A patient hailing from Delhi presents with fever, arthralgia, and extensive petechial rash for 3 days. Lab investigations revealed a hemoglobin of 9 g/ dL, a white blood cell count of 9000 cells/mm3, a platelet count of 20000 cells/mm3, and a prolonged bleeding time. The clotting time was normal. What is the most likely diagnosis?
A patient presents with polyuria following total hypophysectomy. Laboratory results show Na+ levels at 155 mEq/L and urine osmolarity at 200 mOsm/L. What is the definitive management for this patient?
A young patient presents with a large retroperitoneal hemorrhage and a history of intermittent knee swelling after strenuous exercise. There is no history of mucosal bleeding. Which of the following clotting factors is primarily deficient in Hemophilia A?
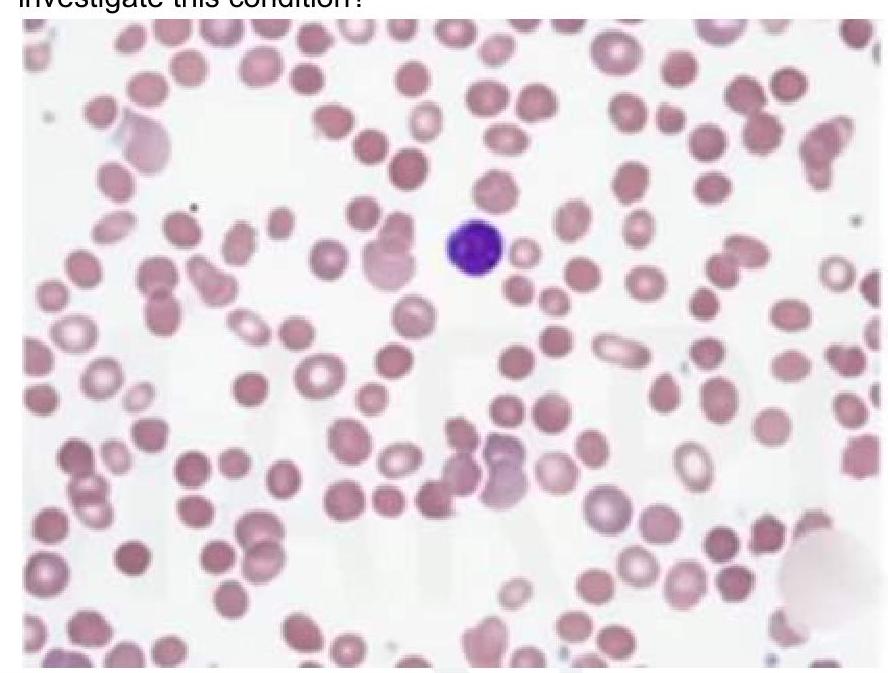
A child presents with intermittent jaundice and splenomegaly. There is a history of similar complaints in the elder brother. Peripheral smear shows the following finding. What is the most appropriate investigation for this condition?
A man presents with a history of dysuria and urethral discharge after having unprotected sexual intercourse. What is the treatment of choice for this infection?
A patient comes with abdominal pain, jaundice, and portal hypertension. Anastomosis between which of the following veins is seen?
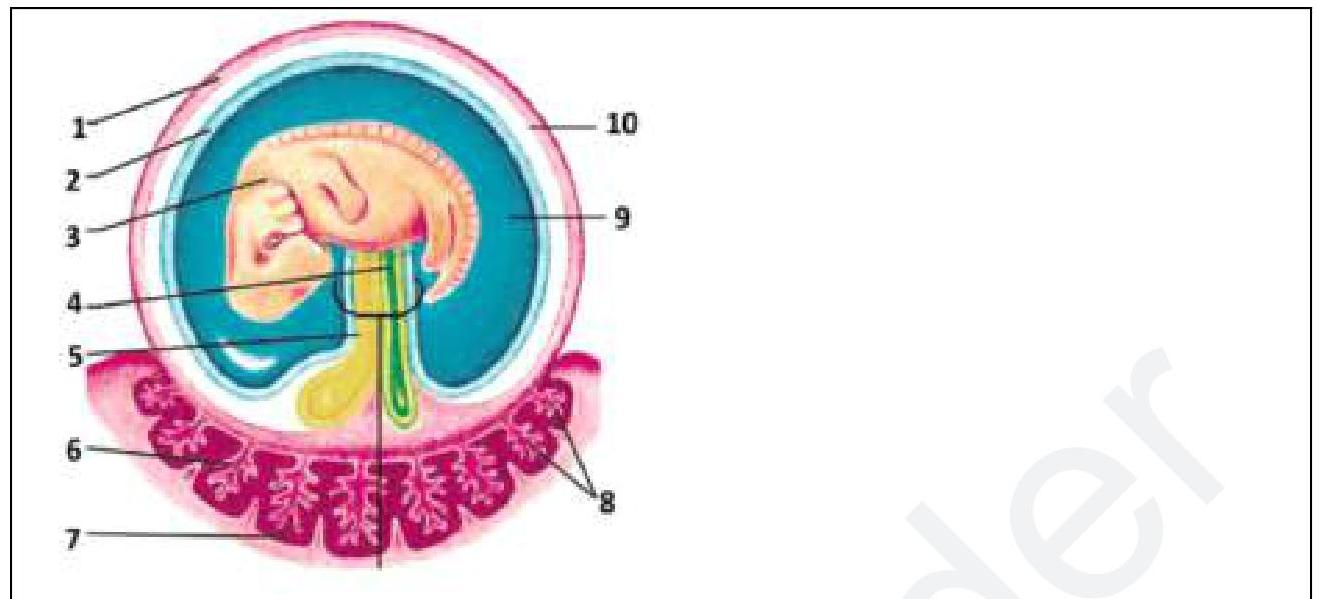
A young male came to the hospital with a clean-cut wound without any bleeding. The patient received a full course of tetanus vaccination 10 years ago. What is the best management for this patient?
In a patient presented with a fever and a positive filarial antigen test, what is the next appropriate method of management?
A bronchial asthma patient on inhalational steroids presented with white patchy lesions on the tongue and buccal mucosa. What condition is likely to be present in this patient?
A male patient presents with sensory loss and weakness of limbs for 3 months. He also has angular stomatitis. On examination, there is loss of proprioception, vibration sensations, UMN type of lower limb weakness, and absent ankle reflex. What is the most probable diagnosis?