A truck driver presented with a painless, demarcated ulcer on the penis and inguinal lymphadenopathy. What is the best method to visualize the motility of the most likely causative agent?
A patient was suspected of having brucellosis. A serum sample was sent for a standard agglutination test, which was initially negative but became positive after dilution of the sample. What is the most likely reason for the initial negative test?
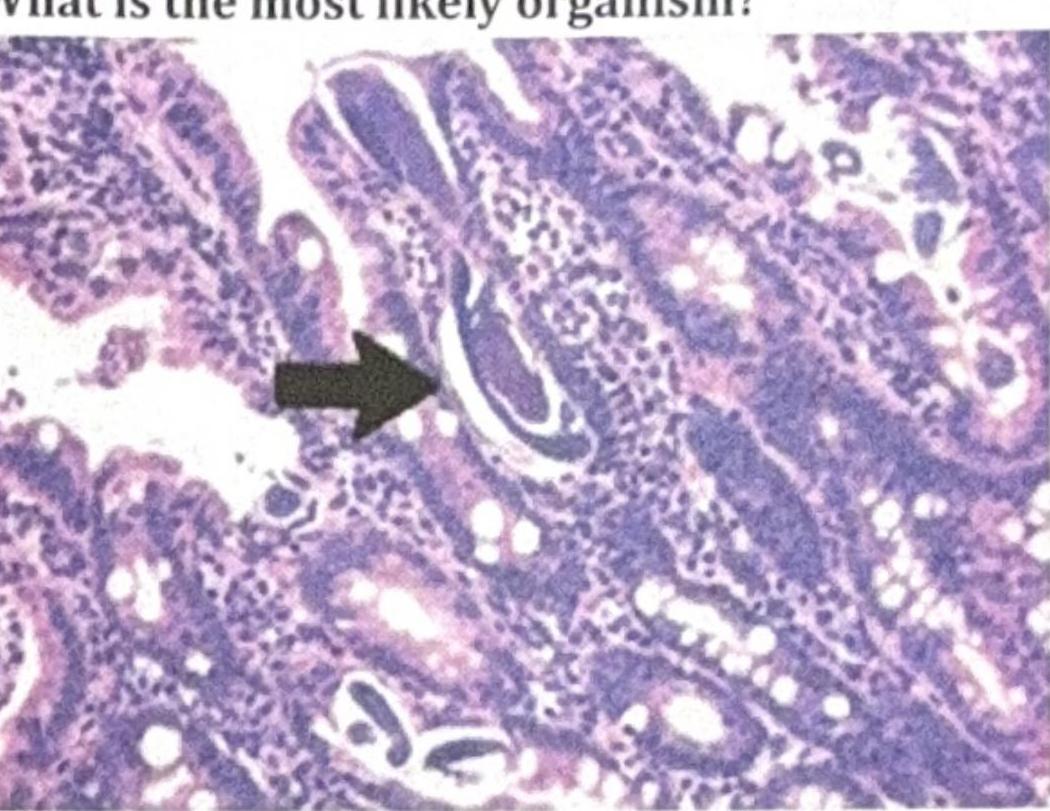
A patient on steroids presented with nocturnal cough and chronic urticaria. Bronchoalveolar lavage (BAL) staining was done, and the organism shown in the image was identified. What is the most likely organism?
A child presented with bloody stools and abdominal pain. Which enrichment medium should be used for processing the fecal sample?
What is the vector for Leishmania, a parasite characterized by a prominent kinetoplast in its morphological forms?