traumatic wounds and deep muscle tissue. *Bacteroides* - ***Bacteroides fragilis*** and other **anaerobic gram-negative bacilli** are among the **most commonly isolated organisms** in Fournier's gangrene. - They produce enzymes that facilitate tissue destruction and contribute significantly to the **polymicrobial synergistic necrotizing infection**. - Essential component of the typical microbial flora in perianal and genital infections. *Streptococcus* - ***Streptococcus pyogenes*** (Group A Streptococcus) and other streptococcal species are **frequently isolated** from Fournier's gangrene. - They produce toxins and enzymes causing **rapid necrotizing fasciitis** with systemic toxicity. - Major contributor to the aggressive nature and rapid progression of the infection. *Staphylococcus* - ***Staphylococcus aureus*** (including MRSA) is **commonly found** in polymicrobial Fournier's gangrene infections. - Contributes to local tissue destruction through toxin production and enzyme activity. - Often isolated from perianal and genital skin flora, facilitating its involvement in these infections.