NEET-PG 2023 — Biochemistry
7 Previous Year Questions with Answers & Explanations
A 45-year-old male patient presents to the emergency department with severe pain and swelling in the big toe joint. He has a history of recurrent joint pain and dietary indiscretion. A specimen from the affected joint is subjected to a test that produces a purple color reaction. What is the test being performed?
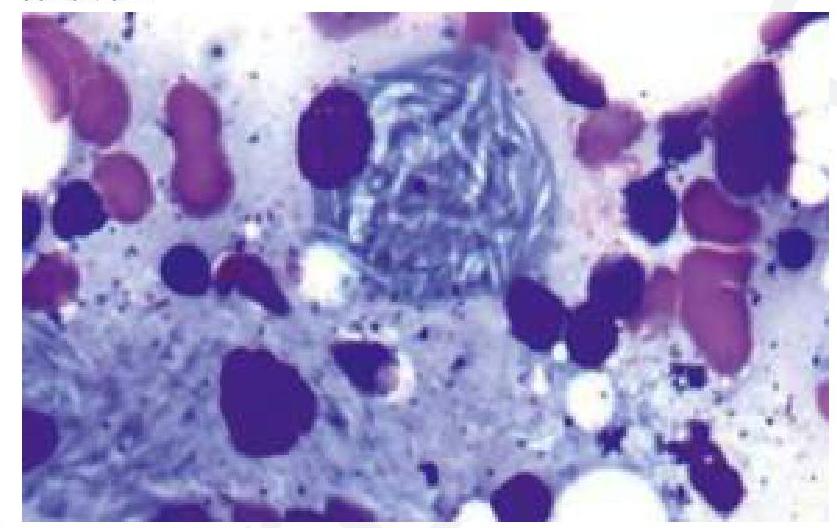
A child presents with bone pain and hepatosplenomegaly, indicative of Gaucher's disease. A trephine biopsy and aspirate show the following finding. Which of the following is the most likely enzyme deficient in this condition?
A newborn presented with chest retractions, dyspnea, and lethargy. The pediatrician diagnosed the baby with respiratory distress syndrome. This occurs due to the deficiency of:
A patient presenting with bleeding gums and easy bruisability was diagnosed with scurvy. This condition results from a deficiency of which of the following?
An infant is brought by his parents with complaints that his urine turns black on standing. Which of the following metabolic disorders is likely?
A family consumes only polished rice. Which of the following combinations of vitamin deficiency and enzymatic defect will be present in this family?
Enzyme activated by decrease in Insulin: glucagon ratio:
NEET-PG 2023 - Biochemistry NEET-PG Practice Questions and MCQs
Question 1: A 45-year-old male patient presents to the emergency department with severe pain and swelling in the big toe joint. He has a history of recurrent joint pain and dietary indiscretion. A specimen from the affected joint is subjected to a test that produces a purple color reaction. What is the test being performed?
- A. Florence test for choline compounds
- B. Teichmann test for blood
- C. Acid phosphatase test for prostate
- D. Murexide test for uric acid detection (Correct Answer)
Explanation: ***Murexide test for uric acid detection*** - The patient's presentation with **severe pain and swelling in the big toe**, recurrent joint pain, and dietary indiscretion is highly suggestive of **gout**, which is caused by the accumulation of **uric acid crystals**. - The **Murexide test** is a specific qualitative chemical test used to detect the presence of **uric acid** and its derivatives, yielding a characteristic **purple** color in the presence of uric acid. *Florence test for choline compounds* - The **Florence test** is used to identify **choline compounds**, primarily in forensic science for detecting **spermatozoa** by reacting with choline to form dark brown or black crystals. - While it involves a chemical reaction, its application and the compounds it detects are unrelated to the diagnosis of **gout** or uric acid. *Teichmann test for blood* - The **Teichmann test** (hemin test) is a microscopic chemical test used to confirm the presence of **blood** by detecting **hemin crystals**. - This test is not used for diagnosing joint conditions like gout or identifying **uric acid**. *Acid phosphatase test for prostate* - The **acid phosphatase test** measures the level of **acid phosphatase**, an enzyme mainly found in the **prostate gland**, and is used as a marker for **prostate cancer** or other prostatic conditions. - This test is entirely unrelated to the diagnosis of **gout** or the detection of **uric acid** in synovial fluid.
Question 2: A child presents with bone pain and hepatosplenomegaly, indicative of Gaucher's disease. A trephine biopsy and aspirate show the following finding. Which of the following is the most likely enzyme deficient in this condition?
