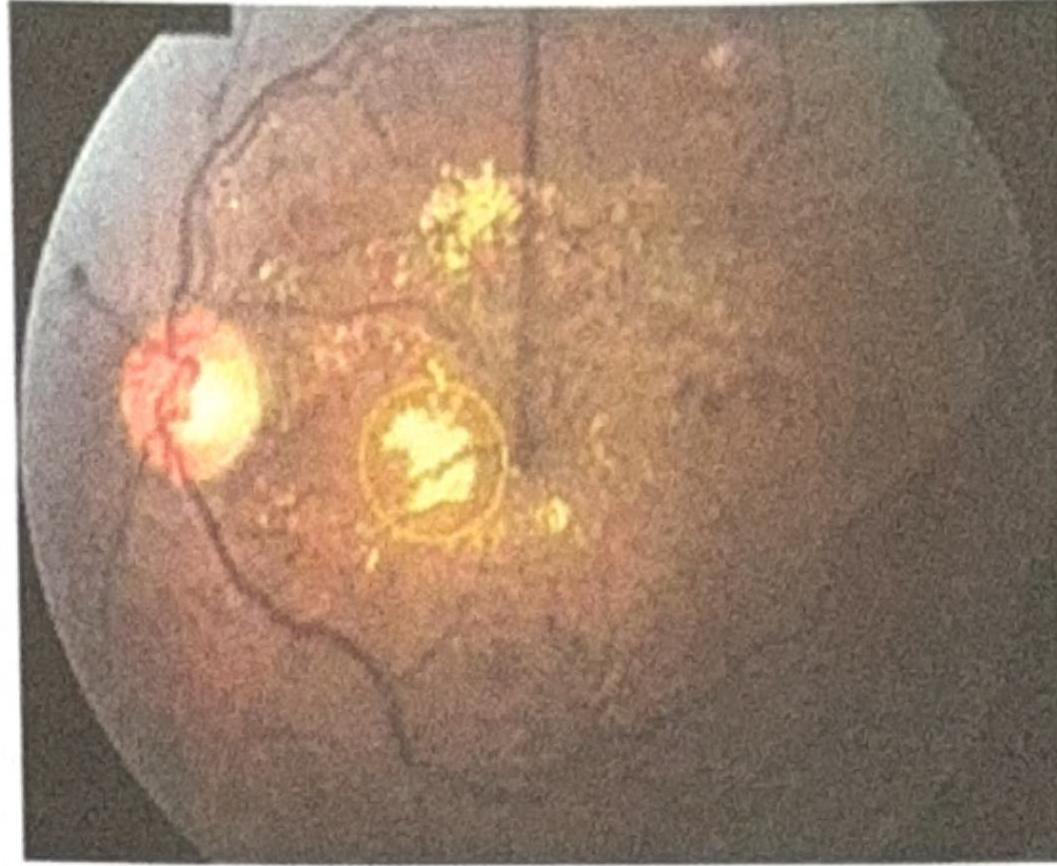
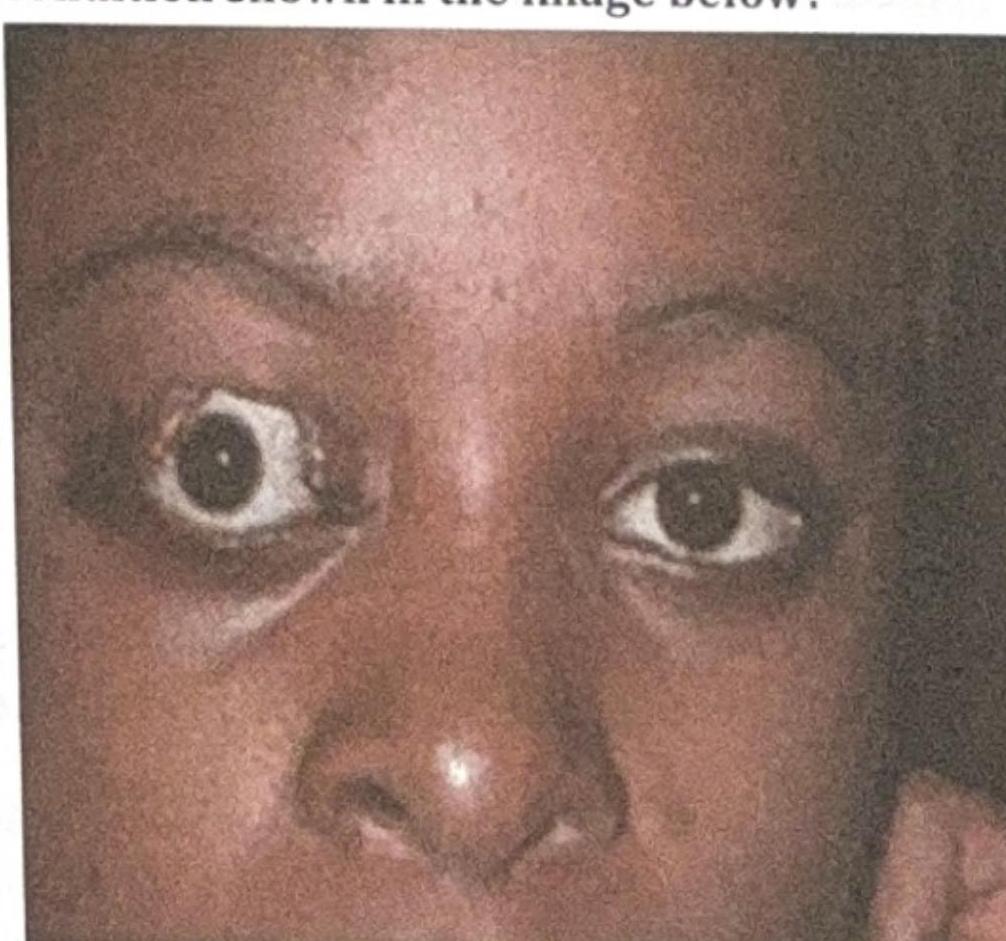
A 33-year-old female patient presents with an inability to see the right side from both eyes (right homonymous hemianopia). What is the most probable cause?
