NEET-PG 2023
133 Previous Year Questions with Answers & Explanations
Anatomy
1 questionsWhat embryological failure leads to the formation of a double aortic arch?
NEET-PG 2023 - Anatomy NEET-PG Practice Questions and MCQs
Question 1: What embryological failure leads to the formation of a double aortic arch?
- A. Failure of neural crest cell migration
- B. Abnormal development of the ductus arteriosus
- C. Failure of the 6th aortic arch to develop
- D. Failure of regression of the right dorsal aorta (Correct Answer)
Explanation: **Failure of regression of the right dorsal aorta** - A double aortic arch results from the **persistence of both right and left aortic arches** that encircle the trachea and esophagus, forming a vascular ring [1]. - In normal development, the **distal right dorsal aorta** (the segment between the right subclavian artery origin and the descending aorta) regresses, leaving only the left arch as the definitive aortic arch. - When this regression fails, both the right and left arches persist, creating a **complete vascular ring** around the trachea and esophagus, which can cause compression symptoms [1]. - This is one of the most common causes of a **symptomatic vascular ring** in infants [1]. *Failure of the 6th aortic arch to develop* - The 6th aortic arches contribute to the **pulmonary arteries** and the **ductus arteriosus**. Their failure to develop would lead to pulmonary circulation anomalies, not a double aortic arch. - This failure is associated with conditions like **pulmonary atresia** or **absent pulmonary artery**. *Abnormal development of the ductus arteriosus* - The ductus arteriosus is derived from the **distal part of the left 6th aortic arch**. Abnormal development typically leads to conditions like **patent ductus arteriosus (PDA)**. - This would not cause two complete aortic arches to persist around the trachea and esophagus. - While a right-sided ductus can be part of some vascular ring anomalies, it is not the primary cause of double aortic arch. *Failure of neural crest cell migration* - Neural crest cells are crucial for the **septation of the truncus arteriosus** and the formation of the aorticopulmonary septum. - Failure of neural crest cell migration is associated with conotruncal heart defects such as **Tetralogy of Fallot**, **Persistent truncus arteriosus**, or **Transposition of the Great Arteries**, not a double aortic arch. - Double aortic arch is primarily a failure of normal regression, not a neural crest cell defect.
Internal Medicine
3 questionsA 50-year-old HIV-positive patient presents with a painless, purple lesion on the skin. What is the most likely diagnosis?
In which of the following conditions is neoadjuvant chemotherapy not typically used?
Which of the following is a potential complication of blood transfusion?
NEET-PG 2023 - Internal Medicine NEET-PG Practice Questions and MCQs
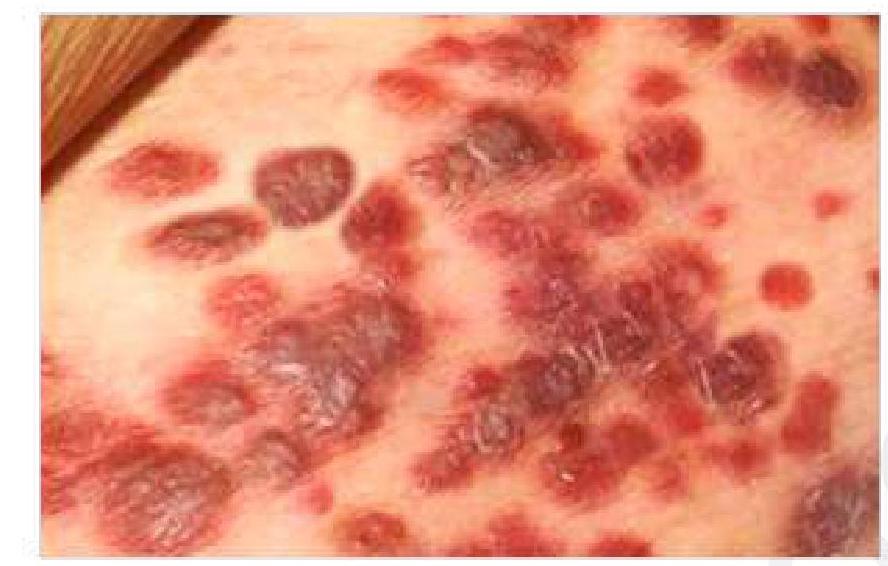
Question 1: A 50-year-old HIV-positive patient presents with a painless, purple lesion on the skin. What is the most likely diagnosis?