- A. Hexosaminidase
- B. Glucocerebrosidase (Correct Answer)
- C. Sphingomyelinase
- D. Alpha 1,4-glucosidase
Explanation: ***Correct: Glucocerebrosidase*** - The clinical presentation of **bone pain**, **hepatosplenomegaly**, and the characteristic histological finding of **lipid-laden macrophages** (Gaucher cells) with a **crinkled paper** appearance in the bone marrow aspirate are highly suggestive of **Gaucher's disease**. - **Gaucher's disease** is caused by a deficiency of the lysosomal enzyme **glucocerebrosidase**, leading to the accumulation of **glucocerebroside**. *Incorrect: Hexosaminidase* - Deficiency of **hexosaminidase A** is associated with **Tay-Sachs disease**, which presents with neurological degeneration but typically **lacks hepatosplenomegaly** and bone pain. - The histological findings in Tay-Sachs disease would show neuronal storage of **GM2 gangliosides**, not Gaucher cells. *Incorrect: Sphingomyelinase* - Deficiency of **sphingomyelinase** causes **Niemann-Pick disease**, characterized by hepatosplenomegaly, neurological involvement, and interstitial lung disease, but the storage cells (foam cells) have a **foamy appearance** due to sphingomyelin accumulation, not the "crinkled paper" appearance of Gaucher cells. - While there is organomegaly, the distinct **histological features** in the image rule out Niemann-Pick disease. *Incorrect: Alpha 1,4-glucosidase* - Deficiency of **alpha 1,4-glucosidase** (acid maltase) causes **Pompe disease** (Glycogen Storage Disease Type II), which primarily affects muscle and liver with **glycogen accumulation**. - Pompe disease does not typically present with the same type of **bone pain** or the characteristic **Gaucher cells** seen in the image.
Question 3: A newborn presented with chest retractions, dyspnea, and lethargy. The pediatrician diagnosed the baby with respiratory distress syndrome. This occurs due to the deficiency of:
- A. Dipalmitoyl inositol
- B. Dipalmitoylphosphatidylethanolamine
- C. Lecithin (Correct Answer)
- D. Sphingomyelin
Explanation: ***Lecithin*** - **Respiratory distress syndrome (RDS)** in newborns is primarily caused by a deficiency of pulmonary **surfactant**. - **Lecithin (phosphatidylcholine)**, specifically in its dipalmitoyl form (**dipalmitoylphosphatidylcholine or DPPC**), is the main active component of surfactant, constituting ~40-50% of surfactant lipids. - DPPC is crucial for reducing surface tension in the alveoli and preventing their collapse during expiration. - This is the **primary biochemical deficiency** in neonatal RDS. *Dipalmitoyl inositol* - **Inositol** is a sugar alcohol involved in various cellular processes and is present in surfactant as phosphatidylinositol, but it is not a primary functional component. - Deficiency of this compound does not directly lead to **respiratory distress syndrome**. *Dipalmitoylphosphatidylethanolamine* - **Phosphatidylethanolamine (PE)** is a phospholipid found in cell membranes but is not the primary phospholipid responsible for surfactant function. - Note: This is PE, not PC (phosphatidylcholine). While PE is present in surfactant, its deficiency does not specifically cause **neonatal RDS**. *Sphingomyelin* - **Sphingomyelin** is a sphingolipid found in cell membranes and myelin sheaths, but it is not the critical component of pulmonary surfactant. - The **lecithin-to-sphingomyelin (L/S) ratio** is used to assess fetal lung maturity; an L/S ratio >2 indicates mature lungs capable of producing adequate surfactant.
Question 4: A patient presenting with bleeding gums and easy bruisability was diagnosed with scurvy. This condition results from a deficiency of which of the following?
- A. Inhibition of vitamin K
- B. Increased collagen breakdown
- C. Defective collagen synthesis
- D. Low vitamin C (Correct Answer)
Explanation: ***Low vitamin C*** - **Scurvy** is directly caused by a severe deficiency of **vitamin C (ascorbic acid)**. - Vitamin C is a cofactor for **prolyl hydroxylase** and **lysyl hydroxylase**, enzymes essential for **collagen synthesis**. - Its deficiency leads to defective collagen formation, resulting in weakened connective tissues and fragile capillaries, explaining the bleeding gums and easy bruising. *Inhibition of vitamin K* - **Vitamin K** is crucial for the synthesis of **blood clotting factors** (II, VII, IX, X). - Its inhibition (e.g., by warfarin) would lead to bleeding disorders but does not explain the characteristic connective tissue problems (poor wound healing, perifollicular hemorrhages) seen in scurvy. *Increased collagen breakdown* - Conditions like **Ehlers-Danlos syndrome** involve abnormal collagen structure leading to tissue fragility. - Scurvy is characterized by a problem in the *synthesis* rather than the increased *breakdown* of collagen. *Defective collagen synthesis* - While this describes the **pathophysiological mechanism** of scurvy, it is not the answer to what the patient is *deficient in*. - The question asks for the underlying **nutritional deficiency**, which is **vitamin C**—the root cause that leads to defective collagen synthesis.
