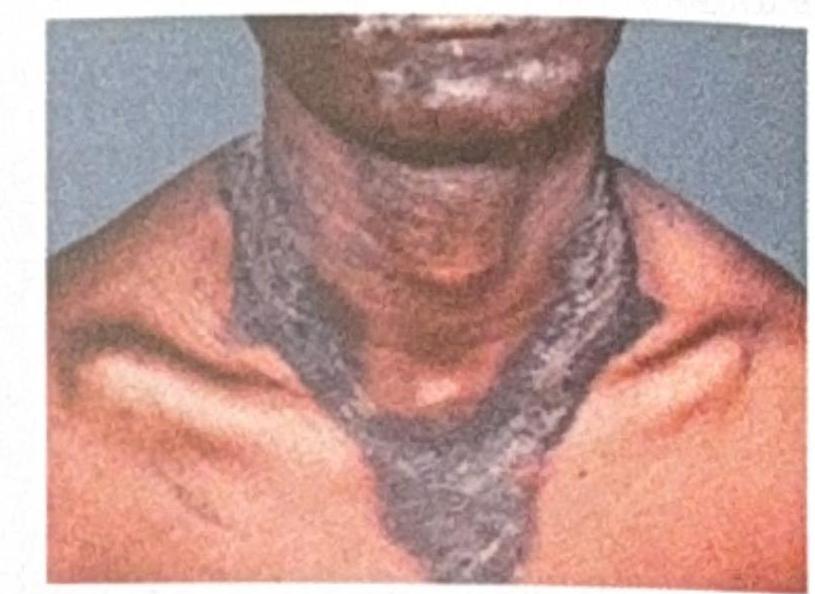
A 45-year-old man presents with the following skin changes (as shown in the image). What relevant history should be taken to diagnose this condition?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A farmer complains of a skin rash that worsens with sun exposure and redness of the tongue. Maize is the staple in his diet. Which vitamin deficiency is likely responsible for these symptoms?
There is an outbreak of buboes in a community. What is the vector responsible for transmitting the causative agent?
Which of the following is not included in the Global Hunger Index?
In a 10-year-old school child under the school health program, which vaccine should be administered?
A 45-year-old man presents with the following skin changes (as shown in the image). What relevant history should be taken to diagnose this condition?

A child presented with bluish-white spots in the mouth followed by a rash. What is the genome of the most likely causative agent?
An 11-year-old girl is experiencing symptoms of fever and sore throat, and a throat swab was taken for culture. After the culture, which bag should be used to discard the swab?
A 16-month-old child weighing 8 kg is assessed using a growth chart. The child's weight falls between the median (standard) and minus 2 standard deviations ( -2 SD ). What should be the next step in the management of this child?
An anganwadi teacher measures the weight and height of a 4-year-old child and finds that the child's height-for-age is below the normal percentile. What does this finding indicate?
A girl child has had recurrent yeast and respiratory viral infections since she was 3 months old. Considering studies for her immune status, which of the following vaccines is contraindicated?