- A. Kaposi's sarcoma (Correct Answer)
- B. Squamous cell carcinoma
- C. Malignant melanoma
- D. Basal cell carcinoma
Explanation: ***Kaposi's sarcoma*** - The presentation of **painless, purple skin lesions** in an **HIV-positive patient** is highly characteristic of Kaposi's sarcoma. - This is a vascular tumor caused by **Human Herpesvirus 8 (HHV-8)**, often seen in immunocompromised individuals. *Malignant melanoma* - Malignant melanoma typically presents as a **dark, irregularly shaped lesion** with varying colors and often exhibits change in size, shape, or color over time (**ABCDEs of melanoma**). - While it can be purple or dark, the multiple, widespread nature and association with HIV points away from typical melanoma. *Squamous cell carcinoma* - Squamous cell carcinoma usually presents as a **red, scaly patch, nodule, or an open sore** that doesn't heal, often found in sun-exposed areas. - It is not typically described as a painless purple lesion, and while HIV patients have increased risk, the lesion morphology is more consistent with Kaposi's. *Basal cell carcinoma* - Basal cell carcinoma commonly appears as a **pearly or waxy bump**, a **flat, flesh-colored lesion**, or a **brown, scar-like lesion**, often with a rolled border and telangiectasias. - Unlike the description, it is not typically purple and painless, and while common, the clinical picture with HIV is not classic for BCC.
Question 2: In which of the following conditions is neoadjuvant chemotherapy not typically used?
- A. Thyroid cancer (Correct Answer)
- B. Breast cancer
- C. Esophageal cancer
- D. Lung cancer
Explanation: ***Thyroid cancer*** - **Neoadjuvant chemotherapy** is generally **not used** for the treatment of thyroid cancer, as it is primarily managed with surgery, radioactive iodine, and thyroid hormone suppression [1]. - Most thyroid cancers, especially differentiated types like **papillary** and **follicular carcinoma**, are not highly sensitive to conventional chemotherapy [1]. *Breast cancer* - **Neoadjuvant chemotherapy** is a common approach in **locally advanced breast cancer** to downstage tumors, improve surgical outcomes, and assess treatment response. - It may also be used in cases of **inflammatory** or certain aggressive subtypes like **triple-negative** breast cancer. *Esophageal cancer* - **Neoadjuvant chemotherapy**, often combined with **radiation** (chemoradiotherapy), is a standard treatment for **locally advanced esophageal cancer**. - Its purpose is to **downstage** the tumor, reduce invasiveness, and improve surgical resectability and survival rates. *Lung cancer* - **Neoadjuvant chemotherapy** is frequently employed for **locally advanced non-small cell lung cancer** (NSCLC) to reduce tumor size and extent before surgical resection. - This approach aims to improve the likelihood of a complete surgical removal and overall prognosis.
Question 3: Which of the following is a potential complication of blood transfusion?