Question 5: An infant is brought by his parents with complaints that his urine turns black on standing. Which of the following metabolic disorders is likely?
- A. Phenylketonuria
- B. Alkaptonuria (Correct Answer)
- C. Homocystinuria
- D. Maple syrup urine disease
Explanation: ***Alkaptonuria*** - **Alkaptonuria** is an autosomal recessive disorder characterized by a deficiency of **homogentisate 1,2-dioxygenase**, an enzyme involved in the metabolism of tyrosine. - The accumulation of **homogentisic acid** in tissues and urine causes the urine to turn black on standing due to oxidation. *Phenylketonuria* - **Phenylketonuria (PKU)** is caused by a deficiency of **phenylalanine hydroxylase**, leading to the accumulation of phenylalanine. - While it can manifest with intellectual disability and neurological symptoms, it does not typically cause the urine to turn black. *Homocystinuria* - **Homocystinuria** is a disorder of methionine metabolism, typically due to a deficiency of **cystathionine beta-synthase**. - It is characterized by intellectual disability, skeletal abnormalities, and lens dislocation, but not black urine. *Maple syrup urine disease* - **Maple syrup urine disease (MSUD)** results from a deficiency of **branched-chain alpha-keto acid dehydrogenase complex**, leading to the accumulation of branched-chain amino acids. - The distinguishing feature is urine that smells like maple syrup, not turning black.
Question 6: A family consumes only polished rice. Which of the following combinations of vitamin deficiency and enzymatic defect will be present in this family?
- A. Thiamine-transketolase (Correct Answer)
- B. Riboflavin-glutathione reductase
- C. Thiamine-transaminase
- D. Riboflavin-transketolase
Explanation: ***Thiamine-transketolase*** - Consumption of **polished rice** is a classic cause of **thiamine (vitamin B1) deficiency** because the polishing process removes the outer layers of the grain where thiamine is abundant. - **Transketolase** is a key enzyme in the **pentose phosphate pathway** that requires thiamine pyrophosphate (TPP) as a cofactor, making its activity a reliable indicator of thiamine status. *Riboflavin-glutathione reductase* - **Glutathione reductase** activity is indeed used to assess **riboflavin (vitamin B2) status**, as it requires FAD (a derivative of riboflavin) as a cofactor. - However, **riboflavin deficiency** is not characteristically associated with consumption of polished rice. *Thiamine-transaminase* - While this option correctly identifies **thiamine**, the associated enzyme, **transaminase**, is incorrect in this context. - **Transaminases** are primarily dependent on **pyridoxal phosphate (vitamin B6)** as a cofactor, not thiamine. *Riboflavin-transketolase* - This option incorrectly combines **riboflavin deficiency** with the enzyme **transketolase**. - As mentioned, **transketolase** activity is specifically used to assess **thiamine status**, not riboflavin status.
Question 7: Enzyme activated by decrease in Insulin: glucagon ratio:
- A. PFK
- B. Glucose 6 phosphatase (Correct Answer)
- C. Glucokinase
- D. Hexokinase
Explanation: ***Glucose 6 phosphatase*** - A decreased **insulin:glucagon ratio** signifies a catabolic state, promoting glucose release into the blood. - **Glucose-6-phosphatase** is the key enzyme in **gluconeogenesis** and **glycogenolysis** in the liver, dephosphorylating **glucose-6-phosphate** to **free glucose**, which can then be exported from the liver. *PFK* - **Phosphofructokinase (PFK)** is a key regulatory enzyme in **glycolysis**, which is inhibited in a state of low insulin:glucagon ratio. - Its activity would decrease, not increase, to reduce glucose utilization. *Glucokinase* - **Glucokinase** phosphorylates glucose to **glucose-6-phosphate** in the liver, trapping it for metabolism; its activity is increased by high insulin levels. - In a low insulin:glucagon ratio, its activity would be reduced to conserve glucose. *Hexokinase* - **Hexokinase** phosphorylates glucose in most peripheral tissues but has a lower Km for glucose than glucokinase, becoming saturated even at low glucose concentrations. - Its activity is not primarily regulated by the insulin:glucagon ratio; it is generally involved in glucose uptake for cellular energy needs.