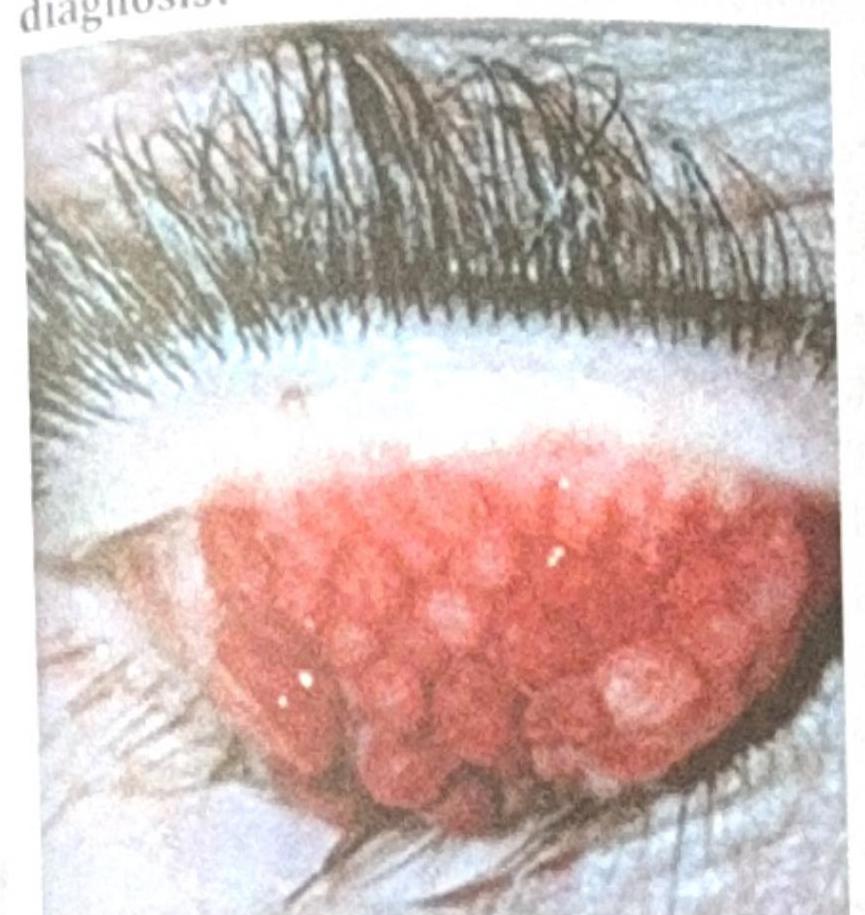
A patient complained of gradual diminution of vision. On examination, the patient had dry eyes and a rough corneal surface. What deficiency is most likely causing these manifestations?
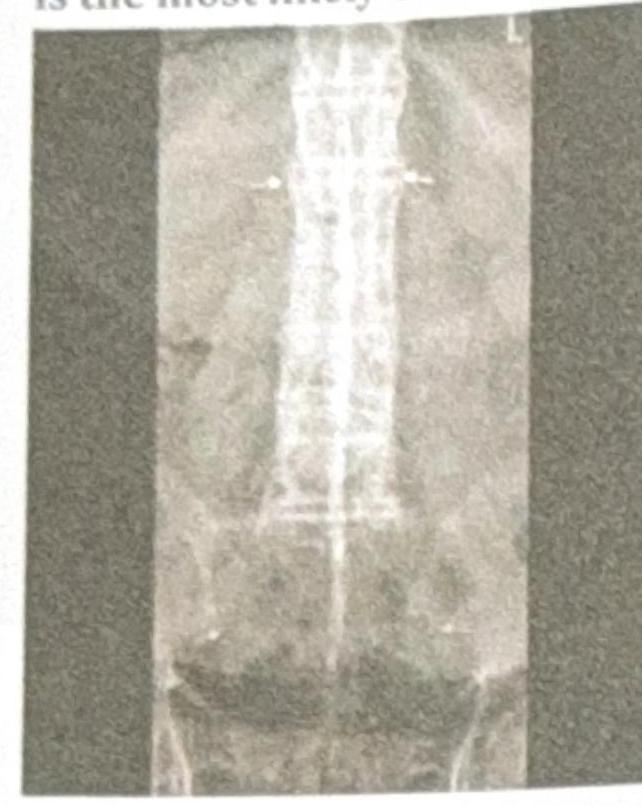
A young male presents with acute redness of the eye. His X-ray of the spine is shown below. What is the most likely condition?