- A. Hyponatremia
- B. Hypercalcemia
- C. Increased serum albumin
- D. Hyperkalemia (Correct Answer)
Explanation: ***Hyperkalemia*** - Stored red blood cells can release **intracellular potassium** into the storage solution, leading to elevated potassium levels in transfused blood. - Rapid or massive transfusions deliver a significant potassium load, potentially causing **cardiac arrhythmias**. *Hyponatremia* - This is generally not a direct complication of blood transfusions; instead, blood products themselves contain electrolytes, and massive transfusion can disrupt electrolyte balance, but usually not to cause hyponatremia. - Volume overload from transfusion could dilute existing electrolytes, but most commonly, other electrolyte imbalances such as hyperkalemia or hypocalcemia occur. *Hypercalcemia* - Often, the opposite, **hypocalcemia**, is a complication of massive transfusion due to **citrate toxicity**. - Citrate, an anticoagulant in transfused blood, chelates calcium, reducing free calcium levels in the recipient. *Increased serum albumin* - Blood transfusions primarily administer **red blood cells**, plasma, or platelets, not typically albumin in amounts that would significantly increase serum albumin levels in the absence of an albumin-specific infusion [1]. - Low albumin (hypoalbuminemia) is a common finding in critically ill patients, and a blood transfusion usually doesn't correct this unless plasma or albumin is specifically administered [1].
Pathology
2 questionsA primary structural defect of an organ resulting from an intrinsically abnormal developmental process is termed as:
A five-year-old girl is brought to a pediatrician because she is developing breasts. Physical examination shows large hyperpigmented macules with irregular margins on one side of her back. Which of the following bony abnormalities would most likely be associated with these symptoms?
NEET-PG 2023 - Pathology NEET-PG Practice Questions and MCQs
Question 1: A primary structural defect of an organ resulting from an intrinsically abnormal developmental process is termed as:
- A. Malformation (Correct Answer)
- B. Disruption
- C. Deformation
- D. Association
Explanation: ***Malformation*** - Refers to a **primary structural defect** present at birth, arising during development, leading to abnormal organ structure. - Typically involves intrinsic factors and can affect any organ or system, making it a key category of congenital anomalies. *Association* - Describes a **non-random occurrence** of two or more anomalies but does not indicate a structural defect of a specific organ. - Does not imply a direct defect, as it can occur without an **underlying structural issue** in a particular organ. *Deformation* - Refers to a change in the **shape or structure** of a normally formed organ or body part due to an external force rather than an intrinsic defect [1]. - Examples include clubfoot or positional plagiocephaly, which are not classified as malformations [1]. *Disruption* - Involves the breakdown of an originally normal tissue or organ due to extrinsic factors, leading to secondary structural defects. - Not inherent to the embryological development process itself, differentiating it from intrinsic faults like malformations. **References:** [1] Kumar V, Abbas AK, et al.. Robbins and Cotran Pathologic Basis of Disease. 9th ed. Diseases of Infancy and Childhood, pp. 460-462.
Question 2: A five-year-old girl is brought to a pediatrician because she is developing breasts. Physical examination shows large hyperpigmented macules with irregular margins on one side of her back. Which of the following bony abnormalities would most likely be associated with these symptoms?
- A. Excessive bony deposition with obliteration of marrow
- B. A combination of osteitis fibrosa cystica and osteomalacia
- C. A generalized thinning of bony spicules
- D. Multiple localized whorls of connective tissue (Correct Answer)
Explanation: ***Multiple localized whorls of connective tissue*** - This constellation of symptoms (precocious puberty, hyperpigmented macules with irregular margins, and bony abnormalities) is characteristic of **McCune-Albright syndrome** [1]. - The bony abnormality associated with McCune-Albright syndrome is **fibrous dysplasia**, which is characterized by the replacement of normal bone with **fibrous tissue** and immature woven bone, often described as localized whorls of connective tissue [1]. *A combination of osteitis fibrosa cystica and osteomalacia* - **Osteitis fibrosa cystica** is associated with severe **hyperparathyroidism**, leading to bone resorption and cyst formation. - **Osteomalacia** results from defective mineralization of bone due to **vitamin D deficiency** or phosphate wasting, neither of which comprehensively explains the given symptoms. *A generalized thinning of bony spicules* - This description is characteristic of **osteoporosis**, a condition of reduced bone mass and structural deterioration, leading to increased fracture risk. - Osteoporosis is typically seen in older adults and is not directly associated with precocious puberty or café-au-lait spots. *Excessive bony deposition with obliteration of marrow* - This describes **osteopetrosis** (Albers-Schönberg disease), a genetic disorder characterized by abnormally dense bones due to defective osteoclast function. - While it affects bone, its presentation does not include precocious puberty or hyperpigmented macules. **References:** [1] Kumar V, Abbas AK, et al.. Robbins and Cotran Pathologic Basis of Disease. 9th ed. Bones, Joints, and Soft Tissue Tumors, pp. 1208-1209.
