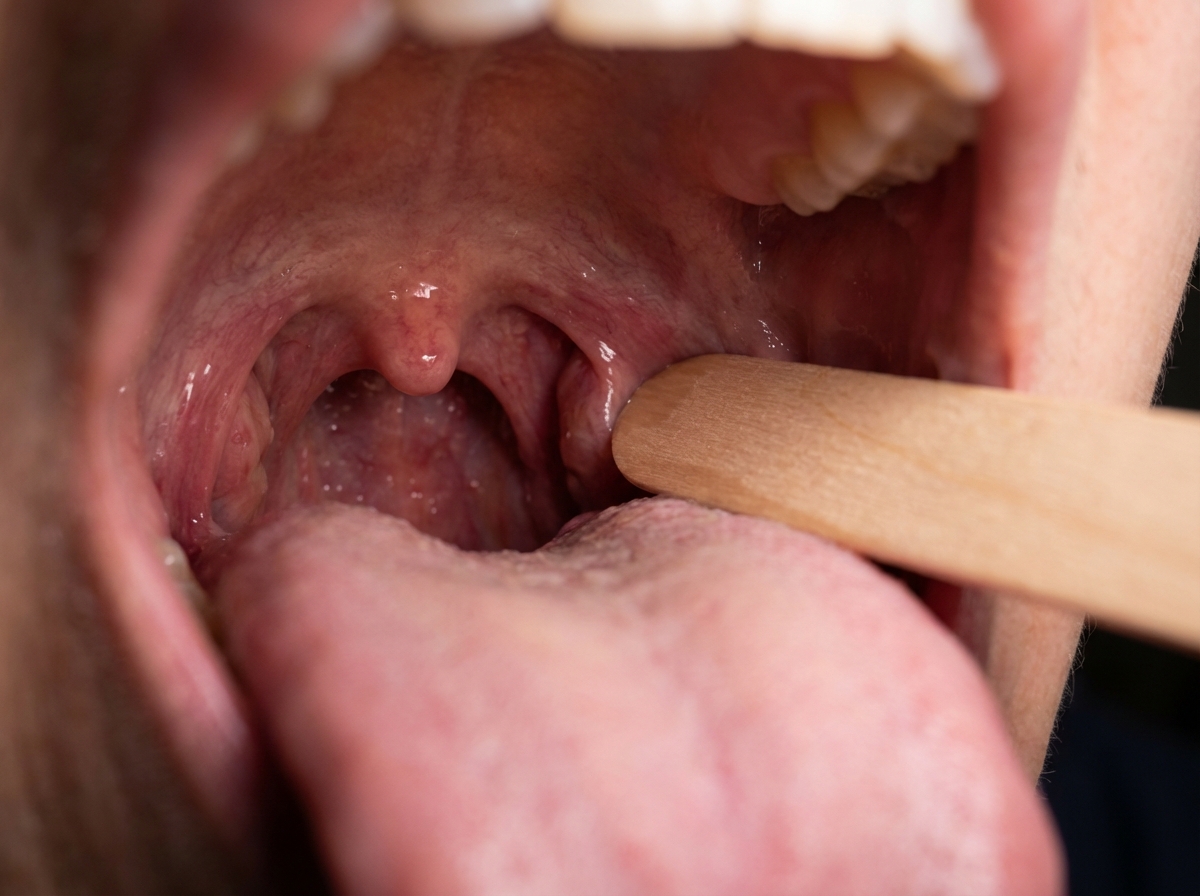
A patient was admitted with skull base trauma. The doctor was testing the marked structure in the pharyngeal region. Which of the following nerves was being tested?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A patient was admitted with skull base trauma. The doctor was testing the marked structure in the pharyngeal region. Which of the following nerves was being tested?

A child is learning the steps of hand hygiene. Which domain of learning is primarily involved?
A 55-year-old patient from Chhattisgarh presents with progressive muscle weakness, stiffness of both lower limbs, and complete paralysis. What is the most important history that should be asked?
A woman visits the ENT outpatient department with complaints of nasal obstruction. On examination, greenish-black crusts were found in the nasal cavity covering the turbinates and septum, and she also had complete anosmia (lack of sense of smell). What other sign is most likely to be found on examination in this case?
A child who underwent a tonsillectomy started bleeding while lying in the ward post-operatively. Which of the following is the most appropriate management step?
A patient with a history of chronic ear infection now presents with manifestations, including headache and vomiting. A CT brain image is shown. What is the most probable diagnosis?

What is the SI unit of illuminance (brightness of light on a surface)?
Which transporter is responsible for the absorption of glucose in the intestine when a person is given Oral Rehydration Solution (ORS)?
A 35-year-old male presents with posterior epistaxis. Conservative management including nasal packing to stop the bleeding was unsuccessful. What is the next step in the management of this patient?
Which of the following is a common topical use of the medicine shown in the image?