Pediatrics
1 questionsA 4-year-old child is brought to the emergency department with severe dehydration due to diarrhea. What is the initial management for severe dehydration?
NEET-PG 2023 - Pediatrics NEET-PG Practice Questions and MCQs
Question 1: A 4-year-old child is brought to the emergency department with severe dehydration due to diarrhea. What is the initial management for severe dehydration?
- A. Oral rehydration therapy
- B. Intravenous fluids (Correct Answer)
- C. Antidiarrheal medication
- D. Antibiotics
Explanation: ***Intravenous fluids*** - For **severe dehydration**, rapid correction of fluid and electrolyte imbalances is critical, and **intravenous fluids** (normal saline or Ringer's lactate) are the **first-line treatment**. - As per **WHO and IAP guidelines**, children with severe dehydration require **IV fluid resuscitation** at 100 mL/kg over 3-6 hours (or 30 mL/kg bolus initially). - Signs of severe dehydration include **lethargy, sunken eyes, absent tears, very dry mucous membranes, poor skin turgor**, and inability to drink. - IV route ensures **rapid intravascular volume expansion** when oral intake is compromised or inadequate. *Oral rehydration therapy* - **ORT** is the treatment of choice for **mild to moderate dehydration only** (Plan B as per WHO). - In severe dehydration, children often have **altered consciousness, persistent vomiting**, or **circulatory compromise**, making oral intake ineffective or impossible. - ORT can be initiated once the child is alert and able to drink after initial IV resuscitation. *Antidiarrheal medication* - **Not recommended** in children with acute diarrhea, especially under 5 years. - Medications like loperamide can cause **ileus, drowsiness**, and may worsen outcomes. - They do **not address fluid and electrolyte deficits**, which is the immediate life-threatening concern. *Antibiotics* - Only indicated for **specific bacterial causes** (e.g., cholera, shigellosis with blood in stool, or proven invasive bacterial infection). - **Not part of initial management** for severe dehydration. - Indiscriminate use contributes to **antibiotic resistance** and delays critical rehydration.
Pharmacology
1 questionsClaviceps purpurea produces which of the following toxins?
NEET-PG 2023 - Pharmacology NEET-PG Practice Questions and MCQs
Question 1: Claviceps purpurea produces which of the following toxins?
- A. Ergot alkaloids (Correct Answer)
- B. Aflatoxins
- C. Sanguinarine alkaloid
- D. Pyrazolidone drug
Explanation: ***Ergot alkaloids*** - **Claviceps purpurea** is a fungus that infects cereals, particularly rye, and produces a group of toxic compounds known as **ergot alkaloids**. - These alkaloids can cause a condition called **ergotism**, which includes symptoms like hallucinations, gangrene, and severe vasoconstriction. *Aflatoxins* - **Aflatoxins** are produced by species of **Aspergillus fungi**, such as *A. flavus* and *A. parasiticus*, not *Claviceps purpurea*. - They are potent **carcinogens** and are commonly found in contaminated crops like peanuts and maize. *Sanguinarine alkaloid* - **Sanguinarine** is an alkaloid derived from plants like **bloodroot (Sanguinaria canadensis)**, not *Claviceps purpurea*. - It has been linked to **glaucoma** and liver toxicity. *Pyrazolidone drug* - **Pyrazolidone** is a classification of synthetic drugs, often used as **non-steroidal anti-inflammatory drugs (NSAIDs)**, such as phenylbutazone. - This is a pharmaceutical compound and not naturally derived from *Claviceps purpurea* or any fungus.
Physiology
2 questionsWhich substance has the least renal clearance?
Following occurs in living cells only:
NEET-PG 2023 - Physiology NEET-PG Practice Questions and MCQs
Question 1: Which substance has the least renal clearance?
- A. Glucose (Correct Answer)
- B. Inulin
- C. Urea
- D. Creatinine
Explanation: ***Glucose (Correct Answer)*** - Under normal physiological conditions, **glucose is almost completely reabsorbed** in the proximal tubule of the nephron, leading to a **renal clearance of nearly zero**. - While glucose is freely filtered by the glomerulus, the extensive reabsorption mechanisms (via SGLT2 and SGLT1 transporters) ensure that virtually no glucose appears in the urine under normal circumstances. - This makes glucose the substance with the **least renal clearance** among the given options. *Inulin (Incorrect)* - **Inulin** is freely filtered by the glomerulus but is neither reabsorbed nor secreted by the renal tubules. - Its renal clearance equals the **glomerular filtration rate (GFR)** (~125 mL/min), making it an ideal marker for GFR measurement. - Inulin has a **much higher clearance than glucose**. *Urea (Incorrect)* - **Urea** is filtered by the glomerulus, and approximately **50% of the filtered urea** is reabsorbed in the renal tubules, primarily in the proximal tubule and medullary collecting duct. - Its clearance (~60-70 mL/min) is lower than GFR but still **significantly higher than glucose clearance**. *Creatinine (Incorrect)* - **Creatinine** is freely filtered by the glomerulus and is also **secreted by the renal tubules** (approximately 10-20% secreted). - This secretion means its renal clearance (~130-140 mL/min) is slightly **higher than the actual GFR**. - Despite this, creatinine is commonly used as an estimate of GFR due to its relatively stable production and ease of measurement.
Question 2: Following occurs in living cells only:
- A. Simple diffusion
- B. Facilitated diffusion
- C. Osmosis
- D. Active transport (Correct Answer)
Explanation: ***Active transport*** - **Active transport** requires energy (ATP) to move substances against their concentration gradient, a process only possible in **living cells** that can produce ATP. - This process is crucial for maintaining cellular homeostasis, accumulating nutrients, and removing waste, all of which are vital functions of **living organisms**. *Simple diffusion* - **Simple diffusion** is the passive movement of substances across a membrane from an area of higher concentration to lower concentration, without the need for energy or membrane proteins. - This process can occur in **both living and non-living systems**, as it is driven by random molecular motion and concentration gradients. *Facilitated diffusion* - **Facilitated diffusion** involves the passive movement of molecules across a membrane with the help of **transport proteins** (channels or carriers) but still moves down the concentration gradient without direct energy expenditure. - While it uses proteins, these proteins can sometimes function in **isolated membrane systems** even if the cell is not metabolically active (e.g., in a cell lysate). *Osmosis* - **Osmosis** is the specific type of diffusion involving the net movement of **water molecules** across a selectively permeable membrane, driven by differences in solute concentration. - Similar to simple diffusion, osmosis is a **physical process** based on water potential gradients and can occur in both **living and non-living membranes** given the right conditions.
About NEET-PG 2023 Questions
This page contains 133 questions from the NEET-PG 2023 paper, organised across 20 subjects for focused practice. Every question comes with the correct answer and a detailed explanation to help you understand the underlying concept. Subject-wise organisation lets you target specific areas and identify which topics carried the most weight in this particular year.
Practising year-wise papers is essential for understanding how the NEET-PG exam evolves — you can spot trending topics, gauge difficulty shifts, and benchmark your readiness against a real paper. To take your preparation further, download the Oncourse app for AI-driven performance insights, spaced repetition of questions you got wrong, and a personalised study plan built around your NEET-PG goals.